Physical Therapy Guide to Bunion (Hallux Valgus)
A bunion (hallux valgus) is a bony bump on the side of the foot that develops at the base of the big toe. This area of the foot can become inflamed and swollen, causing foot pain. Bunions most often develop in women and older adults. Over time, the affected joint may become stiff, painful, and deformed. Bunions and the pain they cause can lead to problems with shoe fit and difficulty walking. Physical therapists help people with bunions reduce their pain, increase the function of the big toe, improve muscle strength, and restore walking ability.
Physical therapists are movement experts. They improve quality of life through hands-on care, patient education, and prescribed movement. You can contact a physical therapist directly for an evaluation. To find a physical therapist in your area, visit Find a PT.
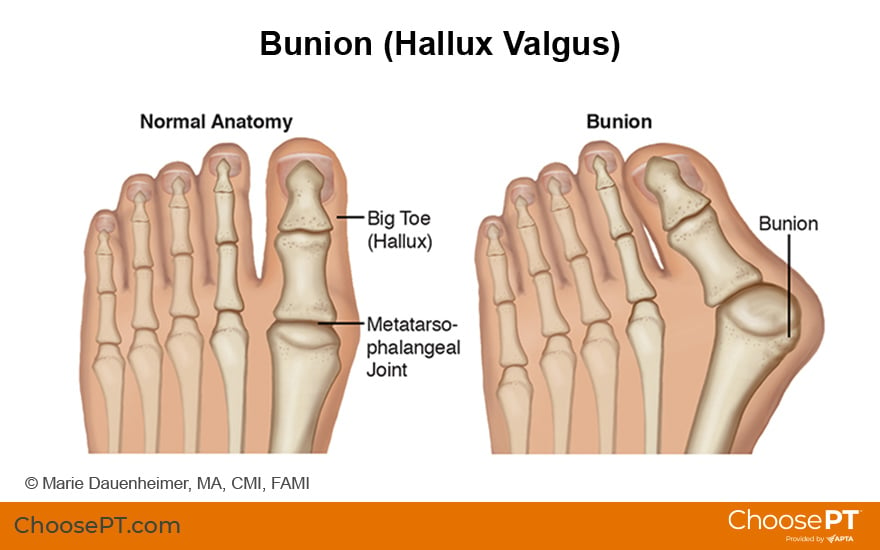
What Is a Bunion?
A bunion is a bump on the side of the foot that develops at the joint where the big toe connects to the foot. It can be classified as mild, moderate, large, or severe. Several factors may cause bunions, including:
- Heredity.
- Foot shape.
- Flat arches.
- Loose joints (known as laxity).
- Osteoarthritis.
Recent research suggests that footwear may not be a factor in bunion development. However, tight footwear can irritate a bunion by rubbing on the tissue at the joint. This pressure creates more swelling and pain.
How Does It Feel?
How a bunion feels varies with each individual. Not all bunions cause symptoms. People with bunions report mild to severe symptoms, including:
- Pain and swelling in the big toe joint that gets worse with standing and walking.
- Gradual enlargement of the bump on the side of the foot. The bunion can become inflamed and swollen, causing foot pain.
- Pain when wearing shoes, making it difficult to find comfortable or stylish footwear.
- Changes in gait (walking movements).
- Increased difficulty walking.
- Changes in balance, increasing the risk of falling, particularly in older adults.
- Crossing of the big toe and lesser toes, causing crowding of the toes. This symptom can also result in other deformities and pain.
- Reduced quality of life because of foot pain.
How Is It Diagnosed?
A physical therapist will conduct a thorough examination on your first visit. This will include taking your health history. The goals of the initial exam are to determine the degree of your injury and its probable cause. The interview will be specific to you. It may include questions like:
- What is the history of your foot condition?
- How have you taken care of your bunion so far? Have other health care practitioners ordered imaging or other tests?
- What are your current symptoms and how do they affect your day?
