Physical Therapy Guide to Wounds and Wound Care
A wound or skin injury can occur for many different reasons. It could be due to an accident, injury, surgery, a burn, circulation problems, diabetes, or spending too much time in one position (not moving enough). When you add all of these different causes together, wounds affect more than 1 million people every year. Physical therapists can help people prevent wounds. They also can help heal wounds by providing advanced wound-care treatments and prescribing specific exercises and activities.
Physical therapists are movement experts who improve quality of life through hands-on care, patient education, and prescribed movement. You can contact a physical therapist directly for an evaluation. To locate a physical therapist in your area, visit Find a PT.
What Are Wounds?
Wounds result from a number of different causes. A physical therapist can assist with any type of wound. It is important to note that anytime you have a break in the skin, there is a potential for infection. You should seek treatment for any wound sooner rather than later.
There are four main categories of wounds:
- Arterial wounds. People with peripheral artery disease typically have decreased blood flow to their legs and feet. This condition can worsen over time. When there is not enough blood flow to the tissue, wounds can occur more easily and often take much longer to heal.
- Diabetic wounds (also known as diabetic foot ulcers). People who have diabetes can develop structural and sensation changes in their feet. These changes make a person with diabetes more likely to develop wounds. Wounds in people with diabetes are often located on the bottom of the feet, but they also can occur in other areas of the foot. They often result from shoes that don’t fit well or stepping on an object without realizing it.
- Pressure injuries. This type of wound occurs often in people who are bedridden, or are not able to move or change positions very well on their own. These wounds also can occur beneath applied medical equipment like splints or items used in a hospital (tubing, positioning devices, etc.).
- Venous wounds.With chronic venous disease, problems with circulation cause difficulty pumping fluid away from the legs, causing swelling. This swelling can cause breaks in the skin or make it much harder for external cuts or scrapes to heal.
Signs and Symptoms
Some wounds can be quite painful and are easy to identify. Other types of wounds may not hurt at all. It is important for people with diabetes and older adults, or anyone who does not move much, to conduct regular close visual skin inspections. These can be done by themselves or others to determine if a wound is present.
During inspection, you or your caregiver should look for:
- Breaks in the skin.
- Drainage.
- Changes in skin color (pink or red tones on light skin; darker than normal tones on darker skin).
- New feelings of pain or a painful area (even if it is not an open wound).
- Temperature changes where one area of the skin feels warmer to touch.
If you have any of these symptoms, seek help. These are all signs that should be explored further by a physical therapist or other health care provider.
How Is It Diagnosed?
A physical therapist will conduct a full evaluation, including measuring the wound area and inspecting the surrounding skin. Range of motion, mobility, and strength also will be assessed, as these can contribute to the wound problem, and may assist in the healing process. Your physical therapist also may perform specific testing related to circulation and sensation; you may need additional testing from a doctor as well.
How Can a Physical Therapist Help?
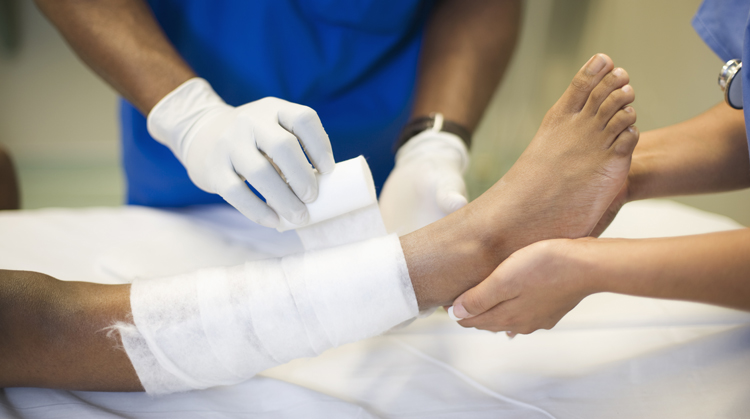
Physical therapists are skilled in managing all types of wounds. Based on the results of your physical therapist's evaluation, including a review of your medical history and an examination of the wound, they will design a treatment program to meet your needs and goals. Your treatment may include:
- Patient education.
- Strengthening and mobility exercises.
- Wound care.
- Recommending improvements to the seat, bed, or footwear.
- Caregiver training.
Your physical therapist also may work with other health care providers to ensure the safest and most effective healing process possible. Your physical therapist can:
Train family and caregivers. Many wounds can benefit from specific inspection techniques and adjusting body position. When people are unable to safely perform these tasks on their own, family or caregivers may be trained to help with these activities. Physical therapists are experts in positioning people on different surfaces, including beds, wheelchairs, toilets, bedside toilets, or other types of chairs and furniture. They also are skilled in making transfers (moving a person from one surface to another). Your physical therapist can train family members and caregivers to safely perform positioning and transfers, and also teach them skin and wound inspection techniques.
Improve strength and movement. In many cases, wounds are made worse by weakness and/or decreased ability to move. Your physical therapist will develop an exercise program so that the person with a wound can move around their environment as safely as possible without harm. In some cases, exercising and being active will help speed the healing process.
Care for wounds. Physical therapists are trained in wound care and know how to remove dead tissue from a wound (debridement). In extreme cases, debridement may require general anesthesia and be performed by a surgeon.
Wounds require proper dressings to aid healing. Dressings include a suitable material to cover wounds and to fill deeper wounds. Other treatments also may be needed.
