Physical Therapy Guide to Shoulder Replacement (Arthroplasty)
Shoulder replacement (arthroplasty) is surgery to replace all or part of the shoulder joint. Although less common than a knee or hip replacement, around 65,000 people have shoulder arthroplasties in the U.S. each year. Physical therapists help people return to their prior activity levels after total or partial shoulder replacement surgery.
Physical therapists are movement experts. They improve quality of life through hands-on care, patient education, and prescribed movement. You can contact a physical therapist directly for an evaluation. To find a physical therapist in your area, visit Find a PT.
What Is Shoulder Arthroplasty?
Shoulder replacement (arthroplasty) is a surgical procedure done when other treatments, such as medication or physical therapy, have not managed or helped with pain, or the shoulder cannot be used. A visit with an orthopedic surgeon will help you decide whether to have this surgery.
The conditions that lead to shoulder replacement surgery most often include:
- Osteoarthritis of the shoulder.
- Rotator cuff disease (a muscle tear or breakdown of the rotator cuff muscles).
- Shoulder fracture.
Less common reasons for surgery include:
- Rheumatoid arthritis.
- Osteonecrosis -- a rare condition in which the head of the arm bone dies.
There are three different types of shoulder arthroplasties. Your orthopedic surgeon will consider various factors. Your surgeon will decide whether or not one of these procedures is right for you:
Total shoulder arthroplasty. This surgery involves removing the ends of two bones at the shoulder and replacing them with artificial parts. The upper part of the arm bone is shaped like a ball. This is called the "head" of the shoulder. The head sits on a small socket in the shoulder blade to make the shoulder joint. During a TSA, the head is replaced by a ball-shaped metal implant. A small dish-like cup replaces the socket.
Shoulder hemiarthroplasty. This is a partial shoulder replacement. In this surgery, only the head of the arm bone is replaced with a metal ball.
Reverse total shoulder arthroplasty. In this procedure, the surgeon will reverse the ball and socket. Doctors recommend this surgery when there is damage to the rotator cuff muscles of the shoulder. The plastic device is attached to the top of the arm bone and the metal ball is attached to the socket. This allows the deltoid, another shoulder muscle, to provide movement. The deltoid compensates for the damaged rotator cuff muscles. This surgery can improve the range of motion, strength, and stability of your shoulder.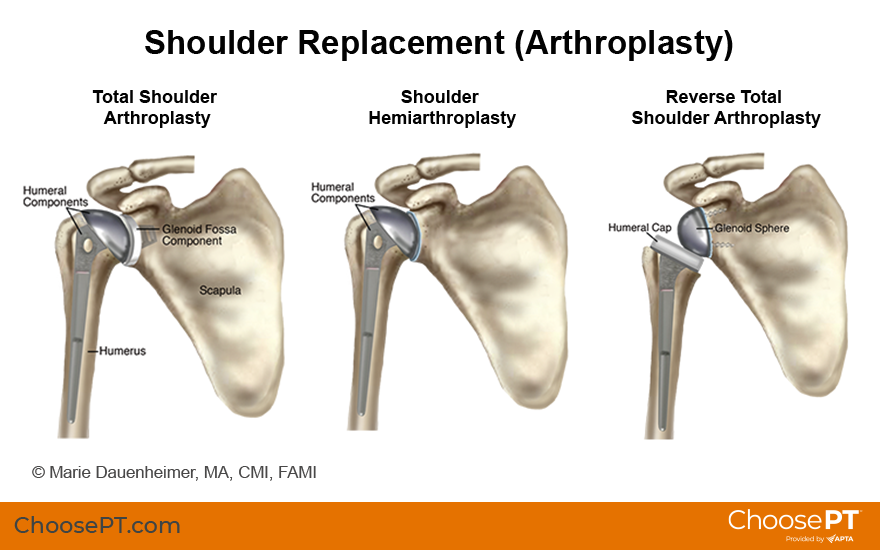
How Can a Physical Therapist Help?
Physical therapy is vital for safe and healthy recovery after shoulder replacement surgery. After surgery, your physical therapist will guide you to improve your shoulder function and limit pain while you heal. As you regain strength and movement, your PT will help you safely return to your previous activity levels. The goal is to restore your ability to do household activities, job duties, and recreational hobbies.
Your PT also can work with you before surgery to help prepare your shoulder for surgery.
