Physical Therapy Guide to Osteochondritis Dissecans
Osteochondritis dissecans, or OCD, is a condition that involves damage within a joint. This condition makes the cartilage unstable and at risk for detaching from the bone. Although the exact cause is unknown, OCD most commonly occurs in children and young athletes ages 10 to 20. Males are more at risk than females. Although OCD is rare, it may be suspected in physically active children and adolescents with joint pain.
The knee, ankle, and elbow are the most common locations of OCD. Surgery is sometimes required, and proper OCD management often takes many health care providers, including a physical therapist. If found early, a physical therapist can treat OCD without surgery. They also help people recover after any needed surgery.
Physical therapists are movement experts. They improve quality of life through hands-on care, patient education, and prescribed movement. You can contact a physical therapist directly for an evaluation. To find a physical therapist in your area, visit Find a PT.
What Is Osteochondritis Dissecans?
Osteochondritis dissecans is a condition that involves damage to the cartilage within a joint. OCD occurs when there is a softening between the cartilage and the bone. Cartilage is the tissue that lines the ends of bones. It provides a smooth surface to protect bones from friction and cushions them during jumping, running, or cutting (a quick change of direction in sports).
With OCD, a lesion (an area of injured tissue) forms where the bone and cartilage meet and makes the cartilage unstable. If a person continues to stress the joint, a piece of cartilage may come off the bone. Sometimes part of the cartilage stays connected. Other times cartilage breaks off entirely and floats within the joint's fluid. This process can lead to a series of symptoms, including:
- Pain.
- Inflammation.
- Decreased function (unable to walk, reach, or move as usual).
- Long-term problems, including locking of the joint and/or early osteoarthritis (cartilage break down).
The knee, ankle, and elbow are the most common locations of OCD.
There are two types of OCD based on a person's age, prognosis (likelihood of needing surgery), and exam:
- Juvenile OCD occurs in children and younger people whose growth plates have not yet closed. A growth plate is an area of active new bone growth in children and teens during development. It is made up of cartilage near the end of long bones. When a growth plate has completely hardened into solid bone, it is considered closed.
- Adult OCD occurs in older adolescents and young adults whose growth plates have closed.
Most OCD lesions are best treated with a health care team. For young athletes, this typically includes the child and family, physical therapist, medical doctors, coaches, and teachers to help the child safely return to activity.
How Does It Feel?
Many people do not know they have anything wrong early on because the most frequent symptom of OCD is an achy joint after activity. As it progresses, a person may limp if the knees or ankles are affected. The joint can be painful or tender at a certain point in the joint's range of motion or with a specific activity.
Common signs and symptoms that develop with OCD include:
- Swelling or stiffness of the affected area that may worsen following activity.
- Limited range of motion or locking of the joint.
- Pain when moving the joint.
- Tenderness along the joint.
- A feeling of popping, cracking, or grinding when moving the joint.
- Pain that gets worse during or after activity, especially when walking, running, jumping, or changing direction. Children may complain of pain during or after recess or gym activities.
Symptoms of OCD typically develop gradually as the damage to the cartilage and bone gets worse. Sometimes, people do not know they have an OCD lesion. This is usually because:
- They cannot remember a specific injury.
- Their early symptoms do not limit their activity.
Often OCD goes unnoticed in children because they may not know something is wrong or can't describe their symptoms. If left untreated, OCD can progress and a person may need surgery to secure the OCD lesion and promote bone and cartilage growth. You may need surgery if:
- The condition does not improve with nonsurgical treatment.
- A piece of cartilage has broken off and is floating or trapped within the joint.
- Growth plates have closed, and improvement without surgery is doubtful.
How Is It Diagnosed?
Physical therapists are an important part of your health care team. Your physical therapist will conduct an evaluation to determine the factors that may be contributing to your condition.
They will interview you to gather information about your health history, condition, and activities. They may be helped by forms you fill out before your first session. The interview will become more specific to the symptoms of OCD. Your physical therapist may ask you questions like:
- When did you first notice this starting?
- What are your current symptoms?
- Do you have pain, and if so, where and how bad does it hurt?
