Physical Therapy Guide to Thoracic Outlet Syndrome
Thoracic outlet syndrome can be a painful and disabling condition of the upper extremity. It results from compression of structures in the space above the first rib and between the collar bone (clavicle). Due to varying signs and symptoms of TOS, the number of people with the condition is unknown. Physical therapists help people who have TOS to ease their symptoms and restore their upper body function.
Physical therapists are movement experts who design treatment plans for each person’s needs and goals. They improve quality of life through hands-on care, patient education, and prescribed movement. You can contact a physical therapist directly for an evaluation. To find a physical therapist in your area, visit Find a PT.
What Is Thoracic Outlet Syndrome?
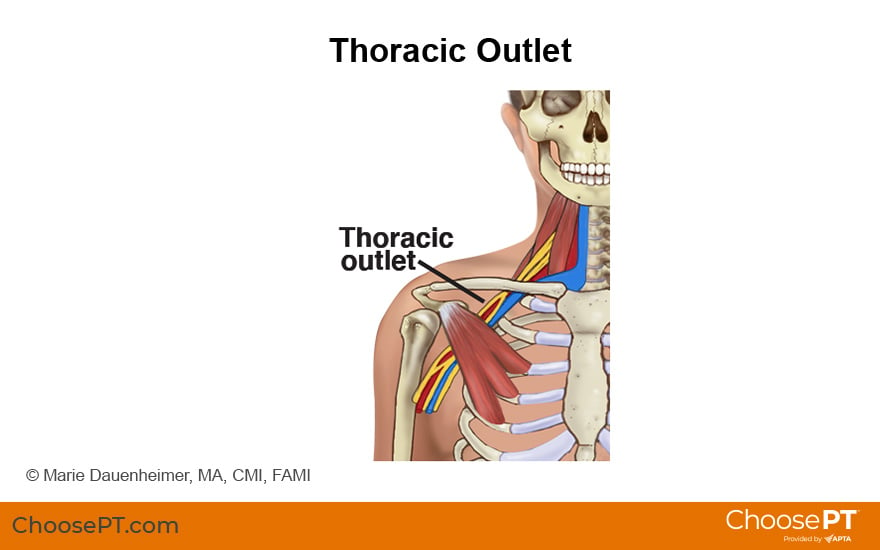
Thoracic outlet syndrome involves the compression or irritation of the nerves and/or blood vessels between the first rib and the collar bone. TOS can result from:
- An acute injury.
- Disease.
- Chronic abnormal posture.
- Repetitive injury.
- A problem present at birth (such as an abnormal first rib).
How Does It Feel?
Symptoms of TOS may vary, depending on the type of structures compressed. More than 90% of TOS cases are likely due to nerve compression (neurogenic). The four categories of TOS are:
Category 1: Arterial TOS
- Pain in the hand, rarely in shoulder or neck.
- Coldness or cold intolerance.
- Numbness and tingling.
- Symptoms worsen when the involved arm and hand is over the head.
Category 2: Venous TOS
- Pain in the arm.
- Swelling in the arm.
- Change in arm color (appears bluish).
- Feeling of heaviness in the arm.
- Numbness and tingling in fingers and hands.
- Symptoms worsen when the involved arm and hand is over the head.
Category 3: True Neurogenic TOS
- Pain, numbness, and tingling in the hand, arm, shoulder, and often the neck.
- Headaches.
- Numbness and tingling of the arm, often waking a person during the night.
- Hand clumsiness.
- Intolerance to cold.
- Hand coldness and color changes.
- Symptoms worsen when the involved arm and hand is over the head.
Category 4: Disputed Neurogenic TOS
- Pain, numbness and tingling in the hand, arm, shoulder, and often the neck.
- Headaches.
- Numbness and tingling of the arm, often waking a person during the night.
- Hand clumsiness.
- Intolerance to cold.
- Hand coldness and color changes.
- Symptoms greater at night.
- Tests may come back normal (hence, the term "disputed").
How Is It Diagnosed?
Diagnosis of TOS begins with a thorough health history and exam. Your physical therapist also will check for any color changes in the affected area. They may try to provoke symptoms by gently moving the affected limb in different directions.
You also may be referred for diagnostic testing such as:
- Doppler ultrasound, which can confirm arterial and venous TOS.
- Nerve conduction velocity testing to help confirm a neurogenic TOS.
Your physical therapist may be the first to recognize the onset of TOS. This is because of how it effects your physical function. During their exam, your physical therapist may ask you questions such as:
- When did you begin experiencing symptoms, and when are they the worst?
- Have you noticed any change in your symptoms when the temperature changes?
- Have you noticed any significant changes in your ability to do physical tasks that require hand movements?
- Have you noticed any changes in the appearance of your arm or hand?
- Are there certain positions that bring on your symptoms?
In addition, your physical therapist will rule out other conditions, which may mimic TOS.
How Can a Physical Therapist Help?
