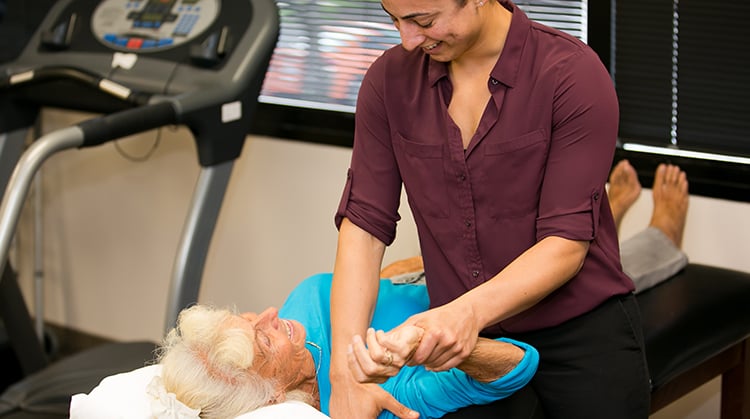
Shoulder replacement (also known as shoulder arthroplasty) is a major surgery in which all or part of the shoulder joint is replaced. This surgery is only done when other conservative treatments no longer provide pain relief or when severe pain limits your ability to use your shoulder. Shoulder replacement surgery can address pain and improve the use of your shoulder, but the recovery time is often significant and requires some work to get the full benefit of the surgery.
If you or someone you know needs shoulder replacement surgery, knowing what to expect can help you have a better outcome.
Here are four things to know:
1. Managing pain after surgery.
You can expect some pain after shoulder replacement or any major surgery. Your pain should decrease as you heal. Most people report barely noticeable to mild pain after they have fully recovered from shoulder replacement surgery through targeted physical therapy. Many people report a great improvement from the pain that they experienced before surgery.
Work with your physical therapist to learn positions and exercises that reduce pain and help you heal. Work with your surgeon and pharmacist to understand how to safely use pain medications after surgery. If your surgeon prescribes opioid medications after surgery, it is important to have a plan to decrease their use in a timely manner.
Research shows that taking prescribed opioids before surgery leads to worse pain management after surgery. Consider weaning off these medicines prior to surgery with the supervision of your health care team. This can help with your pain management after surgery.
2. An initial need for help and assistance.
You can expect to be in a sling for a few weeks. You will not be able to use your arm for anything except prescribed exercises. Your PT will teach you specific exercises to promote healing.
Consider having ready-to-eat meals that are easy to prepare. You may want to set up things at home that you need regularly at an easy-to-reach level. Button-up shirts are easiest to wear while you cannot lift your arm.
Let your friends or family know that you are having major surgery, so they can support you while you recover.
3. Difficulty sleeping.
Initially, sleep may be difficult after surgery but can improve with good habits. Good sleep habits, also known as sleep hygiene, include:
- Avoiding large meals and caffeine before bedtime.
- Limiting or avoiding alcohol.
- Avoiding nicotine.
- Removing electronic devices from the bedroom.
- Having a regular set bedtime.
Finding a well-supported position also will be important. Talk with your physical therapist about positions to keep your shoulder protected while you sleep.
4. Improved mobility and function.
Physical therapy is a critical part of recovery after shoulder replacement surgery. Before surgery, a physical therapist can help you improve your shoulder and upper back movement to keep your shoulder as strong and mobile as possible until the time of surgery.
After surgery, a hospital physical therapist will educate you about what precautions to take when you go home and what movements to avoid during the initial healing phase. They also will teach you how to get in and out of bed while protecting your shoulder.
After discharge, continuing physical therapy is very important to ensure your safe recovery. Your physical therapist will work with you to progress your exercises at the right times in the healing process. They will help you get back your range of motion, improve your strength and function, and eventually help you get back to your everyday activities, job, or sport.
Be sure to tell your physical therapist your goals, so both of you can focus on what is important to you.
Physical therapists are movement experts who improve quality of life through hands-on care, patient education, and prescribed movement. You can contact a physical therapist directly for an evaluation. To find a physical therapist in your area, visit Find a PT.


