Physical Therapy Guide to Meralgia Paresthetica (Bernhardt-Roth Syndrome)
Meralgia paresthetica is a condition that causes numbness, tingling, or burning pain in the outer thigh. It is also known as Bernhardt-Roth syndrome. It occurs as a result of nerve compression. The condition most commonly affects people in middle age, and women more than men. However, it can occur at any age. Physical therapists help people safely and effectively manage the symptoms, and some causes, of meralgia paresthetica.
Physical therapists are movement experts. They improve quality of life through hands-on care, patient education, and prescribed movement. You can contact a physical therapist directly for an evaluation. To find a physical therapist in your area, visit Find a PT.
What Is Meralgia Paresthetica (Bernhardt-Roth Syndrome)
Meralgia paresthetica occurs when the lateral femoral cutaneous nerve gets compressed. This nerve is long and stretches from the spine through the groin and into the upper thigh. Abnormal pressure at any point along the nerve can cause symptoms.
This nerve provides feeling to the outside part of the thigh. It does not aid in leg movement. If the nerve becomes compressed and irritated, your outer thigh may have:
- Numbness.
- Tingling.
- Burning pain.
The most common causes of meralgia paresthetica are linked to increased pressure in the groin area. They include:
- Wearing tight garments such as a work belt, a military or police uniform, or tight jeans.
- Obesity or weight gain.
- Pregnancy.
- Recent hip injury.
Other causes can include:
- Direct trauma to the nerve, such as from a seatbelt in a car accident.
- Repeated leg motions (long periods of biking, walking, squatting).
- Muscle spasms.
- Scoliosis.
- Complications from surgery (most common after surgery to the hip or lower back).
- Prolonged stomach lying after surgery or during a hospital stay.
- Diseases such as diabetes, alcoholism, or lead poisoning.
How Does It Feel?
A person with meralgia paresthetica may experience:
- Numbness, tingling, or burning pain on the outside of the thigh.
- Increased tenderness to light touch on the outside of the thigh.
- Pain when lying on the involved side.
- Increased sensitivity to extremes in air or water temperature or different clothing textures.
Pain is often worse with standing or walking and improves with sitting.
How Is It Diagnosed?
Physical therapists and doctors diagnose meralgia paresthetica based your health history and a physical exam. Further tests are rarely needed. Diagnostic imaging tests, such as X-ray or MRI, are not used to diagnose meralgia paresthetica. However, your doctor may use them to rule out other disorders.
Your physical therapist will review your medical history and discuss your symptoms with you. They also will ask about your daily activities, exercise habits, and the clothing or uniforms you wear often. This will help to identify any factors that may contribute to your condition.
Your physical therapist will perform a thorough physical exam of your back, hip, and leg. The goals of the initial exam are to:
- Find the source of your pain.
- Identify any other factors.
- Assess the mobility and strength of your back, hip, and leg.
Your physical therapist may watch you walk, step onto a stair, squat, or balance on one leg. They also will evaluate sensations of touch on the front, side, and back of your hip and leg to find where your symptoms are the worst.
How Can a Physical Therapist Help?
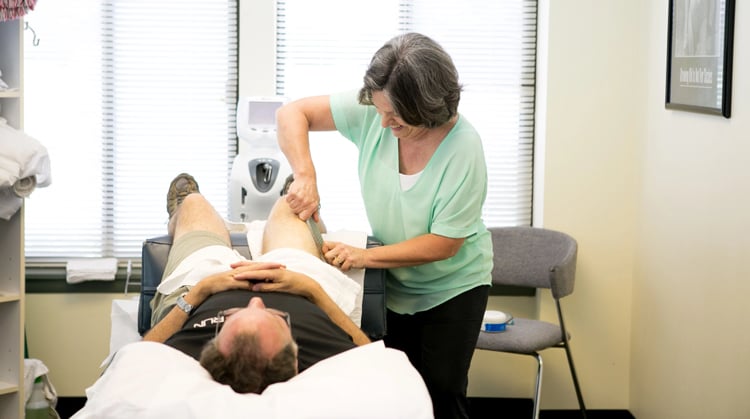
Each case of meralgia paresthetica is different. No matter what the cause, a physical therapist can design a treatment plan to help manage your symptoms. When the condition is caused by a disorder in the hip or pelvis, your physical therapist will address those areas. Their goal is to reduce or eliminate compression on the nerve. Conservative care, such as physical therapy, has been shown to be the most effective treatment for this condition.
Your physical therapist will work with you to develop a plan specific to your needs and goals. They will select treatment strategies in any or all of the following areas:
Pain relief. Physical therapists can provide many pain-relief strategies. These can include:
- Desensitization methods. Your physical therapist may use items of various textures and temperatures to decrease your extreme sensitivity.
