Physical Therapy Guide to Posterior Cruciate Ligament Injury
Posterior cruciate ligament injury occurs when one of the ligaments on the inside of the knee is overstretched. PCL injuries are rare, with fewer than 20,000 cases per year diagnosed in the United States. In comparison, there are just over 150,000 anterior cruciate ligament injuries reported in the U.S. each year. The anterior cruciate ligament, ACL, crosses over the PCL within the knee. Accidents that occur when the knee is bent, such as hitting the knee and shinbone against the dashboard during a car crash or falling onto the shins, are common causes of PCL injuries. Skiers, athletes who play sports such as football and soccer, and dancers who leap and land on their shins with bent knees also can experience PCL injuries. Physical therapists treat people with PCL injuries to help reduce their pain, swelling, stiffness, instability, and any related weakness in the knee or lower extremity.
Physical therapists are movement experts who improve quality of life through hands-on care, patient education, and prescribed movement. You can contact a physical therapist directly for an evaluation. To locate a physical therapist in your area, visit Find a PT.
Posterior Cruciate Ligament Injury
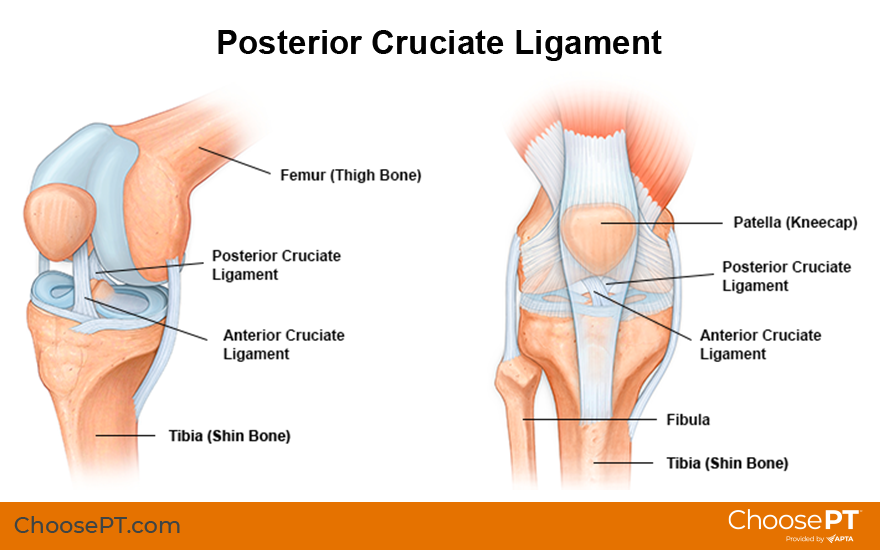
The posterior cruciate ligament is a thick band of tissue deep inside the knee. It connects the thighbone to the shinbone. The PCL prevents the shinbone from sliding too far backward. Any force that pushes the shinbone backward under the thighbone can cause a PCL injury. The PCL may be stretched, partially torn, or completely torn.
Knee injuries that result in a tear to the PCL often can damage other ligaments or cartilage in the knee. A PCL injury also can break a piece of bone loose within the knee. PCL injuries can occur quickly — with a blunt-force injury to the knee — or slowly, due to stresses on the ligament over time.
How Does It Feel?
With an injured PCL, you may experience:
- Sharp or dull pain deep inside the knee joint or the back of the knee.
- Pain in the knee when squatting to lift a heavy load.
- Pain when walking over an unstable surface or longer distances.
- Significant swelling throughout the knee.
- Stiffness in the knee.
- A feeling that the knee will collapse.
- Difficulty going up or down stairs.
- Pain when attempting to run or jump.
PCL injuries will only rarely produce a "popping" sound or sensation when they first occur; for that reason, people may not be sure of the exact time of their injury.
How Is It Diagnosed?
If you see your physical therapist first, they will conduct a thorough evaluation that begins by gathering information about your health history. This may be helped by forms you fill out before your first session. The interview will become more specific as your physical therapist gathers information about your injury and condition. They will assess the degree of your injury to determine the cause or any contributing factors. Your physical therapist may ask you general questions such as:
- How did your injury occur?
- How have you taken care of the condition, such as seeing other health care providers? Have you had imaging or other tests and received their results?
- What are your current symptoms, and how have they changed your typical day and activities?
- Do you have pain, and if so, what is the location and intensity of your pain? Does pain vary during the day?
- Do you have difficulties doing any activities since your injury? What activities are you unable to do?
Your physical therapist will take note of any activities that provoke or make your symptoms worse, as well as anything that reduces your symptoms.
They also will ask questions specific to a PCL injury, which may include:
- Did you feel pain or hear a "pop" when you injured your knee?
- Did your knee straighten out very quickly, past its normal position?
