Physical Therapy Guide to Hip Impingement (Femoroacetabular Impingement)
Hip impingement, or femoroacetabular impingement, involves a change in the shape of the surface of the hip joint. It can lead to stiffness, pain, and damage of the tissue and/or bone. It most often occurs in young, active people. Conditions that cause hip impingement can be present at birth or develop over time. It affects men and women. Physical therapists help people with hip impingement regain movement, flexibility, and strength, and return to their regular activities and sport.
Physical therapists are movement experts. They improve quality of life through hands-on care, patient education, and prescribed movement. You can contact a physical therapist directly for an evaluation. To find a physical therapist in your area, visit Find a PT.
What Is Hip Impingement?
The two types of hip impingement, "pincer" and "cam," may occur alone or together. Hip impingement usually affects people who are younger than 50. It may precede hip osteoarthritis.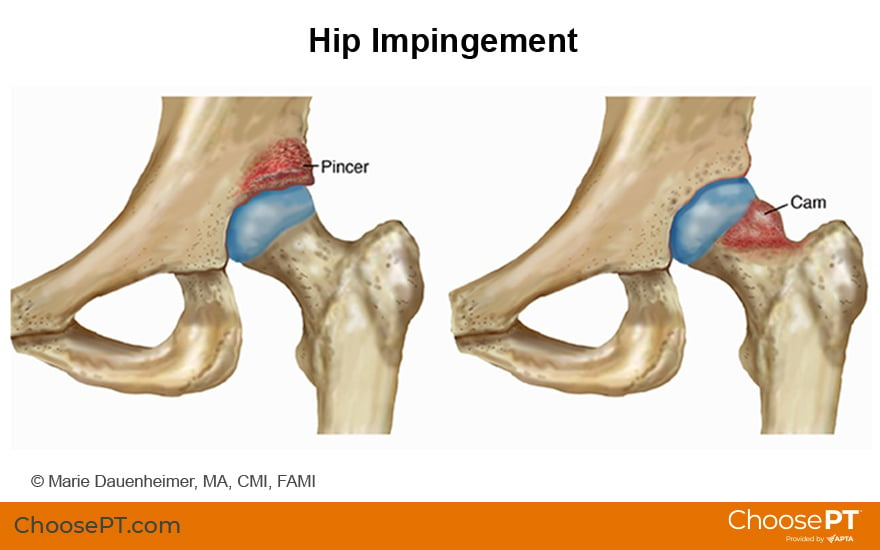
Pincer-Type Impingement
Pincer-type impingements affect men and women. This type may result when:
- The hip socket, which is typically angled forward, angles toward the back.
- Protruding bone develops on the pelvis. This makes the hip socket deeper so that it covers more of the ball or head of the femur bone.
Regardless of the cause, pincer-type impingements pinch the labrum, a rim of connective tissue around the edge of the hip socket. This pinching happens especially when flexing the hip (moving the leg up). Over time this extra pressure leads to wear and tear that can cause inflammation. Sometimes it causes a labrum tear. If this condition persists, the cartilage that lines the hip joint may become worn, form holes, and develop bone spurs.
Cam-Type Impingement
Cam-type impingements affect men more often than women and may result when:
- The shape of the bone around the head of the femur (the ball at the top of the thigh bone) is misshaped. This deformity can be due to:
- Variation of the "normal" shape of the head of the femur. This may be present at birth or can develop over time.
- Bone that is overgrown at the top and front of the femur head. The nickname "pistol grip" deformity often describes this bony overgrowth on X-rays.
- The overgrown or misshapen bone contacts the cartilage that lines the hip socket, possibly causing it to peel away from the bone in the socket. The labrum can become worn, frayed, or torn as well.
Signs and Symptoms
Hip impingement may cause you to experience:
- Pain that begins gradually and may worsen with time. People with hip impingement often describe their pain by making a "C" with the thumb and hand and placing it on the fold at the front and side of the hip. This is called the "C” sign.
- Groin pain or discomfort in the outside of the hip, thigh, low back, or buttocks.
- Sharp, stabbing pain when squatting, sitting and standing, or performing athletic moves like running, "cutting," jumping, twisting, pivoting, or moving side to side.
- Loss of motion or a stiff feeling when rotating your leg inward and/or lifting your leg.
- Pain that increases after sitting for long periods or leaning forward.
How Is It Diagnosed?
Your physical therapist will interview you to learn when and how your symptoms first began. They also will ask how your symptoms affect your daily life. They will discuss your goals for physical therapy and work with you on how best to achieve them.
Your physical therapist will perform an exam, which may include:
- Watching you walk and noting any abnormalities.