- If there is pain what is the location and intensity of your pain? Does your pain vary during the day?
- What activities, if any, do you find hard to complete?
- What activities are you unable to complete?
- Are there any activities that reduce your level of symptoms?
After the interview, your physical therapist will conduct a physical examination. They may:
- Observe your movement doing activities discussed in the interview.
- Assess the movement and strength of the ankle, foot, and toes. The exam also may include other areas of the body, such as the leg or hip, which may be contributing to your condition.
- Gently touch your ankle, foot, and toes to determine the precise location of your pain.
To ensure a correct diagnosis, your physical therapist may also refer you to a specialist for an X-ray or other images of the area.
Once the diagnosis is made, your physical therapist will work with you to develop a treatment program to help reduce your pain, keep your bunion from getting worse, and restore movement.
How Can a Physical Therapist Help?
Physical therapists are movement experts who provide treatments to improve quality of life. Treatment programs for bunions can include exercise, hands-on care, and patient education. Your physical therapist will design a program to treat your specific symptoms. The purpose of treatment is to improve the function of the ankle, foot, and toes, reduce your pain, and get you moving again. Your treatment plan may include:
Patient education. Your physical therapist will work with you to identify and change any external factors causing your pain. The type and amount of exercises you perform, your athletic activities, and your footwear may be discussed. Your physical therapist will recommend improvements in your daily activities and design a personalized exercise program to help ensure a pain-free return to your desired activity level.
Pain management. Your physical therapist will design a program to address your pain that may include applying ice to the affected area. They also may recommend modifying some activities that cause pain. Physical therapists are experts in prescribing pain-management techniques that reduce or eliminate the need for medication, including opioids.
Range-of-motion exercise. The bunion and big toe may not be moving correctly, causing increased stress. Your physical therapist may teach you self-stretching techniques to help restore normal motion of the foot, ankle, and toes.
Manual therapy. Your physical therapist may provide “hands-on” treatments to gently move your muscles and joints. These techniques help improve motion and strength. They often address areas that are difficult to treat on your own.
Muscle strengthening. Your physical therapist will prescribe exercises to strengthen the muscles of the big toe and ankle. Muscle weaknesses or imbalances in other parts of the body also can contribute to bunions and pain. Your physical therapist will choose what strengthening exercises are right for you based on your age, specific physical condition, and goals.
Functional training. Once your pain, strength, and motion improve, you can begin to return to more demanding activities. To minimize stress on your bunion and great toe, you will need to learn safe, controlled movements. Your physical therapist will create a series of activities to help you learn how to use and move your body correctly and safely.
Orthotics and devices. Your physical therapist may recommend the use of splints, shoe inserts, or assistive devices, depending on your condition, and will train you in their use. They may include:
- Splints and toe separators to reduce pain and pressure on the big toe.
- Custom or over-the-counter arch supports (foot orthotics) to help keep the foot and ankle in a correct position when walking.
- A cane, walker, or crutches (assistive devices) to help reduce pain and improve your ability to walk.
How Can a Physical Therapist Help Before and After Surgery?
If your bunion deformity progresses to a point where you cannot find comfortable footwear or walking becomes very difficult, you may choose surgery to correct the position of the big toe. Following surgery, a physical therapist can help you restore the strength and movement of your big toe, reduce pain, and allow you to return to the highest level of function possible.
Immediately after surgery, a hospital physical therapist will teach you how to walk with a cane, walker, or crutches to avoid putting weight on the surgical area. They will also instruct you in the use of ice packs and leg elevation to control pain and swelling.
Recovery and treatment vary with each person, based on their condition and the type of surgical procedure performed. After most surgeries, you will wear a special shoe to protect your foot. This shoe will help you avoid putting pressure on the surgical area.
After discharge from the hospital, you can begin working with a physical therapist to regain your strength and mobility. Treatments will include the elements listed above. The first session may focus on the use of mild ankle range-of-motion exercises, ice packs, and mild massage. Your physical therapist will design a treatment program specifically for you. They will instruct you on how to safely walk and perform exercises in the clinic and at home.
