Physical Therapy Guide to Osgood-Schlatter Disease
Osgood-Schlatter disease is an overuse injury found only in growing children. It is one of the most common causes of pain at the front of the knee and affects 1 in 10 children in the United States. OSD occurs most often in active eight- to 15-year-old children during periods of rapid growth. It usually can last anywhere from 12 to 24 months. OSD can cause the enlargement of the bony bump below the kneecap at the top of the shin. Repeated activities like walking up and down stairs, running, jumping, and landing can contribute to OSD. Children involved in regular or competitive sports are at a higher risk for developing the condition. OSD typically affects one knee, but the condition occurs in both knees about 20% to 40% of the time. OSD affects males and females equally. Physical therapists help children with OSD decrease pain, increase muscle strength, improve muscle flexibility, restore function and movement, and reduce risk of further injury.
Physical therapists are movement experts. They improve quality of life through hands-on care, patient education, and prescribed movement. You can contact a physical therapist directly for an evaluation. To find a physical therapist in your area, visit Find a PT.
What Is Osgood-Schlatter Disease?
Osgood-Schlatter disease is an overuse condition. It develops over time, rather than as a result of a single event. With OSD, irritation and swelling occur at the growth plate at the top of the shinbone. A growth plate is a layer of cartilage near the end of a bone where most of the bone's growth happens. Cartilage is a rubbery, flexible material that is not as strong as the bone, which puts it at more risk for injury from high levels of repeated stress.
Osgood-Schlatter disease happens during a young person’s growth spurts (8-15 years of age). During a growth spurt, the bones, muscles, and tendons grow at different rates. Participating in certain activities and sports can cause inflammation at the growth plate. This leads to the pain and swelling of the bump below the kneecap at the top of the shin.
OSD is more common in athletes who participate in sports that involve:
- Running (soccer, track).
- Sprinting (football).
- Jumping (basketball, volleyball).
- Cutting (changing directions of movement quickly, as in lacrosse or soccer).
- Landings (gymnastics, ballet).¬
- Walking or running up and down stairs.
OSD occurs during periods of rapid growth in:
- Males 12 to 15 years old.
- Females 8 to 12 years old.
It is important to address symptoms while they are happening. However, OSD only occurs during a child’s growth and typically goes away on its own when the ends of the bone harden, and the child stops growing. Treatment of OSD can help to limit or prevent future tendon problems (such as tendonitis, bone overgrowth, or fracture).
OSD is most often treated conservatively (without surgery) and focuses on:
- Symptom management (decreasing pain and inflammation).
- Decreasing the stress or pull at the thigh muscles and bump at the top of the shin.
- Addressing strength and movement issues.
- Guidance for variety in sports participation.
- Modifying activities within a specific sport.
How Does It Feel?
Symptoms of OSD can include:
- Dull ache or pain at just below the front of the knee near the bump on the top of the shin (medically known as the tibial tubercle) with:
- Contact or kneeling.
- Active knee bending or resisted knee straightening (like walking up/down stairs).
- Swelling and increased size of the bump at the top of the shin.
- Pain that worsens during or after activity.
- Pain that improves with rest or stopping the painful activity.
- Limping (may occur during or following activities).
- Weakness in the affected knee.
How Is It Diagnosed?
A pediatrician or physical therapist can diagnose OSD through a review of a child’s history and by conducting a physical exam. A physical therapist may be the first health care provider to evaluate and diagnose your child with OSD.
They may ask your child questions such as:
- Where do you feel the pain?
- When do you feel the pain?
- When did you first notice the pain and how long have you had the pain?
- What makes your pain better?
- What sports or activities do you participate in?
- How often and how long do you play or practice during the week?
- What position do you play?
Because all the joints in the lower half of the body work together to support your body, your physical therapist also may examine your child’s core, trunk, hips, and ankles.
A physical therapist exam to diagnose or rule out OSD can include assessment of:
- Joint range of motion.
- Muscle flexibility (particularly the hamstrings, quadriceps, and calves).
- Muscle strength (particularly the quadriceps and hip muscles).
- Tenderness to touch (knees).