- Does your pain change throughout the day?
- What has helped decrease the pain?
- Do you have trouble doing anything?
- Have you seen any other health care providers for this condition?
- Have you had imaging (X-ray, MRI) or other tests?
This information helps the physical therapist to understand better what you are experiencing. It also helps to determine the best treatment plan.
The physical exam will vary depending on your interview. Most often, it will begin with observing the area of your symptoms and any movements or positions that cause pain. The physical exam may include:
- Identifying any areas that may be tender or painful.
- Asking you to show them any movements that cause the pain to increase or decrease.
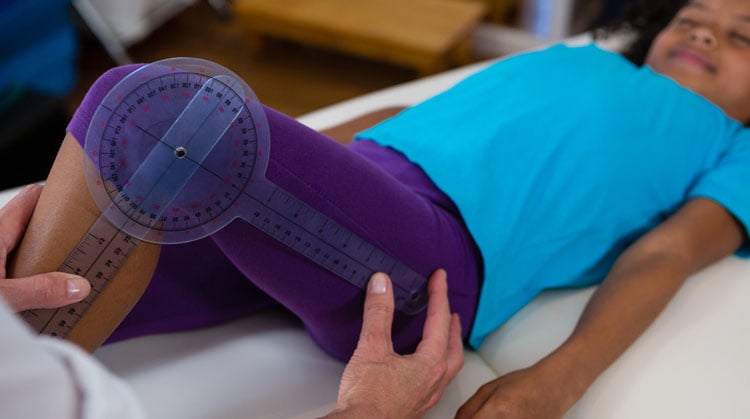
- Measuring the affected joint's movement.
- Assessing your strength and flexibility.
If the patient is a young child, they may need a parent's or guardian's help to detail their complaints and any changes due to symptoms. Information from teachers and coaches can describe how the child responds to physical activities at school.
Several imaging tests help to diagnose and determine how severe OCD is, including:
- X-rays of your joint in different positions.
- An MRI or CT scan if severe joint damage is suspected.
Your medical team will grade your bone and cartilage status on a scale and determine the level of damage based on X-Ray, CT, or MRI findings. This grade will help your physical therapist and medical team as they work together to develop a treatment program specific to your condition and needs.
If you have joint pain that does not respond to rest or that worsens, seek the advice of a physical therapist or other health care provider!
How Can a Physical Therapist Help?
Your physical therapist will design a treatment program specific to your condition and goals. Your treatment plan may include:
Activity guidance. If untreated, OCD may get worse over time. Working as part of your medical team, your physical therapist will help prescribe activities and exercises. Your physical therapist will design an exercise program to help and not harm your joint. The goal of the program is to restore function and health. Imaging done at certain times may help to ensure your cartilage and bone can handle specific loads.
Limiting weight-bearing activities. Your physical therapist may recommend decreasing the weight you put on your leg if you have an OCD lesion in your ankle or knee. This may include using a bike or swimming instead of running. They may ask you to use crutches or a wheelchair instead of walking.
Range-of-motion exercises. One of the most common symptoms of OCD is the limited motion of the injured joint. Your physical therapist will assess for any movement limitations. They will compare the affected joint's movement to the other side of your body and expected normal ranges. Based on your results, your physical therapist may guide you through exercises to restore normal motion.
Muscle strengthening. Strengthening the muscles around the injured joint is an essential part of restoring function. With OCD, decreases in muscle performance may not be evident at first. Muscle function may worsen as damage to the cartilage and bone progresses. For example, muscles along the front and back of the thigh (quadriceps and hamstrings) cross the knee joint and help control the motion of and forces to the knee bones.
Strengthening the hip and core muscles also can help balance the amount of force on leg joints. This is especially important during walking or running. Your physical therapist will:
- Assess these muscle groups.
- Compare the strength in each leg.
- Prescribe specific exercises to target any areas of weakness.
Manual therapy. Your physical therapist may use hands-on therapy to gently move and stretch muscles and joints. Manual therapy helps to improve motion, flexibility, and strength. These techniques can target areas that are difficult to treat on your own. Manual therapy may help to restore the joint's normal motion in people with OCD injuries.