These can include:
- Compression wrapping.
- Casting.
- Use of specialized ultrasound, negative pressure, or electrical stimulation.
Your physical therapist will evaluate your wound with each visit and determine the type of dressing and/or treatment to use and how often it should be done. In some cases, your physical therapist will train your caregivers in how to clean wounds and change dressings. As a wound heals, the treatment will likely change.
Your physical therapist will discuss with you:
- What to expect in terms of normal wound healing.
- Signs to look for between visits that might indicate a problem.
- When to contact a physician or seek emergency medical services.
Improve sitting/lying surfaces and footwear. The surface on which a person lies, sits, or walks may contribute to wounds. Your physical therapist will examine the types of surfaces you use and, if needed, make recommendations for something different. There are special materials that can be used to reduce or remove the amount of weight or pressure for a person who is sitting, lying down, or standing.
Communicate with other health care providers. Several health care providers may be involved in the care of a person with a wound. Your physical therapist will communicate and coordinate care with doctors, nurses, dietitians, and others, as needed. This teamwork will help ensure safe and effective healing, and help prevent new skin breakdown.
Can This Injury or Condition Be Prevented?
Engaging in the right type of activity and/or exercise can help prevent many wounds. Physical therapists are movement experts and can design the right exercise program based on a person’s current wounds and/or risk factors. In addition, exercise and physical activity can help to address many underlying conditions related to wounds, such as:
- Diabetes.
- Peripheral artery disease.
- Peripheral neuropathy.
What Kind of Physical Therapist Do I Need?
All physical therapists are prepared through education and experience to treat patients who have wounds. You may want to consider:
- A physical therapist who is experienced in treating people with wound problems. Some physical therapists have a practice with a wound-care focus.
- A physical therapist who is a board-certified clinical specialist, who completed a residency in wound management physical therapy, or who holds a certified wound specialist credential. This physical therapist has advanced knowledge, experience, and skills that may apply to your condition.
You can find physical therapists who have these and other credentials by using Find a PT, the online tool built by the American Physical Therapy Association to help you search for physical therapists with specific clinical expertise in your geographic area.
General tips when you're looking for a physical therapist (or any other health care provider):
- Get recommendations from family, friends, or other health care providers.
- When you contact a physical therapy clinic for an appointment, ask about the physical therapists' experience in helping people with wounds.
- During your first visit with the physical therapist, be prepared to describe your symptoms in as much detail as possible, and say what makes your symptoms worse.
The following resources offer some of the best scientific evidence related to physical therapy treatment for people who experience wounds or have conditions that increase their risk for developing them. They report recent research and give an overview of the standards of practice both in the United States and internationally. They link to a PubMed* abstract of articles, which also may offer free access to the full text or to other resources, so that you can read them or print out a copy to bring with you to your health care provider.
National Pressure Injury Advisory Panel. npiap.com. Accessed February 1, 2021.
Harris-Hayes M, Schootman M, Schootman JC, Hastings MK. The role of physical therapists in fighting the type 2 diabetes epidemic. J Orthop Sports Phys Ther. 2020;50(1):5–16. Article Summary in PubMed.
Johnson CE, Takemoto JK. A review of beneficial low-intensity exercises in diabetic peripheral neuropathy patients. J Pharm Pharm Sci. 2019;22(1):22–27. Article Summary in PubMed.
Jull A, Slark J, Parsons J. Prescribed exercise with compression vs compression alone in treating patients with venous leg ulcers: a systematic review and meta-analysis. JAMA Dermatol. 2018;154(11):1304–1311. Article Summary in PubMed.
Walsworth MK, de Bie R, Figoni SF, O'Connell JB. Peripheral artery disease: what you need to know. J Orthop Sports Phys Ther. 2017;47(12):957–964. Article Summary in PubMed.
Colberg SR, Sigal RJ, Yardley JE, et al. Physical activity/exercise and diabetes: a position statement of the American Diabetes Association. Diabetes Care. 2016;39(11):2065–2079. Article Summary in PubMed.
Waryasz GR, McDermott AY. Exercise prescription and the patient with type 2 diabetes: a clinical approach to optimizing patient outcomes. J Am Acad Nurse Pract. 2010;22(4):217–227. Article Summary in PubMed.
Reddy M, Gill SS, Kalkar SR, Wu W, Anderson PJ, Rochon PA. Treatment of pressure ulcers: a systematic review. JAMA. 2008;300(22):2647–2662. Article Summary in PubMed.
Expert Review:
Jan 15, 2021
Revised:
Jan 15, 2021
Content Type: Guide
Wounds and Wound Care
Stephanie Woelfel
PT, DPT, certified wound specialist, on behalf of the APTA Academy of Clinical Electrophysiology & Wound Management
You Might Also Like...
Article
Wound Management in Physical TherapyJul 8, 2024
Physical therapists who are wound management specialists have additional skills and expertise to provide wound healing treatments. Learn more about wound
Patient Stories
Wounded Warrior Looks to Motivate Others through RecoveryJul 29, 2021
David was a 20-year-old Army cavalry scout when he was shot by a sniper in both legs while serving as the lead driver for his platoon.
Patient Stories
Man Who Lost 300 Pounds Credits Physical Therapist With Transforming His LifeJul 28, 2021
Scott was was 50 years old, 520 pounds, and depressed. He found hope and better health through physical therapy.


