Physical Therapy Guide to Hyperkyphosis (Humpback)
Hyperkyphosis is a spinal deformity causing a forward-curved posture of the upper back (thoracic spine). Posture is the way you position your body. Posture changes throughout the day depending on what you are doing and how long you have been doing it. Sometimes, a person's posture can cause the upper back curvature to become excessive and stiff. When this happens, it can be difficult to reverse. Sometimes called "humpback," "round back," or "dowager’s hump,” this condition can occur at any age. Most often, the curvature begins to increase in people over age 40 and continues as they age. Around 20% to 40% of older adults — both men and women — will develop the condition. Physical therapists help people with hyperkyphosis:
- Address functional limitations.
- Build strength.
- Improve balance.
They also may help people prevent the condition from getting worse and in some cases reduce hyperkyphosis.
Physical therapists are movement experts. They improve quality of life through hands-on care, patient education, and prescribed movement. You can contact a physical therapist directly for an evaluation. To find a physical therapist in your area, visit Find a PT.
What Is Hyperkyphosis?
Hyperkyphosis is a spinal deformity. It occurs when the natural forward-curving shape of the upper back becomes extreme. It leads to rounded shoulders with a head-forward posture (where the head and neck are forward of the trunk). People with this condition often have difficulty standing up straight. A worsening curvature increases the risk of health problems. These can include back and neck pain, spinal fractures, breathing difficulties, and falls.
Hyperkyphosis can result from conditions such as:
- Osteoporosis (bones with low density).
- Fractures of the vertebrae due to low bone density.
- Scheuermann's disease (juvenile kyphosis): excessive curvature of the upper back that appears in childhood.
If no fractures are present, other suspected causes for the deformity include:
- Poor posture habits.
- Muscle weakness.
- Degenerative disk disease.
- Arthritis.
- Ligament degeneration.
- Family history of the condition.
Signs and Symptoms
The most prominent symptom of hyperkyphosis is a rounded upper back.
- You may not notice the changes in your back posture because in most cases, the curve develops gradually. Friends and family may notice it before you do.
- Other subtle signs can include:
- Changes in how your clothes fit.
- Feeling like it takes a lot of effort to stand or sit up straight.
- Fatigue during walking and other activities.
Caution: If you notice a sudden increase in the curvature of your back, call your doctor. A sudden change in the curve of the spine could be a sign of other health problems.
If left untreated, hyperkyphosis can cause:
- Difficulty doing everyday tasks such as bathing, getting out of a chair, reaching overhead, bending, or walking. It also may take more energy to complete common tasks.
- Decreased flexibility and strength of the trunk muscles.
- Changes in the body’s center of gravity.
- Balance problems (due to the change in center of gravity) that can increase the risk of falls and injury.
- Upper back pain or pain between the shoulder blades.
- Spinal fractures as the condition advances.
If you have advanced hyperkyphosis, you may experience:
- Difficulty breathing, even without a history of lung or heart disease.
- A lessening of the distance between your lowest ribs and your pelvic bones. In this case, pulmonary function tests may be prescribed to measure whether your curvature is restricting your breathing.
How Is It Diagnosed?
A visual inspection of your back is the first assessment for hyperkyphosis. Your physical therapist or doctor may measure your spinal curve using a flexible ruler. They also may order an X-ray and a radiologist will measure the spinal angles on the images. Hyperkyphosis is diagnosed if a curve measures greater than 40 degrees.
Sometimes spinal changes occur because of fractures due to thinning bones or osteoporosis. Spinal changes also can result from degenerative disk disease or arthritis. These are common aging-related problems.
Problems not linked with aging also can cause a sudden change in posture. A tumor, infection, or neurologic changes can cause hyperkyphosis but are not common. If needed, X-rays or an MRI can show whether any of these less common conditions are affecting your posture.
Advanced Hyperkyphosis
If your curvature is severe, you may have difficulty breathing, even without heart or lung disease. You also may notice pain at your waistline, or the distance between your lowest ribs and your pelvic bones becoming less. If so, your health care provider may prescribe tests to measure whether your condition restricts your breathing.
How Can a Physical Therapist Help?