- Did your knee get forcefully bent past its normal position?
- Did you receive a direct hit to the leg while your knee was bent?
- Did you fall on a bent knee with your foot pointed downward?
- Did you see swelling around your knee in the first two to three hours after your injury?
- Does your knee feel like it is wobbling, locking, catching, buckling, or giving way when you try to use it?
This information allows your physical therapist to understand your condition and determine the course of the physical examination.
The physical exam will vary, but most often will begin with observing any movements discussed during the interview. Your physical therapist may:
- Watch how you walk (with or without crutches) or hop on a single leg.
- Assess the mobility (movement) of your knee joint.
- Test the strength of selected muscles in your leg.
- Gently, but skillfully, feel around your knee joint.
- Perform other manual (hands-on) tests to see if there is damage to the PCL.
Your physical therapist may collaborate with an orthopedic doctor or other health care provider. That person may order further tests, such as an X-ray or MRI, to confirm the diagnosis and rule out other damage to your knee, including fracture.
How Can a Physical Therapist Help?
Once the diagnosis is determined, your health care team, which includes your physical therapist and your physicians, will help you make decisions about caring for your injury. Surgery may be suggested, depending on the severity of your injury and whether other structures in your knee are damaged. Physical therapists treat patients with mild to severe PCL injury. Your physical therapist will work with you to design a specific treatment program that will speed your recovery, including exercises you can do at home. Physical therapy will help you return to your normal lifestyle and activities. Every person and injury is different; the time it takes to return to a previous level of function is unique to each individual. Recovery times will vary.
First 24 to 48 Hours
During the first 24 to 48 hours following your injury, your physical therapist may advise you to:
- Rest your knee by using crutches or a brace to reduce the amount of weight you put on your injured leg.
- Avoid any activity that causes pain.
- Apply ice packs to help reduce pain and swelling. Your physical therapist can instruct you on how often and how long to use ice during this time.
- Consult with a doctor for further services such as medication or diagnostic tests.
Treatment Program
Based on the evaluation, your physical therapist will develop a customized treatment program to ensure a safe return to your desired activities. Whether or not you have surgery, this program may include:
- Patient education. Your physical therapist will educate you about your PCL injury to help you understand the healing process. They will work with you to identify and suggest changes or improvements to activities or factors causing your pain, such as the type and amount of exercises you perform, your daily and athletic activities, or your footwear.
- Pain management. Your physical therapist will design a program to address your pain, including applying ice to the affected area. They also may recommend modifying some activities that cause pain. Physical therapists are experts in prescribing pain-management techniques that reduce or eliminate the need for medication, including opioids.
- Range-of-motion exercise. Limited mobility or restriction of your knee, hip, or ankle can cause increased stress on your knee. Your physical therapist may teach you self-stretching techniques to help decrease tension and restore normal motion of the lower extremity joints, from the pelvis/hip region down to the foot.
- Manual therapy. Your physical therapist may treat your condition using hands-on therapy to gently move your muscles and joints. These techniques help improve motion. Through manual therapy, your physical therapist can help guide your knee and lower extremity into a less stressful movement pattern. They also may provide resistance during specific movements or exercises to help you improve your strength.
- Muscle strengthening. Muscle weakness or imbalances can contribute to knee ligament conditions and symptoms. Your physical therapist will design a safe, personalized, and progressive resistance program for you based on your PCL injury level. This program likely will include exercises for your core (midsection) and lower extremity. You may begin by performing strengthening exercises lying on a treatment table, or at home on the bed or floor. You then may advance to doing exercises while standing (such as squats). Your physical therapist will choose the right exercises for you based on your age, physical condition, and goals. This may include using resistance machines in the clinic or at the gym.
- Functional training. Once your pain, strength, and motion improve you will need to safely transition back into more demanding activities. It is important to learn safe, controlled movements to minimize stress on your knee. Based on your movement assessment and goals, your physical therapist will create a series of activities to help you learn how to use and move your body correctly and safely.
- Braces and other assistive devices. Your physical therapist or other members of your health care team may recommend using braces, walking aides, wraps, or tape to assist in your recovery. Their recommendations will be specific to your injury and may include:
- A cane, walker, or crutches to reduce pain and improve your ability to walk. They may recommend using them for a short time or long-term.
- A brace to stabilize your knee during the initial stages of recovery. Your physical therapist will assist you with the proper fit and use of a brace.
- Wrapping your knee to reduce swelling using specific wrapping techniques or compression stockings.
If Surgery Is Necessary
The decision to have surgery is based on multiple factors and should be made by the patient in consultation with an orthopedic surgeon. Recommending surgery is outside the scope of practice for physical therapists. A surgeon will consider your health status, goals, and specific factors that may indicate the need for surgery, such as whether you have:
- A piece of bone that has broken loose inside your knee joint.