- Observing movements that are difficult, but not painful, for you to do (such as squatting).
- Evaluating the range of motion (movement) of both hips, lower extremities (everything from your hips to your toes), and trunk.
- Assessing the strength of both hips, lower extremities, and trunk.
- Checking your balance and coordination for each lower extremity.
- Testing the flexibility of each hip and other joints of the lower extremity.
- Performing special tests to help determine whether the hip is the source of your symptoms. For instance, your physical therapist may gently roll your leg in and out (the "log roll" test), or bend your hip up and inward while turning the lower leg out to the side (the FADDIR test) to help determine the source of your condition.
For a firm diagnosis, your doctor may order tests to help identify any changes in the joint or labrum. These tests may include X-rays or an MRI. A diagnosis of hip impingement may take some time, especially if you also have low back, buttock, or pelvic pain.
How Can a Physical Therapist Help?
Your physical therapist will conduct a thorough examination, including taking a detailed history, and may prescribe stretches and strengthening exercises to balance the muscles around your hip. They may use manual (hands-on) therapy to help restore your hip's range of motion. Your physical therapist also may discuss making changes to your activities and lifestyle to help improve function and decrease your pain.
Without Surgery
Physical therapy may be beneficial for people with low-level hip pain and/or disability. Conservative care aims to:
- Ease pain and discomfort.
- Address individual limitations.
- Improve overall function.
Your physical therapist may use some or all of the following approaches to help you achieve these goals. They may help you avoid the need for surgery or delay your condition getting worse. Your treatment may include:
Modifying your daily, job-related, and sports activities. Your physical therapist will recommend and discuss specific positions and activities for you to avoid or modify. These will be designed to protect your hip. They may recommend limiting how often you bend at the hip to avoid further hip damage. To minimize tension on the hip, your physical therapist will teach you safe, controlled movements.
Improving lower-extremity muscle flexibility and joint movement. Stretching tight muscles. Stretching the hip directly can reduce abnormal forces that cause pain with motion. Stretching other body regions (trunk, leg, ankle, or foot), also may decrease stress at the hip.
Joint mobilization. Your physical therapist may gently move your hip to help ease pain. This may improve your ability to stretch or extend your hip joint.
Improving the strength of your lower extremities and trunk. Strengthening the hips and trunk can reduce abnormal forces on the already injured joint. Your physical therapist will help you develop movement strategies to compensate for the injured hip joint.
Improving lower-extremity balance and coordination. Your physical therapist will prescribe exercises to help improve balance and coordinating movements. These can minimize forces and stress on the hip joint.
Home exercise program. Your physical therapist will design a specific home exercise program based on your needs and goals for you to do on your own. These will help you to stay strong and healthy safely, once your physical therapy visits have ended.
Functional training. Once your pain, strength, and motion improve, you will be able to slowly return to more demanding activities. Based on your unique needs and goals, your physical therapist will create a series of activities for you to do. They will help you learn how to use and move your body correctly and safely during your daily, work, and sports activities.
Following Surgery
Surgery for hip impingement is performed using arthroscopy. Arthroscopy is minimally invasive and only requires small incisions in the skin. The surgeon will insert pencil-sized instruments into the joint to repair the damage. The surgeon may perform one or more techniques during surgery as needed.
After surgery, physical therapy will depend on the type of procedure performed. On your first visit with a physical therapist, they will go over your history thoroughly and perform a physical exam (within the limits set by your surgeon). During later visits, your physical therapist may provide the following treatments:
Education. Your physical therapist will educate you about your condition.
- Postsurgical wound care: You will learn how to watch for signs of infection and learn how to keep your wound clean.
- Restrictions: Your physical therapist will go over any restrictions your surgeon has given you.
- Brace: Your physical therapist will teach you how to put on and remove any brace prescribed by your surgeon, and explain the reasons for using the brace.
Gait training. Your physical therapist will teach you how to walk with an assistive device (such as crutches or a walker) if needed. They will teach you how to avoid putting too much weight on your hip as it heals.
Range-of-motion exercises. Initially, hip range-of-motion exercises will be gently performed for you by your physical therapist. As you heal, your physical therapist may teach you active range-of-motion exercises for you to do on your own.
Flexibility exercises. Your physical therapist may teach you stretching exercises for the entire lower extremity and your trunk.
Strengthening exercises. At the appropriate time, your physical therapist will teach you how to do the following types of strengthening exercises:
- Isometric strengthening: tensing and relaxing your muscles.
- Isotonic strengthening: tensing and moving your muscles (such as bending your knee).
- Eccentric strengthening: tensing your muscles to move your hip joint safely.