How Can a Physical Therapist Help Before & After Surgery?
Before Surgery
If possible, it is best to work with a physical therapist prior to surgery. The better physical condition your shoulder is in before surgery, the better you will recover. Your physical therapist will create a customized program for you. This may include strengthening of the shoulder, neck, and back muscles. Stretches and posture training may be a part of your presurgery program too.
If you take prescribed opioid medications, talk to your surgeon about weaning off them before your surgery. And ask your physical therapist how they can help you manage pain prior to surgery. Patients who use opioid medications for pain relief before surgery have been shown to have worse outcomes compared with those who do not.
After Surgery
After your surgery, you will likely stay in the hospital for two to three days. Your stay could be longer if you have other medical conditions, such as diabetes or heart disease. Your shoulder will be in a sling for three to eight weeks, depending on your surgeon's directions. While wearing the sling, you will be told not to move your shoulder. Your physical therapist will teach you more do’s and don’ts to help speed your recovery.
Physical therapy will begin a day or two after your surgery. A hospital physical therapist will teach you how to perform specific exercises and simple tasks. You also will be told about certain movements to avoid. Your PT may teach you how to:
- Get in and out of bed safely.
- Take your sling off and put it on properly.
- Get dressed while keeping your shoulder in a safe position.
Be sure to ask them any questions that you have about what to do and what not to do once you return home. These questions may include how to manage pain after surgery and swelling with ice treatments.
Your physical therapist also will teach you gentle exercises to help you heal and reduce stiffness. You may need help from friends or family with daily activities for the first few days or weeks. You will not be able to drive for a few weeks after surgery. To help with healing, avoid smoking and alcohol after surgery. If you have diabetes or glucose intolerance, work with your doctor to manage your condition after surgery.
As You Recover
When you are discharged from the hospital, continuing your physical therapy is essential. Your surgeon and your physical therapist will work with you as a team to ensure your safe recovery. Be sure to talk with your physical therapist to find the best balance of exercise and rest. Different exercises are prescribed at specific points after surgery. Your physical therapist will teach you the ones that are best for you at each stage of your recovery. Your treatment plan may include:
Range-of-motion exercises. It is critical to not move your shoulder suddenly or with any force for the first two to six weeks after surgery. Your physical therapist will assist you with gentle movements in different directions to aid healing. These may be passive movements, which your physical therapist will perform for you, or active movements you do yourself. Your physical therapist also will teach you gentle exercises to perform at home. And you may learn range-of-motion exercises for the elbow and hand to avoid stiffness while wearing the sling.
Strengthening exercises. Initially, you can squeeze a ball or putty to help keep your grip strong while in the sling. As your mobility returns within a few weeks or months, your physical therapist will guide you through a shoulder strengthening program. When the time is right, your physical therapist may have you use resistance bands and weights to perform gentle strength-building exercises.
Functional training. Your physical therapist will help you regain everyday shoulder movements. They will teach you how to safely perform activities that are important to you for your self-care. Be sure to tell your physical therapist the areas of your life that are important to you. They will design your treatment program for your specific needs.
Job and sport-specific training. As your strength and movement increases, your physical therapist will design a custom program to help get you back to your job tasks. These may include reaching, pushing, or carrying motions. You also may receive sport-specific training if you are planning to return to a sport. Your physical therapist will create a home or fitness-center exercise program based on your personal needs.
Can This Injury or Condition Be Prevented?
Shoulder replacement is typically an elective surgery. If you notice that your shoulder is painful and you lose the ability to use it, a physical therapist can help. A properly designed exercise program may help you delay or even avoid surgery. A physical therapist can teach you how to manage your pain and restore movement. Your unique treatment plan could focus on your posture, or on learning safe exercises for strength and flexibility. A stable and healthy shoulder joint requires regular activity and frequent exercises for strength. Your physical therapist will design an individual exercise program to address your specific needs and goals.
Proper nutrition and physical activity will keep all of your joints healthy! Avoid smoking or nicotine products. These are associated with inflammation and may limit your recovery from any injury.
What Kind of Physical Therapist Do I Need?