- Swelling (by taking measurements of the bump at the top of the shin).
- Special tests on the knee (to rule out other diagnoses).
- Walking and running.
- Common functional movements (squats, stairs, jumping).
If your physical therapist suspects more than a stress-related irritation, they will likely refer you to an orthopedic doctor (a bone specialist). Symptoms like a recent significant loss of motion or strength, or severe pain with certain movements, may suggest the need for diagnostic imaging (such as ultrasound, X-ray, or MRI).
How Can a Physical Therapist Help?
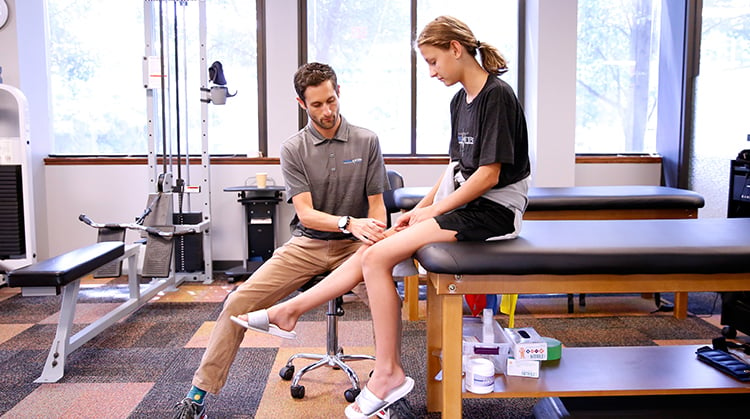
Once other conditions are ruled out and OSD is diagnosed, a child can expect the following steps in treatment to occur:
Your physical therapist will work with you to develop a personalized treatment plan. This plan will address your OSD symptoms and your goals.
Your physical therapist will work with you to manage your pain while enabling you to participate in activities without causing further damage.
Your physical therapy treatment plan may include:
Patient education. Your physical therapist will provide important information to help you manage your condition and avoid further injury. The first step to addressing your knee pain is to limit the amount of stress on the knee. Your physical therapist may recommend the following:
- When you should stop doing an activity that causes pain.
- What to do when you do feel the pain (rest, modify your activity level).
- How long you should rest and be without pain before restarting any activity that caused pain.
- How to modify the intensity of your activity or sport to allow for continued participation.
- Education on the importance of varying your sports and activity (cross training, or participating in a few different sports or activities, rather than specializing in only one).
Range-of-motion (flexibility). Your physical therapist will assess the motion of your knee and its surrounding joints and muscles. They will design gentle range of motion or stretching exercises to help you restore and maintain range of motion.
Strength training. Your physical therapist will teach you exercises to strengthen the muscles around your knee and any other areas of your lower body that may be weak. Strengthening these muscles will ease the stress on your knee joint and help protect it.
Manual therapy. Physical therapists are trained in manual (hands-on) therapy. If needed, your physical therapist will gently move your kneecap or tendon and the surrounding muscles to improve their motion, flexibility, and strength. These techniques can address areas that are difficult to treat on your own.
Pain management. Your physical therapist may recommend specific treatments for sore or swollen spots or tight muscles. They also may recommend the temporary use of a specific type of brace, strap, or taping (to relieve stress on the tendon) to aid in pain management.
Functional training. Physical therapists are experts in movement and training you to function at your best. Your physical therapist will assess your movements and teach you to adjust them to relieve any extra stress on the front of your knee.
Can This Injury or Condition Be Prevented?
There are several ways to help prevent OSD, including education for families (parents, caregivers, and youth athletes), coaches, and educators (physical education teachers).
If OSD symptoms appear, consult a physical therapist as soon as possible.
Early treatment can help to prevent the injury from getting worse and allows your child to continue participating in activities safely. Following the advice and training of a physical therapist helps prevent the injury from leading to more serious issues, including fracture or tendonitis.
Physical therapists have extensive knowledge and can:
- Educate on guidelines for participating in sports, school, and recreational-based activities.
- Explain the common cause of overuse injuries and provide strategies for prevention.
- Inform about the risks of playing through pain.