Based on their findings, your physical therapist will develop a customized rehabilitation program to help ensure a safe return to your desired activities. Some general treatment techniques may include:
- Patient education. Your physical therapist will educate you about thoracic outlet syndrome to help you make decisions. Your physical therapist will work with you to identify and suggest changes to any factors causing your pain. These can include changes to the type and amount of exercise, athletic activities, and activities of daily living. They will recommend ways to improve your activities and develop a personalized exercise program.
- Pain management. Your physical therapist will design a program to address your pain that includes applying ice to the affected area. They also may recommend modifying some activities that cause pain. Physical therapists are experts in pain-management techniques that reduce or eliminate the need for pain medicines, including opioids.
- Range-of-motion exercise. The mobility of your neck, shoulder, and arm may be limited, causing increased stress to the area. Your physical therapist may teach you self-stretching techniques to decrease tension and help restore normal motion of the affected joints.
- Manual therapy. Your physical therapist may treat your condition by applying “hands on” treatments to gently move your muscles and joints. These techniques help improve motion. They also may use hands-on therapy to guide your neck, shoulder, and arm into a less stressful movement pattern. Your physical therapist can provide the right amount of manual resistance to improve any strength deficits.
- Muscle strengthening exercises. Muscle weaknesses or imbalances can contribute to TOS and ongoing symptoms. Based on your symptoms, your physical therapist will design a safe, progressive resistance program for you. You may begin by doing exercises lying on a table or at home on the bed or floor. You then may advance to exercises in a standing position. Your physical therapist will choose what exercises are right for you based on your age and physical condition.
- Functional training. Once your pain, strength, and motion improve, you will need to safely transition back into more demanding activities. To minimize the stress to the neck, shoulder, and arm, it is important learn safe, controlled movements. Based on their assessment and your goals, your physical therapist will give you a series of activities to help you learn how to use and move your body correctly and safely.
- Assistive devices. Your physical therapist may recommend that you use a posture garment to help limit the strain on the area. This will be determined during your treatment sessions.
Can This Injury or Condition Be Prevented?
Some cases of TOS cannot be prevented, including cases due to:
- Body variations.
- Conditions present at birth.
- Trauma.
- Lesions that take up space in the thoracic compartment.
Other cases may be avoidable. Knowing the risk factors that could make you more likely to develop TOS is the first step to prevention.
Your physical therapist will help you develop strategies to help manage your risk factors and symptoms. As with many conditions, education is key. Understanding ways to reduce your symptoms while doing activities can help you live a full and functional life.
What Kind of Physical Therapist Do I Need?
All physical therapists are prepared through education and clinical experience to treat a variety of conditions or injuries. You may want to consider:
- A physical therapist who is experienced in treating people with TOS.
- A physical therapist who is a board-certified clinical specialist or who completed a residency or fellowship in orthopedic physical therapy. This therapist has advanced knowledge, experience, and skills that may apply to your condition.
You can find physical therapists who have these and other credentials by using Find a PT, the online tool built by the American Physical Therapy Association to help you search for physical therapists with specific clinical expertise in your geographic area.
General tips when you're looking for a physical therapist (or any other health care provider):
- Get recommendations from family, friends, or other health care providers.
- When you contact a physical therapy clinic for an appointment, ask about the physical therapists' experience in helping people with TOS.
- Be prepared to describe your symptoms in as much detail as possible. Keep a journal to note when you experience pain to share with your physical therapist to enable them to quickly identify the best treatment approach.
The American Physical Therapy Association believes that consumers should have access to information that could help them make health care decisions and prepare them for a visit with their health care provider.
The following articles provide some of the best scientific evidence related to physical therapy treatment of TOS. The articles report recent research and give an overview of the standards of practice both in the United States and internationally. The article titles are linked either to a PubMed* abstract of the article or to free full text, so that you can read it or print out a copy to bring with you to your health care provider.
Warrick A, Davis B. Neurogenic thoracic outlet syndrome in athletes — nonsurgical treatment options. Curr Sports Med Rep. 2021:20(6):319–326. Article Summary in PubMed.
Balderman J, Abuirqeba AA, Eichaker L, et al. Physical therapy management, surgical treatment, and patient-reported outcomes measures in a prospective observational cohort of patients with neurogenic thoracic outlet syndrome. J Vasc Surg. 2019 Sep;70(3):832–841. Article Summary in PubMed.
*PubMed is a free online resource developed by the National Center for Biotechnology Information. PubMed contains millions of citations to biomedical literature, including citations in the National Library of Medicine's MEDLINE database.
Expert Review:
Mar 4, 2022
Revised:
Jun 9, 2022
Content Type: Guide
Thoracic Outlet Syndrome
PT, DPT, fellow of the American Academy of Orthopedic Manual Physical Therapists
Susan Reischl
PT, DPT, board-certified clinical specialist in orthopaedic physical therapy
Stephen F. Reischl
PT, DPT, board-certified clinical specialist in orthopaedic physical therapy, on behalf of the Academy of Orthopaedic Physical Therapy