- Other ligament or cartilage injuries.
- A constant feeling that your knee is going to buckle beneath you.
Athletes and individuals intending to return to high-demand activities may elect to have surgery to repair their PCL to improve their knee stability. If you have injuries to other structures in the knee at the same time as a PCL injury, you may need a separate strategy to treat those injuries, which could include different types of surgery.
If you have surgery, you will follow a recovery program guided by your physical therapist and surgeon. This program may begin one week after surgery and last through full recovery (which can take two to three months, depending on your injury). Your physical therapist will help you minimize pain, regain motion and strength, and return to normal activities in the safest and fastest manner possible.
Can This Injury or Condition Be Prevented?
Your physical therapist can recommend a home-exercise program to help strengthen and stretch the muscles around your knee, upper leg, and abdomen to prevent future injury. These may include strength and flexibility exercises for the leg, knee, and core muscles.
To help prevent a recurrence of your PCL injury, your physical therapist may advise you to:
- Always use a seat belt to help prevent injury during a car accident.
- Position your car seat so that it is not too close to the dashboard.
- Avoid intentionally landing on the front of your shinbone or your knees.
- Always warm up before starting a sport or heavy physical activity.
- Maintain or improve sport-specific conditioning and techniques that are right for your level of activity.
- Wear shoes that are in good condition and fit well.
- Maintain a healthy weight.
What Kind of Physical Therapist Do I Need?
All physical therapists are prepared through education and experience to treat PCL injury. However, you may want to consider:
- A physical therapist who is experienced in treating people with orthopedic injuries. Some physical therapists have a practice with an orthopedic focus.
- A physical therapist who is a board-certified clinical specialist or who completed a residency or fellowship in orthopaedic or sports physical therapy. This physical therapist has advanced knowledge, experience, and skills that may apply to your condition.
You can find physical therapists with these and other credentials by using Find a PT, the online tool built by the American Physical Therapy Association, to help you search for physical therapists with specific clinical expertise in your geographic area.
General tips when you are looking for a physical therapist (or any other health care provider):
- Get recommendations from family, friends, or other health care providers.
- When you contact a physical therapy clinic for an appointment, ask about the physical therapists' experience in helping people who have your type of injury.
- Be prepared to describe your symptoms in as much detail as possible, and say what makes your symptoms worse.
The American Physical Therapy Association believes that consumers should have access to information to help them make health care decisions and prepare them for a visit with their health care provider.
The following articles provide some of the best scientific evidence related to physical therapy treatment of your injury. The articles report recent research and give an overview of the standards of practice both in the United States and internationally. The article titles link to a PubMed* abstract of the article that may offer free full text so that you can read it or print out a copy to bring with you to your health care provider.
Rauck R, Nwachuka BA, Allen AA, Warren RF, et al. Outcome of isolated posterior cruciate ligament reconstruction at mean 6.3-year follow up: a consecutive case series. Phys Sportsmed. 2019;47(1):60–64. Article Summary in PubMed.
Pache S, Aman ZS, Kennedy M, Nakama GY, et al. Posterior cruciate ligament: current concepts. Arch Bone Jt Surg. 2018;6(1):8–18. Article Summary in PubMed.
Senese M, Greenberg E, Lawrence JT, Ganley T. Rehabilitation following isolated posterior cruciate ligament reconstruction: a literature review of published protocols. Int J Sports Phy Ther. 2018;13(4):737–751. Article Summary in PubMed.
Bedi A, Musahl V, Cowan JB. Management of posterior cruciate ligament injuries: an evidence-based review. J Am Acad Orthop Surg. 2016;(5)24:277–289. Article Summary in PubMed.
Kim JG, Lee YS, Yang BS, et al. Rehabilitation after posterior cruciate ligament reconstruction: a review of the literature and theoretical support. Arch Orthop Trauma Surg. 2013;133(12):1687–1695. Article Summary in PubMed.
Rosenthal MD, Rainey CE, Tognoni A, Worms R. Evaluation and management of posterior cruciate ligament injuries. Phys Ther Sport. 2012;13(4):196–208. Article Summary in PubMed.
*PubMed is a free online resource developed by the National Center for Biotechnology Information. PubMed contains millions of citations to biomedical literature, including citations in the National Library of Medicine's MEDLINE database.
Expert Review:
Aug 31, 2020
Revised:
Aug 31, 2020
Content Type: Guide
Posterior Cruciate Ligament Injury
PT, DPT
Daniel Farwell
PT, DPT, board-certified clinical specialist in sports physical therapy
Stephen F. Reischl
PT, DPT, board-certified clinical specialist in orthopaedic physical therapy, on behalf of the Academy of Orthopaedic Physical Therapy