Physical Therapy Guide to Benign Paroxysmal Positional Vertigo (BPPV)
Every year, millions of people in the United States develop vertigo. Vertigo is a feeling that you or your surroundings are spinning. This sensation can be alarming and may increase the risk of falling. Benign paroxysmal positional vertigo is one of the most common types of vertigo. If you have BPPV, you are not alone. At least nine out of every 100 older adults are affected by it. The good news is that BPPV is treatable. Your physical therapist will use tests to confirm vertigo. They will teach you specific exercises and use special maneuvers to help you get back to the activities that you enjoy.
Physical therapists are movement experts. They improve quality of life through hands-on care, patient education, and prescribed movement. You can contact a physical therapist directly for an evaluation. To find a physical therapist in your area, visit Find a PT.
What Is BPPV?
Benign Paroxysmal Positional Vertigo is a common inner ear problem that affects the vestibular system. This system works to maintain your balance. BPPV causes short periods of dizziness when moving your head into certain positions. It is more common in females and may be hereditary.
Benign means that this disorder is not life-threatening. Paroxysmal means that the spinning sensation occurs suddenly. Positional means that symptoms are triggered by changes in head position, such as when lying down, turning over in bed, or looking up. This dizzy or spinning sensation is called vertigo.
Inside the inner ear, there is a layer of calcium carbonate material called otoconia. People often refer to pieces of the otoconia as crystals. BPPV occurs when these crystals break off and move to a part of the inner ear called the semicircular canal.
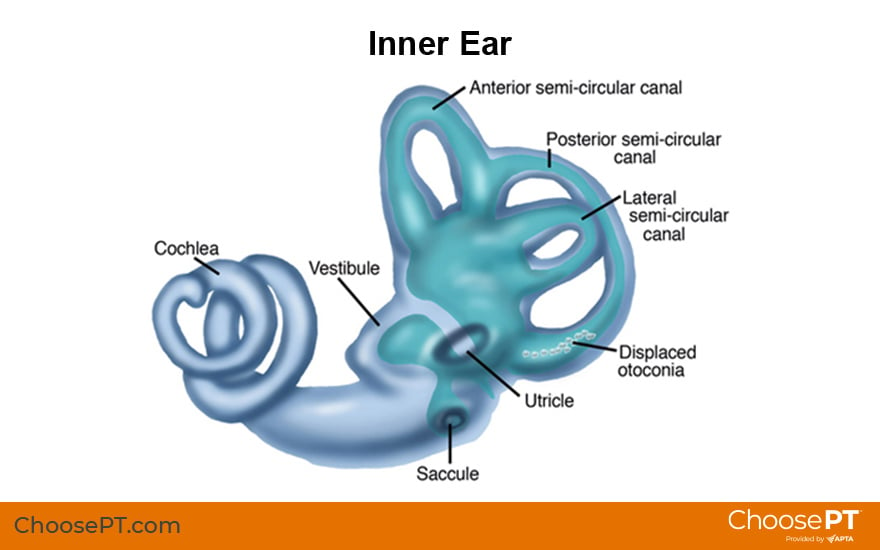
When you move your head a certain way, the crystals move inside the canal and stimulate nerve endings. This causes you to become dizzy. Crystals may become loose due to:
- Trauma to the head.
- Infection.
- Conditions such as Meniere disease.
- Aging.
Most often, the cause of BPPV is not known.
How Does It Feel?
BPPV occurs most commonly after a position change. This dizzy sensation is brief and intense and usually lasts for about 15 to 45 seconds.
Some changes in position that may cause your symptoms include:
- Lying down.
- Turning over in bed.
- Bending over.
- Looking up.
Symptoms may last longer if the crystals become stuck to part of the inner ear. Episodes of vertigo frequently occur for weeks or months at a time. When vertigo occurs, you may feel like the room is spinning around you. You also may feel light-headed, off-balance, or nauseous.
Signs and Symptoms
The signs and symptoms of BPPV usually last less than one minute. They may come and go. They also may go away for a while and then come back. A change in head position often triggers symptoms. Symptoms may include:
- Dizziness .
- A sense that you or your surroundings are spinning or moving (vertigo).
- A loss of balance.
- Unsteadiness.
- Nausea.
- Vomiting.
How Is It Diagnosed?
BPPV is diagnosed if you have a particular kind of involuntary eye movement called nystagmus, and whether you have vertigo when your head is moved into certain positions. Your physical therapist will perform tests to see whether vertigo and involuntary eye movement are present.
