Physical Therapy Guide to Bunionette (Tailor's Bunion)
A bunionette, also known as a tailor’s bunion, is a small bump that forms on the side of the foot at the base of the pinky toe. It may or may not cause pain. The term tailor’s bunion comes from a time when tailors often sat cross-legged, with the outer edge of their foot pressed against the ground. This repeated pressure was thought to contribute to the development of the bump.
Bunionettes are more common in women than in men and can occur on one or both feet. In many cases, they develop due to changes in foot alignment, which can place extra pressure on the outside of the foot.
A physical therapist can play an important role in helping prevent a bunionette from worsening. They can assess how the foot moves and functions. They also teach exercises to strengthen foot muscles, improve mobility, and reduce stress and pain in the affected area.
Physical therapists are movement experts. They improve quality of life through hands-on care, patient education, and prescribed movement. You can see a physical therapist directly for evaluation and treatment without a physician’s referral.* To find a local physical therapist, visit Find a PT.
*A referral may still be required by your insurance plan (some states may limit the type or duration of treatment without a referral).
What Is a Bunionette?
A bunionette is a bump that develops on the base of the pinky toe on the outer side of the foot. It may be caused by tight-fitting shoes, especially those that are narrow in the forefoot or toe box. Or they may develop because of changes in foot alignment.
The long bones of the foot are the metatarsals. The small bones of the toes are the phalanges. In some people with a bunionette, the fifth metatarsal (the long bone behind the pinky toe) begins to drift away from the fourth metatarsal. At the same time, the pinky toe may shift inward toward the fourth toe. This change in alignment alters the shape of the foot and how the foot distributes pressure.
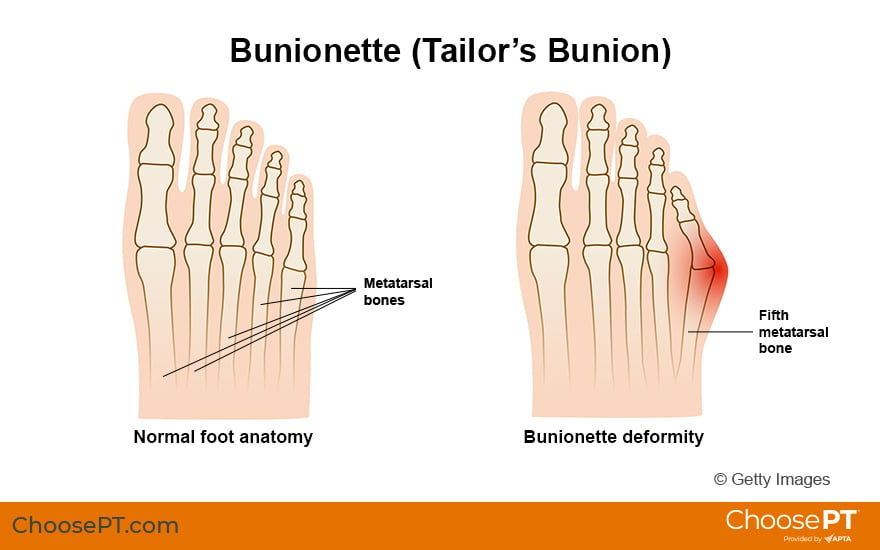
The foot tripod is a concept used to explain the complex mechanics by which the foot supports our bodies. It refers to three contact points: the base of the big toe, the base of the pinky toe, and the center of the heel. These points all work together to distribute pressure and provide stability.
With a bunionette, changes in foot alignment can shift how these points bear weight and interact with one another. This may increase pressure along the outer edge of the foot, making standing or walking less comfortable. When barefoot or wearing shoes with limited cushioning or support, discomfort may be greater. Another common issue is increased friction at the base of the pinky toe. This area may rub against footwear or experience added stress during movement. Over time, repeated pressure and friction can lead to irritation, pain, and inflammation.
A bunionette may develop for several reasons, including:
Inherited foot structure. Some people are born with foot shapes or have medical conditions that make a bunionette more likely to develop. These include:
- Splayfoot, where the long bones of the foot are naturally spread farther apart.
- Loose ligaments (hypermobility) that allow bones to shift over time.
- A high-arched foot. People with high arches often have stiffer feet that may not allow the normal amount of inward rolling (pronation) during walking. This can keep pressure on the outside of the bottom of the foot for longer than normal. It can also reduce the foot’s natural ability to absorb shock, increasing stress near the pinky toe.
- Over-pronation. Excessive inward rolling of the foot during walking or running can increase stress on the outside of the foot and the pinky toe.
- Bone structure differences. A larger‑than‑average head of the fifth metatarsal can make the area more prone to pressure and irritation.
- Chronic medical conditions. Medical conditions, such as rheumatoid arthritis, psoriatic arthritis, and osteoarthritis, may increase the risk of developing a bunionette. Inflammatory conditions like rheumatoid and psoriatic arthritis can damage joints over time, while osteoarthritis may lead to stress in the foot. When these conditions are combined with differences in foot structure or movement patterns, they can lead to changes in joint alignment, greater pressure on the pinky toe, and inflammation.
The tissue changes that may lead to pain or discomfort with a bunionette include:
- Skin and soft tissue inflammation and swelling at the base of the pinky
- Bursitis, or inflammation of the small fluid-filled sac that helps reduce friction (bursa)
- Callus formation due to long-term pressure or inflammation
- Inflammation or arthritis in the joint where the long bone meets the toe
- In more severe cases, a nerve can become irritated or inflamed
How Does It Feel?
