Physical Therapy Guide to Total Knee Replacement (Arthroplasty)
A total knee replacement, or arthroplasty, involves replacing damaged parts of the bones at the knee joint. The knee is the most replaced joint in the body. It is best to consult both your surgeon and physical therapist when deciding whether to have a total knee replacement. Your decision should be based on how much your pain or loss of function is affecting your quality of life. Usually, people have total knee replacement surgery after trying conservative treatment options for:
- Knee joint damage due to osteoarthritis, rheumatoid arthritis, other bone diseases, or fracture. Knee replacement removes arthritis, and it will not return in the replaced joint.
- Knee pain or alignment problems in the leg that cause difficulty with walking or doing daily activities.
Physical therapists help people prepare for and restore function after knee replacement surgery.
Physical therapists are movement experts. They improve quality of life through hands-on care, patient education, and prescribed movement. You can contact a physical therapist directly for an evaluation. To locate a physical therapist in your area, visit Find a PT.
What Is Total Knee Replacement (TKR)?
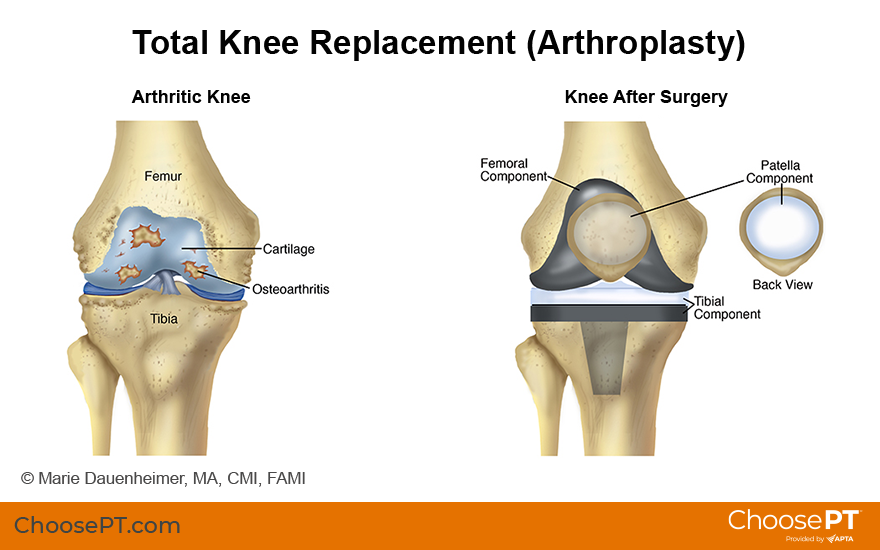
A total knee replacement involves removing and replacing the damaged parts of the bones in the knee joint. These bones include the:
- Tibia, sometimes called the shin bone.
- Femur, or thigh bone.
- Patella, or kneecap.
Replacement parts consist of:
- A metal cap at the end of the femur.
- A tray and stem of metal inserted into the tibia and topped with a plastic liner. This allows the surfaces to move smoothly.
- A smooth plastic surface to line the back of the kneecap.
Partial knee replacement is surgery to address arthritis on only one side or one area of the knee joint. When the arthritis is only on the back of the kneecap, it is a “patellofemoral” replacement.
How Can a Physical Therapist Help?
If you have knee replacement surgery, your physical therapist will be a vital part of your health care team. Physical therapists can help you prepare in advance of surgery and will help you recover from it. They will work with you to help you regain your movement and function so you can return to your daily activities. Your physical therapist will develop a personalized treatment program. They will work with you to get you safely moving again in the most effective way possible.
Before Surgery
A recent study showed that completing a six-week exercise program before knee replacement led to much better pain and function scores (right after and six months after surgery) compared with not doing so.
“Prehab” is physical preparation and structured education before surgery to minimize physical decline. As movement experts, physical therapists are uniquely qualified to:
- Assess any physical deficits prior to surgery.
- Identify potential physical effects related to surgery.
- Provide prevention strategies.
Before surgery, your physical therapist may:
- Teach you exercises to improve the strength and flexibility of the:
- Knee joint.
- Upper body.
- Surrounding muscles.
- Prepare you to use a walker or other assistive device.
- Recommend changes you should make at home before you have surgery. These may include:
- Making sure spaces around your home are clear and hazard-free to prevent tripping and falling.
- Placing a chair to allow you to sit rather than squat to get something out of a low cabinet.