Can This Injury or Condition Be Prevented?
There is no evidence that bunions can be prevented. However, you may be able to prevent a problem from becoming worse, and possibly avoid surgery, by following these guidelines:
- Wear appropriate footwear. For example, avoid wearing shoes that squeeze the toes together. Wearing shoes with a wider toe box will reduce the inward pressure on the big toe, and help keep the outside of the foot from rubbing against the shoe.
- Use splints. When you experience discomfort, see a physical therapist. Your therapist may recommend using a splint. Splints, padding, and big-toe supports are designed to keep your toe in a safe position and reduce pressure on it.
- Use orthotics. Your physical therapist may recommend a shoe insert (orthotic). Shoe inserts can help prevent the arch from flattening during walking, and reduce pressure on the big toe. Sometimes, an orthotic needs to be custom made to fit your specific foot.
Your physical therapist can recommend the best solutions for your particular needs.
What Kind of Physical Therapist Do I Need?
All physical therapists are prepared through education and experience to treat bunions. However, you may want to consider:
- A physical therapist with experience treating foot, ankle, and orthopedic conditions. Some physical therapists have a practice with a focus in this area.
- A physical therapist who is a board-certified clinical specialist or who completed a residency or fellowship in orthopedic physical therapy. This therapist has advanced knowledge, experience, and skills that may apply to your condition.
You can find physical therapists who have these and other credentials by using Find a PT, an online tool built by the American Physical Therapy Association. Search for physical therapists by location and expertise.
General tips when you're looking for a physical therapist (or any other health care provider):
- Ask family, friends, and other health care providers to recommend a physical therapist.
- Ask about the physical therapists' experience in helping people who have bunions before you make an appointment.
- Be prepared to describe your symptoms in as much detail as possible, and say what makes them worse.
The American Physical Therapy Association believes that consumers should have access to information that could help them make health care decisions, and also prepare them for a visit with their health care provider.
The following articles provide some of the best scientific evidence related to physical therapy treatment of hallux valgus (bunion). The articles report recent research and give an overview of the standards of practice in the United States and around the world. The article titles are linked either to a PubMed* abstract of the article or to free full text, so that you can read it or print out a copy to bring with you to your health care provider.
Glasoe WM. Treatment of progressive first metatarsophalangeal hallux valgus deformity: a biomechanically based muscle-strengthening approach. J Orthop Sports Phys Ther. 2016;46(7):596–605. Article Summary in PubMed.
Nix SE, Vicenzino BT, Smith MD. Foot pain and functional limitation in healthy adults with hallux valgus: a cross-sectional study. BMC Musculoskelet Disord. 2012;13:197. Article Summary in PubMed.
Weber L. Beyond Bunionectomy: The Role of Physical Therapy. https://lermagazine.com/cover_story/beyond-bunionectomy-the-role-of-physical-therapy. Published August 2010. Accessed December 19, 2019.
*PubMed is a free online resource developed by the National Center for Biotechnology Information (NCBI). PubMed contains millions of citations to biomedical literature, including citations in the National Library of Medicine’s MEDLINE database.
Expert Review:
Dec 17, 2019
Revised:
Dec 29, 2019
Content Type: Guide
Bunion
PT, board-certified clinical specialist in orthopaedic physical therapy
Erin Hayden
PT, DPT, board-certified clinical specialist in orthopaedic physical therapy
Stephen F. Reischl
PT, DPT, board-certified clinical specialist in orthopaedic physical therapy, on behalf of the American Academy of Orthopaedic Physical Therapy
You Might Also Like...
Health Tips
Better Fit, Better Movement and Function: Why Toe Room in Shoes MattersOct 31, 2025
Some shoes can alter the natural walking stride of healthy people and lead to bunions, hammer toes, or other foot and walking problems. This advice from
