Physical Therapy Guide to Fibularis Tendinopathy
Fibularis (or peroneal) tendinopathy, is an injury to the tendons on the outside of your lower leg. It can cause pain near the back and outside of your foot or heel. This injury often happens to long-distance runners or athletes who do quick movements or jump a lot. It is more common in basketball players and dancers. People with ankle sprains or weak ankles also are more likely to develop this injury. Physical therapists can help by reducing pain and improving ankle strength and motion.
Physical therapists are movement experts. They improve quality of life through hands-on care, patient education, and prescribed movement. You can see a physical therapist directly for evaluation and treatment without a physician’s referral.* To find a physical therapist in your area, visit Find a PT.
*A referral may still be required by your insurance plan (some states may limit the type or duration of treatment without a referral).
What Is Fibularis Tendinopathy?
A tendon is a strong, rope-like tissue that connects muscle to bone. The fibula is the long bone on the outer side of the lower leg. Tendinopathy is a general term for injuries that can cause pain, tenderness, stiffness, and weakness. There are two stages of tendinopathy:
- Inflammatory (tendinitis), an acute condition caused by inflammation of the tendon.
- Degenerative (tendinosis), a chronic condition where the tendon becomes stiff and thick.
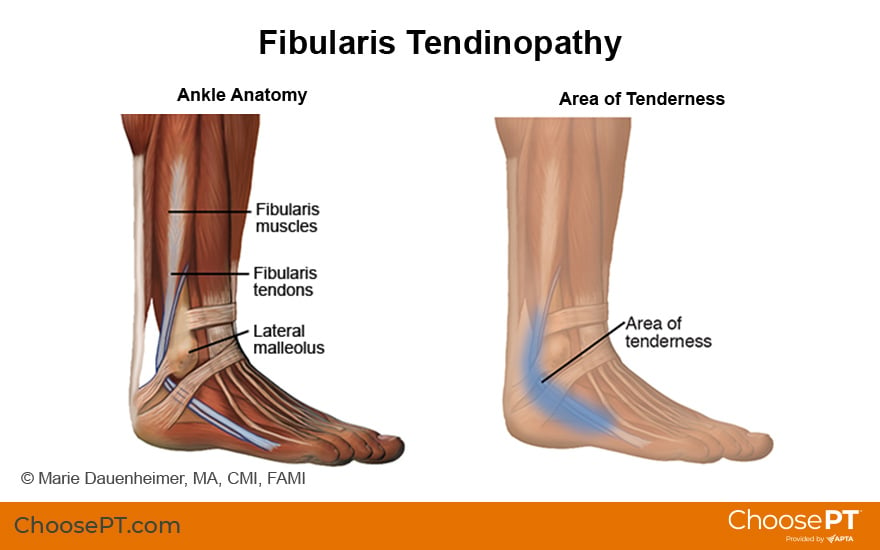
Fibularis tendinopathy is the updated term for peroneal tendinopathy, which some providers might use. This new term was adopted in 1999 to align with Latin-based medical language. The fibularis muscles begin on the outer shin bone called the fibula. The tendons of the fibularis brevis and fibularis longus muscles follow similar paths but attach to different parts of the foot. When the foot bears weight, these muscles are crucial for stability during walking and running. They also rotate the foot outward and assist in pointing the foot downward.
Causes of fibularis tendinopathies include:
- Doing too much activity without enough rest (overuse injury)
- Weak foot muscles causing the fibularis muscles to work harder to stabilize the foot (overuse injury)
- A low or high arch that can lead to increased stress on the tendons
- A lateral ankle sprain (when the ankle rolls inward) that strains the fibularis
- A partial dislocation of the fibularis tendons at the outer ankle bone (lateral malleolus)
- Improper footwear
How Does It Feel?
If you have fibularis tendinopathy, you might notice:
- Pain at the back of the foot or heel during or after activity, such as:
- Pushing up off the ball of the foot (a heel raise)
- Walking, running, or jogging
- Quick movements
- Jumping
- Walking on uneven surfaces or on a hill
- Decreased pain with rest but pain in the morning
- Swelling or tenderness behind the outer ankle bone (lateral malleolus)
- Soreness on the outside of the lower leg
- Pain and weakness when actively moving the foot outward
- A clicking or popping sensation when you move your foot
How Is It Diagnosed?