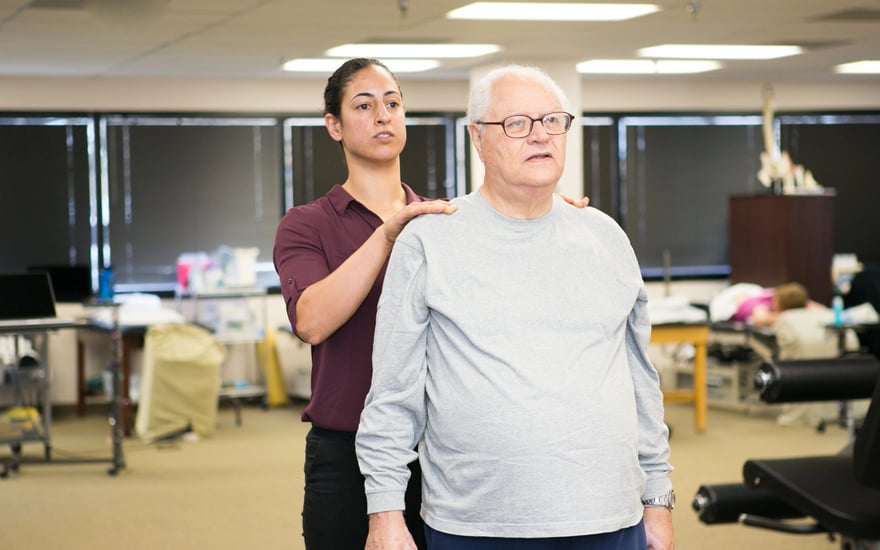
A physical therapist can help you with your pain and address changes in your posture to help prevent worsening. They also will work with you to address any functional limitations, loss of strength, or balance problems.
Your physical therapist will first review your medical history, including any medications you take.
Note: Any sudden rounding of your back may point to a more serious health problem. Your physical therapist will refer you to your primary care provider if you report:
- A sudden change in your posture.
- Severe pain.
- A major change in function.
Your physical therapist will perform special tests to assess your condition. They will begin by measuring your:
- Postural alignment.
- Functional strength.
- Range of motion.
- Balance.
- Flexibility.
If you have problems walking or keeping your balance, your physical therapist will perform additional tests. They also will assess whether you have an increased risk of falling. Your physical therapist will design a treatment program to address your specific needs and goals. Your treatment may include:
- Postural alignment training, stretching, and strengthening exercises. These exercises can help reduce the spinal curvature, decrease your pain, and prevent your condition from getting worse. Doing the prescribed exercises in the clinic and at home is essential for success. You can lessen or slow the progression of your curve by improving how you sit, stand, and do daily activities.
- Balance exercises and walking (gait) training. These treatments will help increase your tolerance for activity. They also can improve your safety by reducing your risk of falls.
- Education. Your physical therapist will teach you ways to improve how you do your daily activities. For example, they can teach you how to safely get in and out of a bed, a chair, or a bathtub. They also can help you learn how to bend and walk with more ease.
- Breathing exercises. These can help you improve your tolerance for physical activity by increasing your lung capacity.
- Manual (hands-on) therapy. Your physical therapist may use gentle techniques to massage or reduce stiffness in your muscles and soft tissues. They also may mobilize your joints using gentle movements to help improve spinal flexibility.
- Specialized braces or therapeutic taping. These methods may help reduce the angle of your upper-back curve.
- Pain management. Your physical therapist may use heat, ice, and/or electrical stimulation to help reduce your pain. They will choose the right treatment that will help you most — and help reduce your need for pain medication, such as opioids.
All cases of hyperkyphosis are different. Your physical therapist will choose the best treatment options for you based on your specific condition.
Can This Injury or Condition Be Prevented?
Research shows that you can reduce hyperkyphosis by:
- Maintaining and improving posture.
- Strengthening the spine.
- Achieving and maintaining physical fitness.
Taking these actions also can help prevent the condition worsening with the normal aging process. However, there is no evidence that hyperkyphosis can be prevented.
Altering some daily activities also may help you avoid the worsening of hyperkyphosis. Your physical therapist may teach you how to:
- Lift or carry heavier objects safely.
- Avoid bending too far from the waist or twisting your trunk too far.
- Keep your posture upright when you cough or sneeze: avoid looking down or bending forward.
- Avoid exercises that involve bending forward at the waist or midback such as toe-touches, sit-ups, or crunches.
- Change how you get in and out of bed. Rolling to your side to get up can help lessen the progression of hyperkyphosis. It also can help to protect your spinal vertebrae from fracture.
- Modify your environment to help support your posture. They may recommend that you use a back cushion or a supportive chair when sitting. Your physical therapist can recommend changes you can make that are specific to your needs.
- Maintain bone health to prevent thinning bones. Doing weight-bearing exercises and resistance training are important for strong bones. So is getting enough calcium and vitamin D. Some people may need prescribed medicines for bone health. Talk with your doctor and physical therapist to find the best solutions for your needs.
What Kind of Physical Therapist Do I Need?
All physical therapists are prepared through education and experience to treat hyperkyphosis. You may want to consider:
- A physical therapist who has treated people with hyperkyphosis. Some physical therapists have a practice with an orthopedic or geriatric focus.
- A physical therapist who is a board-certified clinical specialist in orthopedic or geriatric physical therapy, or who completed a residency in one of these specialties.
- A physical therapist who has completed a fellowship in spine therapy.
These types of physical therapists have advanced knowledge, experience, and skills that may apply to your condition.
You can search for physical therapists in your area who have these and other credentials by using Find a PT, provided by the American Physical Therapy Association.