- Help athletes, their parents, and their coaches understand the benefits of scheduling time to do the assigned physical therapy exercises and to allow time to recover between activities or events.
- Track an adolescent’s growth curves (height, weight, body mass index) to help identify periods of increased risk for further injury.
- Develop customized flexibility and strengthening routines for children and youth athletes to follow throughout the sports season or school year.
What Kind of Physical Therapist Do I Need?
All physical therapists are prepared through education and clinical experience to treat a variety of conditions or injuries, including Osgood-Schlatter disease. You may want to consider:
- A physical therapist who is experienced in treating orthopedic or musculoskeletal injuries or who focuses on sports physical therapy.
- A physical therapist who has experience treating pediatric patients.
- A physical therapist who is a board-certified clinical specialist or has completed a residency in pediatric, orthopedic, or sports physical therapy. This physical therapist will have advanced knowledge, experience, and skills that apply to the active pediatric population.
You can find physical therapists with these and other credentials by using Find a PT, an online tool provided by the American Physical Therapy Association. This tool will help you search for physical therapists with specific clinical expertise in your geographic area.
General tips when you're looking for a physical therapist (or any other health care provider):
- Ask for recommendations from family, friends, or other health care providers.
- When you contact a physical therapy clinic for an appointment, ask about the physical therapists' experience in helping adolescents and young athletes with knee pain.
- Be prepared to describe your symptoms in as much detail as possible, and report activities that make the symptoms worse.
The American Physical Therapy Association believes that consumers should have access to information that could help them make health care decisions and also prepare them for a visit with their health care provider.
The following articles provide some of the best scientific evidence related to physical therapy treatment of Osgood-Schlatter disease and pediatric injuries. The articles report recent research and give an overview of the standards of practice, both in the United States and internationally. The article titles are linked either to a PubMed* abstract of the article or to free full text, so you can read it or print out a copy to bring with you to your health care provider.
Smith JM, Varacallo M. Osgood-Schlatter disease. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2023 Aug 4. Article Summary in PubMed.
Ladenhauf HN, Seitlinger G, Green DW. Osgood–Schlatter disease: a 2020 update of a common knee condition in children. Curr Opin Pediatr. 2020;32(1):107–112. Article Summary in PubMed.
Rathleff MS, Winiarski L, Krommes K, et al. Activity modification and knee strengthening for Osgood-Schlatter disease: a prospective cohort study. Orthop J Sports Med. 2020;8(4):2325967120911106. Article Summary in PubMed.
Rathleff MS, Winiarski L, Krommes K, et al. Pain, sports participation, and physical function in adolescents with patellofemoral pain and Osgood-Schlatter disease: a matched cross-sectional study. J Orthop Sports Phys Ther. 2020;50(3):149–157. Article Summary in PubMed.
Guldhammer C, Rathleff MS, Jensen HP, Holden S. Long-term prognosis and impact of Osgood-Schlatter disease 4 years after diagnosis: a retrospective study. Orthop J Sports Med. 2019;7(10):2325967119878136. Article Summary in PubMed.
Lam JJH, Venkatesh SH, Ho CL, Wong BSS. Clinics in diagnostic imaging (202). Osgood-Schlatter disease (OSD). Singapore Med J. 2019;60(12):610–615. Article Summary in PubMed.
Kienstra A, Macias CG. Osgood-Schlatter disease (tibial tuberosity avulsion). Summary on UpToDate. Published 2019.
Circi E, Atalay Y, Beyzadeoglu T. Treatment of Osgood-Schlatter disease: review of the literature. Musculoskelet Surg. 2017;101(3):195–200. Article Summary in PubMed.
*PubMed is a free online resource developed by the National Center for Biotechnology Information. PubMed contains millions of citations to biomedical literature, including citations in the National Library of Medicine’s MEDLINE database.
Expert Review:
Mar 16, 2024
Revised:
Jul 22, 2024
Content Type: Guide
Osgood-Schlatter Disease
PT, DPT, board-certified clinical specialist in sports physical therapy
Kara Copanas
PT, DPT, Board-Certified Clinical Specialist in Pediatric Physical Therapy, on behalf of the Academy of Pediatric Physical Therapy