Physical therapists use positional tests to recreate BPPV symptoms. These tests require moving your head in specific ways. They will help your physical therapist determine the cause and type of your dizziness. During these tests, your physical therapist will watch your eyes for specific movements. This will help them determine the right treatment maneuver to reduce or eliminate your vertigo.
There are many causes of dizziness. Dizziness is often hard for people to describe. This can make the source of dizziness challenging to diagnose.
It is important to be as specific as possible when describing your symptoms to your health care provider.
For example, explain if you have light-headedness or if you see or feel the room spinning during an episode. And describe how long your symptoms last (seconds, minutes, hours, or days). Do your best to explain what makes your dizziness better or worse. For example, is your dizziness made worse by movement or position changes? Is your dizziness eased by stillness or rest?
Be sure to discuss any recent illnesses or injuries, problems with your immune system, changes in medications or hormones, and whether you have headaches. These clues will help your physical therapist make an accurate diagnosis, or indicate the need for a referral to another specialist.
How Can a Physical Therapist Help?

Fortunately, the majority of people with BPPV can be treated with simple and specific maneuvers that involve moving the head and body. Your physical therapist will perform an evaluation and determine which maneuver is right for you. These maneuvers are designed to move the crystals from the semicircular canal back into the appropriate area in the inner ear (the utricle).
No medication has been found to cure BPPV. In some cases, medicine can actually delay recovery.
Most cases of BPPV can be managed with treatment maneuvers by a physical therapist. In very rare cases, a surgical procedure called a posterior canal plugging may be considered. Surgery for BPPV is very rare.
Can This Injury or Condition Be Prevented?
There are no known ways to prevent BPPV. After treatment, symptoms can return if new crystals break off and get into the semicircular canal. Some people report that their BPPV symptoms recur predictably, perhaps seasonally, or with changes in the weather. Within three years of having a bout of BPPV, symptoms will return for about 50% of people.
If BPPV results from head trauma, it is more likely to recur. Although your BPPV may return, you will be able to recognize the symptoms and keep yourself safe until you can get help. Your physical therapist will apply the appropriate maneuver to return the crystals to their correct position in the inner ear. They also may teach you exercises that can reduce or end your symptoms and improve your balance.
What Kind of Physical Therapist Do I Need?
Physical therapists use their education and experience to evaluate and treat dizziness and imbalance. You may want to consider:
- A physical therapist who is experienced in treating people with neurological problems.
- A physical therapist with specialized training and experience in vestibular rehabilitation.
- A physical therapist who is a board-certified neurological clinical specialist, who completed a residency or fellowship in neurologic physical therapy, or who has advanced knowledge, experience, and skills that may apply to your condition.
You can find physical therapists who have these and other credentials by using Find a PT, the online tool built by the American Physical Therapy Association to help you search for physical therapists with specific clinical expertise in your geographic area.
General tips when you're looking for a physical therapist (or any other health care provider):
- Get recommendations from family, friends, or from other health care providers.
- When you contact a physical therapy clinic for an appointment, ask about the physical therapists' experience in helping people with inner ear problems.
- Be prepared to describe your symptoms in as much detail as possible and say what makes your symptoms better or worse.
The American Physical Therapy Association believes that consumers should have access to information that could help them make health care decisions and also prepare them for a visit with a health care provider.
The following articles provide some of the best scientific evidence about treatment of BPPV. The articles report recent research and give an overview of the standards of practice for treatment both in the United States and around the world. The article titles are linked either to a PubMed abstract of the article or to free full text, so that you can read it or print out a copy to bring with you to your health care provider.
Vestibular Disorders Association. Benign paroxysmal positional vertigo (BPPV). Accessed January 13, 2020.
Bhattacharyya N, Gubbels SP, Schwartz SR, et al. Clinical practice guideline: benign paroxysmal positional vertigo (update). Otolaryngol Head Neck Surg. 2017;156(3_suppl):S1–S47. Article summary in PubMed.
* PubMed is a free online resource developed by the National Center for Biotechnology Information. PubMed contains millions of citations to biomedical literature, including citations in the National Library of Medicine’s MEDLINE database.
Expert Review:
Mar 15, 2020
Revised:
Jul 8, 2020
Content Type: Guide
Benign Paroxysmal Positional Vertigo (BPPV)
PT, PhD
PT, DPT
PT, DPT
PT, PhD, board-certified clinical specialist in neurologic physical therapy
Carrie W. Hoppes
PT, PhD, board-certified clinical specialist in neurologic and orthopaedic physical therapy
Karen H. Lambert
PT, DPT, board-certified clinical specialist in neurologic physical therapy