Balance and coordination exercises. Your physical therapist will teach you how exercises to improve your balance and coordination.
Job- or activity-specific training. As you regain strength and movement, your physical therapist may add more specific exercises. Doing these will help prepare you to return to your work and sports activities.
Most people return to normal daily activities around three months after surgery. Returning to high-level activities and sports may take four to six months after surgery. Your physical therapist will recommend a gradual return to your regular activities based on your condition. Research shows that about 74% of athletes return to their prior playing ability after rehabilitation from this type of hip surgery. Each person is different. How long it takes to return to your desired activities will depend on the surgery performed and your sport.
Can This Injury or Condition Be Prevented?
Currently, there are no recommendations to prevent hip impingement. Despite a significant increase in research to learn more about this condition, there is a great deal that is unknown. For example, many active young people whose X-rays show abnormal hips do not have pain, despite active lives and playing sports.
However, evidence shows that physical therapy treatment, along with anti-inflammatory medicines, can:
- Decrease pain.
- Slow joint damage.
- Improve function.
Physical therapy is very important for people who:
- Have mild hip impingement.
- Wish to avoid surgery.
- Are not candidates for surgery.
What Kind of Physical Therapist Do I Need?
All physical therapists are prepared through education and experience to treat patients who have hip impingement. You may want to consider:
- A physical therapist who is experienced in treating people with musculoskeletal problems. Some physical therapists have a practice with a sports or orthopedic focus.
- A physical therapist who is a board-certified clinical specialist or who completed a residency or fellowship in sports or orthopedic physical therapy. This physical therapist has advanced knowledge, experience, and skills that may apply to your condition.
You can find physical therapists who have these and other credentials by using Find a PT, the online tool built by the American Physical Therapy Association to help you search for physical therapists with specific clinical expertise in your geographic area.
General tips when you are looking for a physical therapist (or any other health care provider):
- Get recommendations from family, friends, or other health care providers.
- When you contact a physical therapy clinic for an appointment, ask about the physical therapists' experience in helping people with hip impingement.
- Be prepared to describe your symptoms in as much detail as possible, and say what makes your symptoms worse.
The American Physical Therapy Association believes that consumers should have access to information to help them make health care decisions and prepare them for their visit with their health care provider.
The following articles provide some of the best scientific evidence related to physical therapy treatment of problems related to hip impingement. The articles report recent research and give an overview of the standards of practice for treatment both in the United States and internationally. They link to a PubMed* abstract that may offer free full text so that you can read it or print out a copy to bring with you to your health care provider.
Reiman MP, Peters S, Sylvain J, Hagymasi S, Mather RC, Goode AP. Femoroacetabular impingement surgery allows 74% of athletes to return to the same competitive level of sports participation but their level of performance remains unreported: a systematic review with meta-analysis. Br J Sports Med. 2018;52(15):972–981. Article Summary in PubMed .
Shaw C. Femoroacetabular impingement syndrome: a cause of hip pain in adolescents and young adults [published correction appears in Mo Med. 2017;114(5):352]. Mo Med. 2017;114(4):299–302. Article Summary in PubMed.
Amanatullah DF, Antkowiak T, Pillay K, et al. Femoroacetabular impingement: current concepts in diagnosis and treatment. Orthopedics. 2015;38(3):185–199. Article Summary in PubMed.
Enseki K, Harris-Hayes M, White DM, et al. Nonarthritic hip joint pain. J Orthop Sports Phys Ther. 2014;44(6):A1–A32. Article Summary in PubMed.
*PubMed is a free online resource developed by the National Center for Biotechnology Information. PubMed contains millions of citations to biomedical literature, including citations in the National Library of Medicine's MEDLINE database.
Expert Review:
Jul 19, 2020
Revised:
Jul 19, 2020
Content Type: Guide
Hip Impingement
Jennifer Miller, PT, MPT, board-certified clinical specialist in sports physical therapy
Lica Noceti-DeWit
PT, DPT, board-certified clinical specialist in orthopaedic and sports physical therapy
Stephen F. Reischl
PT, DPT, board-certified clinical specialist in orthopaedic physical therapy, on behalf of the Academy of Orthopaedic Physical Therapy
You Might Also Like...
Podcast
Success Story: Physical Therapist Collaborates With Surgeon For Hip ImpingementJun 29, 2017
The pain that Annie Karp felt in her hip wasn't intense, but it was unrelenting. She had no success with treatment, until a physical therapist asked: "Are
Patient Stories
Dancer Recovers From Hip Injury With Physical TherapyDec 14, 2015
After hip impingement led to surgery, Elizabeth said she felt like her "legs had been cut off." Her partnership with her physical therapist got her back