Good physical health before surgery improves your chances for better results (especially short-term). It also reduces your risk for complications. Long before surgery, it is helpful to:
- Lose excess body weight. This can help you recover more quickly and help improve your function and overall results after surgery.
- Stop smoking. Being tobacco-free will improve the healing process after surgery. Seek help or advice from your physician on stopping smoking, as you schedule and plan for your surgery.
After Surgery
Many people go home on the same day as total knee replacement surgery, depending on their condition and other factors. People with chronic conditions or physical disabilities may stay overnight following surgery. Or they may need to discharge to a skilled nursing facility before going home.
Shortly after your surgery, a physical therapist may:
- Work with you to show you how to move safely so you can function at home.
- Show you how to safely get in and out of a bed and chairs.
- Show you how to use a walker or crutches and get in and out of a car.
- Educate you on applying ice, elevating your leg, and using compression wraps or stockings. These activities will control swelling in the knee area and help your incision heal.
- Teach you breathing exercises to help you relax.
- Help you continue the exercises that you may have learned before your surgery.
As You Begin to Recover
In the first two weeks of recovery, you will mostly focus on:
- Bending your knee.
- Stretching your knee straight.
- Managing pain and making it bearable during your recovery.
- Decreasing swelling.
- Restoring normal walking.
- Doing exercises to help you move through the different stages of recovery.
After two weeks, your physical therapist will tailor your exercise program to address your specific needs. Your program may include:
- Higher degree range-of-motion exercises.
- Progressive muscle-strengthening exercises.
- Body awareness and balance training.
- Functional training.
- Activity-specific training. This training addresses your specific goals.
Your specific treatment plan may include:
Range-of-motion exercises. Active knee bending and straightening helps to improve pain and swelling. Your physical therapist will safely guide you through exercises to restore your knee range of motion. Movement flexibility is key to beginning a strengthening program.
Strengthening exercises. Your physical therapist will guide you through the right exercises to ensure a healthy recovery. This will help you build the muscle strength needed to walk and then use stairs. If your thigh and lower leg muscles are too weak, you may first need a walker, then graduate to using a cane, until you gain enough strength to walk and use the stairs on your own.
Balance training. Specialized training exercises help your muscles "learn" to respond to changes around you, such as a sidewalk becoming uneven or finding yourself on rocky ground. Working to support full weight on your leg will improve your balance and decrease chances of falling. Balance training will prepare you for real-life situations. Your physical therapist may have you do activities that challenge your balance and knee control to help you improve. They will design your program based on your specific needs, goals, activity level, and general health.
Functional training. When you can walk without pain, your physical therapist may add activities. They will help you get back to doing what you used to do before knee pain limited you. Your training might include crossing a busy street or getting on and off an escalator. The specific activities will be based on your needs and goals.
Activity-specific training. The timeline for returning to work, daily, leisure, or sports activities varies from person to person. Your physical therapist can estimate your unique timeline based on your specific condition. Depending on your job or sport, you may need additional visits tailored to your specific activities (such as climbing a ladder or swinging a golf club). Your physical therapist can personalize an exercise program that takes all these demands into account.
Can This Injury or Condition Be Prevented?
If you have knee pain, you may be able to delay the need for surgery by working with a physical therapist. They can help you improve the flexibility and strength of the muscles that support and move your knee. In some cases, this type of training may even help you avoid surgery altogether.
Following an exercise program designed by a physical therapist can protect against knee injury.
Doing regular moderate-intensity physical activities and controlling your weight through diet may reduce the risk of knee osteoarthritis getting worse.
What Kind of Physical Therapist Do I Need?
All physical therapists are prepared through education and experience to provide treatment before or after total knee replacement surgery. You may want to consider:
- A physical therapist with experience treating people with orthopedic or muscle, bone, and joint problems.
- A physical therapist who is a board-certified clinical specialist or who completed a residency or fellowship in orthopedic or geriatric physical therapy. This physical therapist has advanced knowledge, experience, and skills that may apply to your condition.
You can find physical therapists who have these and other credentials by using Find a PT, a tool built by the American Physical Therapy Association to help you search for physical therapists in your area.
General tips before making an appointment with a physical therapist (or any other health care provider):
- Get recommendations from family, friends, or other health care providers.
- Ask about the physical therapists' experience in helping people with knee replacements.
- Be prepared to describe your symptoms in as much detail as possible and your goals at the end of treatment.