A physical therapist will diagnose your ankle injury with a thorough evaluation. They will ask about your health, daily activities, and how the injury happened.
A physical therapy evaluation for an ankle injury may include:
- Looking at how you walk, squat, and climb stairs
- Testing the strength of your foot, legs, and core (the muscles of your trunk)
- Measuring the range of motion of your foot, ankle, and other joints
- Assessing the flexibility of your legs
- Testing your balance and movement patterns
- Performing movement and resistance tests to determine what tissues are causing your symptoms
- Discussing your goals, including what activities you want to return to
Your physical therapist may refer you to an orthopedic doctor or podiatrist to rule out other causes with imaging tests. An X-ray can rule out an injury to the bone. An MRI or CT scan can show the health of muscles, tendons, and ligaments. After your diagnosis, your physical therapist will work with you to create a personalized treatment program to begin your recovery.
How Can a Physical Therapist Help?
Physical therapists are doctorate-educated movement experts. They help people with fibularis tendon injuries heal through custom treatment plans. Your physical therapist will design a program based on your evaluation results and personal goals.
Your treatment program may include:
Education. You will learn what caused your injury and how to modify your activities so your tendon can heal. You will also learn ways to prevent reinjury. As your symptoms improve, your physical therapist will guide you on how to gradually resume normal activities.
Hands-on therapy (manual therapy). Mobilizing your joints and soft tissue helps to reduce stiffness and improve movement. Your physical therapist may use these hands-on techniques to help the fibularis tendon heal.
Pain management. Your physical therapist will monitor your progress and pain levels throughout treatment. They may use ice and heat. Additional therapies they may provide to reduce pain include:
- Shock wave therapy (a treatment that uses high-energy sound waves)
- Low-level laser
- Ultrasound
- Iontophoresis (medication delivered through an electric patch)
- Dry needling to help with healing and pain relief.
Footwear and orthotics. Your physical therapist may recommend shoes or inserts to support your foot while it heals. In some cases, they may suggest custom orthotics or shoe inserts. As you get stronger, your footwear needs may change. You may start with inserts and then not need them as your condition resolves. However, in some cases, long-term footwear adjustments could be advised.
Range-of-motion exercises. Tightness in your foot, ankle, or legs can lead to fibularis tendinopathies. Your physical therapist will use hands-on techniques and exercises to restore normal movement.
Strengthening exercises. Targeted resistance exercises promote tendon healing. Building strength in your foot, hip, and core also helps protect your feet and ankles from stress. Your physical therapist will guide you through a gradual strengthening program to help you return to the activities you enjoy.
Functional training. Task-specific exercises can help get you ready to return to your activities. When recovering from a tendon injury, there may be ups and downs in your progress. Sometimes, swelling or inflammation can happen because your body is responding to new stress. This is normal as your tendon adjusts and gets stronger. Your physical therapist will monitor your response to exercises and adjust your program as needed to support steady healing.
Can This Injury or Condition Be Prevented?
Fibularis tendinopathy can often be prevented. These tips can reduce your risk for fibularis tendinopathy:
- Pay attention to pain. If you feel pain on the outside of your foot or ankle after sports, apply ice and allow yourself time to recover. Rest days, along with massaging the area and gentle stretching can help.
- Make changes gradually. Make sure to slowly increase how hard you train, how long you exercise, and the kinds of exercises you do. This helps prevent injuries caused by overuse or doing too much too soon.
- Add strength training. Include exercises for your core, hips, legs, and feet in your regular exercise regimen to improve stability and reduce stress on your ankles.
- Get a gait assessment. A physical therapist can assess your walking or running style and recommend the right shoes or inserts for your needs.
The American Physical Therapy Association encourages regular physical therapy checkups to detect early signs of muscle imbalances, joint stiffness, poor movement habits, or restricted movement. Addressing these issues may help prevent muscle and joint injuries that can develop over time. Physical therapists can design a personalized program tailored to your specific needs and goals to enhance your physical health and lower your risk of injury.
What Kind of Physical Therapist Do I Need?
All physical therapists are prepared through education and experience to treat fibularis tendinopathy. However, you may want to consider:
- A physical therapist who is experienced in treating people with ankle tendinopathies.
- A physical therapist whose practice focuses on orthopedic or sports rehabilitation.