- Recommending that you decrease or avoid certain activities or make changes to clothing.
- Applying a special kind of tape to the affected area to help relieve your symptoms.
Range of motion. Your back, hip joint, or surrounding muscles may have limited motion. This can cause increased pressure on the nerve. Your physical therapist may teach you self-stretching techniques. These can decrease muscle tension and help restore normal motion in the back, hip, and leg.
Manual therapy. Your physical therapist may apply hands-on treatments to gently move your muscles and joints. Hands-on (manual) therapy can improve movement and strength. These methods focus on areas that are difficult to treat on your own. Your physical therapist may use neural mobilization (a technique to restore movement in tissues and nerves). This treatment can help to relieve pain caused by the impinged nerve.
Muscle strength. Muscle weaknesses or imbalances linked to injury of the hip or pelvis can cause nerve compression. Your physical therapist will design a safe, progressive strengthening program for your condition. It likely will focus on your core (midsection) and lower extremities (from your hips to toes). You may begin by doing exercises lying down. You will advance to doing exercises in a standing position. Your physical therapist will choose what exercises are right for you, based on your age, symptom level, and physical condition.
Functional training. Symptoms of meralgia paresthetica are often caused or made worse by repeated movements. These motions may be required in your daily or work activities. Based on your movement assessment and goals, your physical therapist will create a series of activities to help you learn how to move your body safely.
Patient education. Your physical therapist will work with you to find and change any external factors that cause you pain. They will recommend improvements and safe alternatives to help you avoid discomfort.
Can This Injury or Condition Be Prevented?
Knowing the causes of meralgia paresthetica, and modifying them when possible, are the best ways to prevent it. In many cases, it may help to:
- Change tight clothing.
- Modify daily work, life, or exercise activities.
- Attain appropriate mobility and strength.
Cases caused by a traumatic injury are harder to prevent.
What Kind of Physical Therapist Do I Need?
All physical therapists are prepared through education and experience to treat meralgia paresthetica. However, you may want to consider:
- A physical therapist who is experienced in treating people with meralgia paresthetica. Some physical therapists have a practice with an orthopedic or muscle, bone, and joint focus.
- A physical therapist who is a board-certified clinical specialist, or who completed a residency or fellowship in orthopedic or sports physical therapy. This physical therapist has advanced knowledge, experience, and skills that may apply to your condition.
You can find physical therapists who have these and other credentials by using Find a PT. This tool built by the American Physical Therapy Association can help you search for physical therapists with specific clinical expertise in your area.
General tips when you're looking for a physical therapist (or any other health care provider):
- Get recommendations from family, friends, or other health care providers.
- When you contact a physical therapy clinic for an appointment, ask about the physical therapists' experience in helping people who have meralgia paresthetica.
- Be prepared to describe your symptoms in detail and explain what makes your symptoms better or worse at your first visit.
The American Physical Therapy Association believes that consumers should have access to information to help them make informed health care decisions and prepare them for their visit with a health care provider.
The following resources offer some of the best scientific evidence related to physical therapy treatment for meralgia paresthetica. They report recent research and give an overview of the standards of practice both in the United States and internationally. They link to a PubMed* abstract, which also may offer free access to the full text, or to other resources. You can read them or print out a copy to bring with you to your health care provider.
Coffey R, Gupta V. Meralgia Paresthetica. Tampa/St Petersburg, FL: StatPearls Publishing; 2021. https://www.ncbi.nlm.nih.gov/books/NBK557735/. Updated February 6, 2021. Accessed May 3, 2021.
Bellinghausen AL, LaBuzetta JN, Chu F, Noelli F, Rodelo AR, Owens RL. Lessons from an ICU recovery clinic: two cases of meralgia paresthetica after prone positioning to treat COVID-19-associated ARDS and modification of unit practices. Crit Care. 2020;24(1):580. Article available in PubMed.
Cheatham SW, Kolber MJ, Salamh PA. Meralgia paresthetica: a review of the literature. Int J Sports Phys Ther. 2013;8(6):883–893. Article Summary in PubMed.
Grossman MG, Ducey SA, Nadler SS, Levy AS. Meralgia paresthetica: diagnosis and treatment. J Am Acad Orthop Surg. 2001;9(5):336–344. Article Summary in PubMed .
* PubMed is a free online resource developed by the National Center for Biotechnology Information. PubMed contains millions of citations to biomedical literature, including citations in the National Library of Medicine’s MEDLINE database.
Expert Review:
Nov 29, 2020
Revised:
Nov 29, 2020
Content Type: Guide
Meralgia Paresthetica
PT, DPT, board-certified clinical specialist in sports physical therapy
Emily Cassata
PT, DPT
James E. Zachazewski
PT, DPT, board-certified clinical specialist in sports physical therapy, on behalf of the American Academy of Sports Physical Therapy