Modalities. Your physical therapist may recommend treatments like ice and heat to aid in pain management.
Bracing. Compression sleeves around the affected joint may help reduce pain and swelling. If surgery is needed, your physical therapist may recommend using braces to control the amount of motion allowed after surgery.
Surgery Considerations
People with the following may need surgery:
- Closed growth plates.
- Loose bodies (pieces of cartilage that broke off).
- Unstable fragments.
- Lack of improvement with nonsurgical treatment.
- Other related injuries.
The goal of surgery is to restore the damaged cartilage and bone. Your surgeon will consider the following to determine which kind of surgery is right for you:
- The condition or level of damage to your joint.
- Your age.
- The activity level you want.
Your physical therapist will refer you to a surgeon if needed. They also will work with you after surgery to help you safely recover.
Can This Injury or Condition Be Prevented?
There are many theories about what causes OCD. The exact reason for it remains unknown. Factors that may influence the development of OCD include:
- The size and shape of your bones.
- Family genetics.
- The stage of development in children.
Seeing a physical therapist may decrease a young person's risk for developing OCD. A physical therapist can help people:
- Avoid too much high-intensity exercise.
- Develop stretching and strengthening activities specific to a young athlete's needs.
- Select the proper shoes and equipment to promote good form for athletic activities.
- Understand the:
- Risks of pushing through pain caused by athletics.
- Importance of getting enough rest and recovery between athletic events.
- Common signs and symptoms of joint injury.
What Kind of Physical Therapist Do I Need?
All physical therapists are prepared through education and experience to treat a variety of conditions or injuries. You may want to consider:
- A physical therapist with experience treating people who have orthopedic (muscle, bone, and joint) injuries.
- A physical therapist who is a board-certified specialist or has completed a residency in orthopedic or sports physical therapy. This physical therapist will have advanced knowledge, experience, and skills that apply to athletes.
You can find physical therapists who have these and other credentials by using Find a PT, the online tool built by the American Physical Therapy Association. This tool can help you search for physical therapists with specific clinical expertise in your area.
General tips when you are looking for a physical therapist (or any other health care provider):
- Call ahead to see if the physical therapist has experience treating OCD lesions.
- Get recommendations from family, friends, or other health care providers.
- When you contact a physical therapy clinic for an appointment, ask about the physical therapists' experience in helping young athletes.
- Be prepared to describe your symptoms in as much detail as possible, and report activities that make your symptoms worse.
The American Physical Therapy Association believes that consumers should have access to information to help them make health care decisions and prepare them for their visit with their health care provider.
The following resources offer some of the best scientific evidence related to physical therapy treatment for osteochondritis dissecans. They report recent research and give an overview of the standards of practice both in the United States and internationally. They link to a PubMed* abstract, which also may offer free access to the full text, or to other resources. You can read them or print out a copy to bring with you to your health care provider.
Accadbled F, Vial J, Sales de Gauzy J. Osteochondritis dissecans of the knee. Orthop Traumatol Surg Res. 2018;104(1S):S97–S105. Article Summary in PubMed.
Bauer KL, Polousky JD. Management of osteochondritis dissecans lesions of the knee, elbow, and ankle. Clin Sports Med. 2017;36(3):469–487. Article Summary in PubMed.
Eismann EA, Pettit RJ, Wall EJ, Myer GD. Management strategies for osteochondritis dissecans of the knee in the skeletally immature athlete. J Orthop Sports Phys Ther. 2014;44(9):655–679. Article Summary in PubMed.
* PubMed is a free online resource developed by the National Center for Biotechnology Information. PubMed contains millions of citations to biomedical literature, including citations in the National Library of Medicine's MEDLINE database.
Expert Review:
Mar 20, 2021
Revised:
Mar 20, 2021
Content Type: Guide
Osteochondritis Dissecans
Kathryn Lucas
PT, DPT, PhD, board-certified clinical specialist in sports and orthopaedic physical therapy
James E. Zachazewski
PT, DPT, board-certified clinical specialist in sports physical therapy, on behalf of the American Academy of Sports Physical Therapy