- A physical therapist who is a board-certified clinical specialist or has completed a residency or fellowship in orthopedic or sports physical therapy. This physical therapist has advanced knowledge, experience, and skills that may apply to your condition.
You can search for physical therapists who have these and other credentials by using Find a PT, an online tool provided by the American Physical Therapy Association.
General tips when you're looking for a physical therapist (or any other health care provider) include:
- Get recommendations from family, friends, or other health care providers.
- Ask about the physical therapists' experience in helping people with ankle tendinopathies.
- Be prepared to describe your symptoms in as much detail as possible, and say what makes your symptoms better or worse.
The American Physical Therapy Association believes consumers should have access to information that can help them make informed healthcare decisions and prepare for their visit with their health care provider.
The following resources provide some of the best scientific evidence related to physical therapy treatment of fibularis tendinitis. They report recent research and give an overview of the standards of practice both in the United States and internationally. The article titles are linked either to a PubMed* abstract of the article or to free full text, so that you can read it or bring it to discuss with your health care provider.
Melville DM, Taljanovic MS, Gimber LH, et al. Comparison of ultrasound and MRI with intraoperative findings in the diagnosis of peroneal tendinopathy, tears, and subluxation. J Clin Med. 2024;13(3):740. Article Summary in Pubmed.
Sprinchorn AE, Eizenberg N, Barker PJ. Differences and similarities in muscle architecture of fibularis longus and brevis: an observational descriptive cross-sectional and feasibility study. J Orthop Surg Res. 2024;19(1):105. Article Summary in Pubmed.
Sasun AR, Babar T, Dadgal R. Effectiveness of ankle proprioceptive neuromuscular facilitation techniques in restoring the biomechanical integrity of the ankle following plantar fasciitis: an experimental study. Cureus. 2024;16(7):e64371. Article Summary in Pubmed.
Hayek R, Gottlieb U, Gutman I, et al. Peroneal muscle response to single-leg drop-jump and unexpected leg-drop in young and middle-aged adults before and after one session of neuromuscular training. Eur Rev Aging Phys Act. 2023;20(1):11. Article Summary in Pubmed.
Yoshizuka H, Kuraoka A. Calcaneofibular ligament may act as a tensioner of peroneal tendons as revealed by a contactless three-dimensional scan system on cadavers. Sci Rep. 2022;12(1):16650. Article Summary in Pubmed.
Willegger M, Hirtler L, Schwarz GM, et al. Peroneal tendon pathologies: from the diagnosis to treatment. Orthopade. 2021;50(7):589–604. Article Summary in Pubmed.
Ugbolue UC, Yates EL, Ferguson K, et al. Electromyographic assessment of the lower leg muscles during concentric and eccentric phases of standing heel raise. Healthcare (Basel). 2021;9(4):465. Article Summary in Pubmed.
Koldenhoven RM, Fraser JJ, Saliba SA, et al. Ultrasonography of gluteal and fibularis muscles during exercises in individuals with a history of lateral ankle sprain. J Athl Train. 2019;54(12):1287–1295. Article Summary in Pubmed.
Bavdek R, Zdolsak A, Strojnik V, Dolenec A. Peroneal muscle activity during different types of walking. J Foot Ankle Res. 2018;11:50. Article Summary in PubMed.
Scott A, Docking S, Vicenzino B, et al. Sports and exercise-related tendinopathies: a review of selected topical issues by participants of the second international scientific tendinopathy symposium (ISTS) Vancouver 2012. Br J Sports Med. 2013;47(9):536–544. Article Summary in PubMed.
Rao S, Riskowski J, Hannan MT. Musculoskeletal conditions of the foot and ankle: assessments and treatment options. Best Pract Res Clin Rheumatol. 2012;26(3):345–368. Article Summary in PubMed.
Hensley CP, Kavchak AJ. Novel use of a manual therapy technique and management of a patient with peroneal tendinopathy: a case report. Man Ther. 2012;17(1):84–88. Article Summary in PubMed.
*PubMed is a free online resource developed by the National Center for Biotechnology Information. PubMed contains millions of citations to biomedical literature, including citations in the National Library of Medicine’s MEDLINE database.
Expert Review:
Nov 21, 2025
Revised:
Mar 23, 2026
Content Type: Guide
Peroneal Tendinopathy
PT, MPT
Makenzie Mazin
PT, DScPT