The American Physical Therapy Association provides this information to help consumers make informed health care decisions and prepare them for their visit with their health care provider.
The following articles offer some of the best scientific evidence related to physical therapy treatment before and after total knee replacement. The articles report recent research and give an overview of the standards of practice both in the United States and internationally. The titles link either to a PubMed* abstract (summary) of the article or to free full text. You can read it or print a copy to bring with you to your health care provider.
Gränicher P, Mulder L, Lenssen T, et al. Prehabilitation improves knee functioning before and within the first year after total knee arthroplasty: a systematic review with meta-analysis. J Orthop Sports Phys Ther. 2022;52(11):709–725. Article Summary in PubMed.
Wang D, Wu T, Li Y, et al. A systematic review and meta-analysis of the effect of preoperative exercise intervention on rehabilitation after total knee arthroplasty. Ann Palliat Med. 2021;10(10):10986–10996. Article Summary in PubMed.
Jette DU, Hunter SJ, Burkett L, et al. Physical therapist management of total knee arthroplasty. Phys Ther. 2020;100(9):1603–1631. Article Summary in PubMed.
Domínguez-Navarro F, Igual-Camacho C, Silvestre-Muñoz A, et al. Effects of balance and proprioceptive training on total hip and knee replacement rehabilitation: a systematic review and meta-analysis. Gait Posture. 2018;62:68–74. Article Summary in PubMed.
Doma K, Grant A, Morris J. The effects of balance training on balance performance and functional outcome measures following total knee arthroplasty: a systematic review and meta-analysis. Sports Med. 2018;48(10):2367–2385. Article Summary in PubMed.
Pua YH, Seah FJ, Poon CL, et al. Age- and sex-based recovery curves to track functional outcomes in older adults with total knee arthroplasty. Age Ageing. 2018;47(1):144–48. Article Summary in PubMed.
Sobh AH, Siljander MP, Mells AJ, et al. Cost analysis, complications, and discharge disposition associated with simultaneous vs staged bilateral total knee arthroplasty. J Arthroplasty. 2018;33(2):320–323. Article Summary in PubMed.
Bistolfi A, Zanovello J, Ferracini R, et al. Evaluation of the effectiveness of neuromuscular electrical stimulation after total knee arthroplasty: a meta-analysis. Am J Phys Med Rehabil. 2018;97(2):123–130. Article Summary in PubMed.
Harmelink KE, Zeegers AV, Hullegie W, et al. Are there prognostic factors for one-year outcome after total knee arthroplasty: a systematic review. J Arthroplasty. 2017;32(12):3840–3853.e1. Article Summary in PubMed.
Otero-López A, Beaton-Comulada D. Clinical considerations for the use lower extremity arthroplasty in the elderly. Phys Med Rehabil Clin N Am. 2017;28(4):795–810. Article Summary in PubMed.
Loyd BJ, Jennings JM, Judd DL, et al. Influence of hip abductor strength on functional outcomes before and after total knee arthroplasty: post hoc analysis of a randomized controlled trial. Phys Ther. 2017;97(9):896–903. Article Summary in PubMed.
* PubMed is a free online resource developed by the National Center for Biotechnology Information. PubMed has millions of citations to biomedical literature, including citations in the National Library of Medicine’s MEDLINE database.
Expert Review:
Feb 22, 2022
Revised:
May 8, 2023
Content Type: Guide
Knee Replacement
PT, DPT, PhD, board-certified clinical specialist in orthopaedic physical therapy
Alisa Curry
PT, DPT, board-certified clinical specialist in geriatric physical therapy
Kenneth L. Miller
PT, DPT, MA, board-certified clinical specialist in geriatric physical therapy, on behalf of APTA Geriatrics, an academy of the American Physical Therapy Association
You Might Also Like...
Patient Stories
'Famous Amos' Founder Relies On His Physical TherapistJul 29, 2021
Amos is convinced that his success is a result of the individual attention he received from a physical therapist who understood his body and cared about
Did You Know?
Prescribed Opioids Resulted in 3.3 Billion Unused PillsNov 1, 2017
Despite increased efforts and awareness to reduce opioid use after surgery, nine out of 10 patients were prescribed an average of 85 pills after surgery
Podcast
Volleyball Legend Gabrielle Reece Chooses PT, Not Opioids, After Knee SurgeryDec 19, 2016
Former professional beach volleyball player Gabby Reece shares how she managed pain after knee replacement surgery and relied on physical therapy to return