All licensed physical therapists are prepared through education and experience to treat people before and after shoulder surgery. Consider finding a physical therapist who has experience treating individuals with musculoskeletal conditions. You may want to look for a specialized physical therapy clinic focused on orthopaedic conditions or sports medicine. You may choose to ask for a highly qualified physical therapist with postprofessional special training, such as one of these:
- A physical therapist who has completed a residency program and who has spent 1,500 hours to advance their knowledge and skills within a specific specialty area.
- A board-certified clinical specialist with advanced clinical knowledge, experience, and skills in geriatric, orthopaedic, or sports physical therapy.
- A physical therapist who has completed a fellowship program and has met specific criteria. These physical therapists have advanced knowledge and expertise in their specific area. You may want to look for a geriatrics, orthopaedic, or sports physical therapy fellow.
You can find a physical therapist who has these and other credentials by using Find a PT. This is an online tool built by the American Physical Therapy Association to help you search for physical therapists with specific clinical expertise in your geographic area.
General tips when you're looking for a physical therapist or any other health care provider:
- Get recommendations from family, friends, or other health care providers.
- When you contact a physical therapy clinic for an appointment, ask about the physical therapist’s experience in helping people who have shoulder or orthopedic conditions.
Additional Resources
The American Physical Therapy Association (APTA) believes that consumers should have access to information that could help them make health care decisions, and also prepare them for a visit with their health care provider.
The following articles provide some of the best scientific evidence related to shoulder surgery. The articles report recent research and give an overview of the standards of practice both in the U.S. and internationally. The article titles are linked either to a PubMed* abstract of the article or to free full text, so that you can read it or print out a copy to bring with you to your health care provider.
Bullock GS, Garrigue GE, Ledbetter LA, Kennedy J. A systematic review of proposed rehabilitation guidelines following anatomic and reverse shoulder arthroplasty. J Orthop Sports Phys Ther. 2019;49(5):337–346. Article Summary in PubMed.
Cox RM, Brolin TJ, Padegimas EM, et al. Outcomes of bilateral shoulder arthroplasties: a comparison of bilateral total shoulder arthroplasties and bilateral reverse shoulder arthroplasties. Clin Orthop Surg. 2019;11(3):316–324. Article Summary in PubMed.
Goplen CM, Verbeek W, Kang SH, et al. Preoperative opioid use is associated with worse patient outcomes after total joint arthroplasty: a systematic review and meta-analysis. BMC Musculoskelet Disord. 2019;20(1):234. Article Summary in PubMed.
Leroux TS, Zuke WA, Saltzman BM, et al. Safety and patient satisfaction of outpatient shoulder arthroplasty. JSES Open Access. 2018;2(1):13–17. Article Summary in PubMed.
Liu JN, Steinhaus ME, Garcia GH, et al. Return to sport after shoulder arthroplasty: a systematic review and meta-analysis. Knee Surg Sports Traumatol Arthrosc. 2018;26(1):100–112. Article Summary in PubMed.
Rasmussen JV, Hole R, Metlie T, et al. Anatomical total shoulder arthroplasty used for glenohumeral osteoarthritis has higher survival rates than hemiarthroplasty: a Nordic registry-based study. Osteoarthritis Cartilage. 2018;26(5):659–665. Article Summary in PubMed.
Wagner ER, Solberg MJ, Higgins LD. The utilization of formal physical therapy after shoulder arthroplasty. J Orthop Sports Phys Ther. 2018;48(11):856–863. Article Summary in PubMed.
Dillon MT, Chan PH, Inacio MC, Singh A, Yian EH, Navarro RA. Yearly trends in elective shoulder arthroplasty, 2005-2013. Arthritis Care Res (Hoboken). 2017;69(10):1574–1581. Article Summary in PubMed.
Schairer WW, Nwachukwu BU, Lyman S, Craig EV, Gulotta LV. National utilization of reverse total shoulder arthroplasty in the United States. J Shoulder Elbow Surg. 2015;24(1):91–97. Article Summary in PubMed.
*PubMed is a free online resource developed by the National Center for Biotechnology Information (NCBI). PubMed contains millions of citations to biomedical literature, including citations in the National Library of Medicine’s MEDLINE database.
Authored by Julie A. Mulcahy, PT, MPT. Revised and reviewed by Christina S. Crawford, PT, DPT, MSHS, advanced credentialed exercise expert for aging adults and board-certified clinical specialist in geriatric physical therapy.
Revised:
Feb 5, 2020
Content Type: Guide
Shoulder Replacement