General tips when you're looking for a physical therapist (or any other health care provider):
- Get recommendations from family, friends, or other health care providers.
- Ask about the physical therapists' experience in helping people who have hyperkyphosis, have experienced a fall, have a fear of falling, or have balance problems.
- Be prepared to describe your symptoms in as much detail as possible.
The American Physical Therapy Association believes that consumers should have access to information to help them:
- Make informed health care decisions.
- Prepare them for a visit with their health care provider.
The following articles offer some of the best scientific evidence related to physical therapy treatment of hyperkyphosis. They report recent research and give an overview of the standards of practice in the United States and internationally. The articles link either to a Pub Med* abstract or to the free full text, so that you can read it or bring a copy to your health care provider.
Bone Health & Osteoporosis Foundation. Proper Body Alignment. https://www.bonehealthandosteoporosis.org/patients/treatment/exercisesafe-movement/proper-body-alignment/. Accessed February 12, 2023.
Bone Health & Osteoporosis Foundation. Exercise/Safe Movement. https://www.bonehealthandosteoporosis.org/patients/treatment/exercisesafe-movement/. Accessed February 12, 2023.
Hartley GW, Roach KE, Nithman RW, et al. Physical therapist management of patients with suspected or confirmed osteoporosis: a clinical practice guideline from the Academy of Geriatric Physical Therapy. J Geriatr Phys Ther. 2022;44(2):E106–E119. Article Summary in PubMed.
Patel R, Shen J, Nichols JF, et al. Trabecular bone score and its association with Cobb angle kyphosis in older men: a cross-sectional study for the Osteoporotic Fractures in Men (MrOS) Study. Osteoporos Int. 2022;33(5):1171–1176. Article Summary in PubMed.
Ponzano M, Tibert N, Bansal S, et al. (2021). Exercise for improving age-related hyperkyphosis: a systematic review and meta-analysis with GRADE assessment. Arch Osteoporos. 2021;16(1):140. Article Summary in PubMed.
Suwannarat P, Amatachaya P, Sooknuan T, et al. Hyperkyphotic measures using distance from the wall: validity, reliability, and distance from the wall to indicate the risk for thoracic hyperkyphosis and vertebral fracture. Arch Osteoporos. 2018;13(1):25. Article Summary in PubMed.
Aboutorabi A, Arazpour M, Ahmadi Bani M, Keshtkar AA. Effect of spinal orthoses and postural taping on balance, gait and quality of life in older people with thoracic hyperkyphosis: protocol for a systematic review and meta-analysis. BMJ Open. 2018;8(1):e015813. Article Summary in PubMed.
Roghani T, Khalkhali Zavieh M, Rahimi A, et al. The reliability and validity of a designed setup for the assessment of static back extensor force and endurance in older women with and without hyperkyphosis. Physiother Theory Pract. 2018;34(11):882–893. Article Summary in PubMed.
Roghani T, Khalkhali Zavieh M, Rahimi A, et al. The reliability of standing sagittal measurements of spinal curvature and range of motion in older women with and without hyperkyphosis using a skin-surface device. J Manipulative Physiol Ther. 2017;40(9):685–691. Article Summary in PubMed.
Katzman WB, Parimi N, Gladin A, et al. Sex differences in response to targeted kyphosis specific exercise and posture training in community-dwelling older adults: a randomized controlled trial. BMC Musculoskelet Disord. 2017;18(1):509. Article Summary in PubMed.
Senthil P, Sudhakar S, Radhakrishnan R, Jeyakumar S. Efficacy of corrective exercise strategy in subjects with hyperkyphosis. J Back Musculoskelet Rehabil. 2017;30(6):1285–1289. Article Summary in PubMed.
Katzman WB, Vittinghoff E, Lin F, et al. Targeted spine strengthening exercise and posture training program to reduce hyperkyphosis in older adults: results from the study of hyperkyphosis, exercise, and function (SHEAF) randomized controlled trial. Osteoporos Int. 2017;28(10):2831–2841. Article Summary in PubMed.
Kado DM. The rehabilitation of hyperkyphotic posture in the elderly. Eur J Phys Rehabil Med. 2009;45(4):583–593. Article Summary in PubMed.
* PubMed is a free online resource developed by the National Center for Biotechnology Information. PubMed has millions of citations to biomedical literature, including citations in the National Library of Medicine’s MEDLINE database.
Expert Review:
Feb 12, 2023
Revised:
Feb 12, 2023
Content Type: Guide
Hyperkyphosis
PT, MEd, board-certified orthopaedic clinical specialist
Sherri R. Betz
PT, DPT, board-certified clinical specialist in geriatric physical therapy, credentialed exercise expert for aging adults, and nationally certified Pilates teacher
Kenneth L. Miller
PT, DPT, MA, board-certified clinical specialist in geriatric physical therapy, on behalf of APTA Geriatrics, an academy of the American Physical Therapy Association