Some people can see a bunionette without having any symptoms. Others may experience:
- Pain or pressure along the outside of the pinky toe
- Pain or pressure under the pinky toe
- Soreness that improves when wearing a shoe with a wide toe box
- Swelling, redness, or callus formation at the base of the pinky toe
The first line of treatment for a bunionette is often a change in footwear. Shoes with a wider toe box can reduce pressure on the pinky toe, while supportive shoes may help improve how your foot moves while walking. If these changes or over-the-counter inserts do not relieve your symptoms, custom orthotics may be recommended to provide additional support. Padding placed over the bunionette area may also help reduce irritation. To reduce pain and inflammation, a medical provider may recommend strategies such as ice, anti‑inflammatory medications, or, in some cases, injections.
A physical therapist can help identify movement or alignment factors that contribute to a bunionette, such as excessive inward rolling of the foot (over‑pronation). Physical therapy focuses on improving foot strength, flexibility, and mobility to reduce stress on the pinky toe, ease discomfort, and help prevent worsening of symptoms.
How Is It Diagnosed?
You may be the first to notice a change in the shape of your foot. Many people do not seek care for a bunionette until it begins to cause pain, irritation, or makes walking or wearing shoes difficult.
To diagnose a bunionette, a health care provider will first rule out other possible causes of pain on the outside of the foot, such as arthritis or soft‑tissue inflammation.
If you see a physical therapist first, they will perform a physical examination to assess foot alignment, joint mobility, muscle strength, and areas of stress or pressure. Your physical therapist may also observe how you stand and walk.
To confirm the diagnosis, a physical therapist may refer you to another health care provider, such as a foot and ankle orthopedic physician or podiatrist, for additional testing. Imaging, such as an X‑ray, may be used to determine whether changes in the alignment of the fifth toe or fifth metatarsal are contributing to your symptoms.
How Can a Physical Therapist Help?
If you have a bunionette, a physical therapist can help identify and address factors that may be placing extra pressure on your pinky toe and contributing to your symptoms. Your physical therapist will conduct a thorough evaluation, review your medical history and main concerns, and assess how your movement and mobility may be affecting your feet.
During your evaluation, a physical therapist may:
- Assess the mobility of your ankle, foot, and toes
- Observe how you walk barefoot and in your everyday shoes
- Assess the strength of muscles that support walking and balance, including the muscles of your foot, calf, hips, and core (trunk)
- Review your footwear choices and how they may impact foot alignment and pressure
- Test your balance and coordination
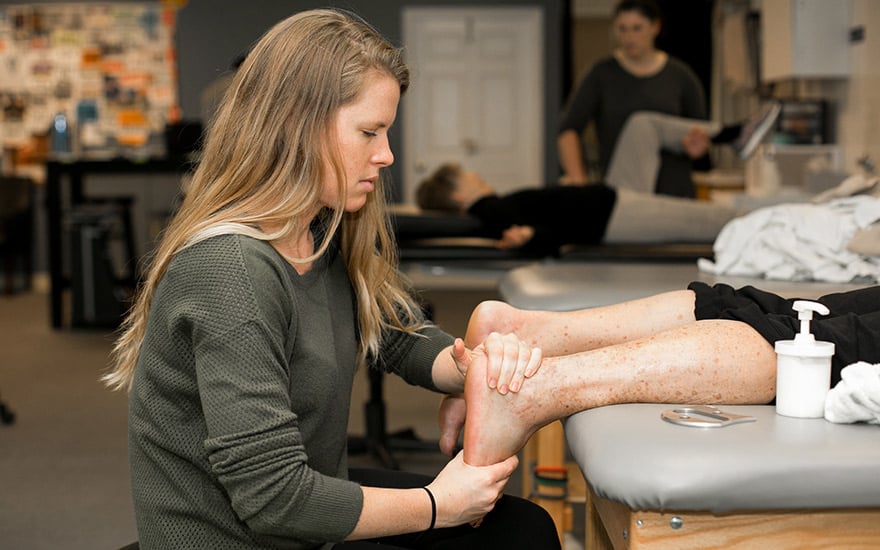
Based on this evaluation, your physical therapist will create a treatment plan designed to reduce pain, improve function, and help prevent the bunionette from worsening. Your treatment plan may include:
Patient Education. Your physical therapist can provide guidance on selecting footwear that reduces pressure on the pinky toe and supports healthy walking mechanics. In some cases, they may recommend or provide custom orthotics to support your foot.
Hands-on (Manual) Therapy. Your physical therapist may use hands-on techniques and guide you through flexibility exercises to improve joint mobility and foot movement.
Strengthening Exercises. Your physical therapist will design a program that includes strengthening exercises to help stabilize the foot during walking and daily activity. These will include exercises for the small muscles inside the foot (intrinsic foot muscles) and supporting muscles of the calf (extrinsic foot muscles), legs, and core.
Pain Management. Pain-relief strategies, such as the when to use ice or heat to manage your symptoms and improve comfort.
Working with a physical therapist can help you move more comfortably, stay active, and protect your foot health over time.
Can This Injury or Condition Be Prevented?
A bunionette caused by inherited foot structure or certain health conditions, such as rheumatoid arthritis, may be hard to prevent. However, many of the factors that lead to irritation, pain, or worsening of a bunionette can be managed.
Wearing tight or narrow shoes, especially those that crowd the toes, can put pressure on the toes and increase the risk of foot pain. While it is okay to occasionally wear fashionable shoes that put extra stress on the forefoot (such as high heels with or without a pointed toe), most of your time should be spent in shoes that allow your toes to move freely.
For people with high arches, which may be due to their natural foot structure or tightness in their joints or muscles. Wearing shoes with good cushioning and using exercise to improve foot and ankle motion can help reduce stress on the outside of the foot.
If you have been told that you overpronate (your foot rolls inward more than usual), wearing shoes that support normal foot motion or limit excessive pronation may reduce stress on your foot. A physical therapist can help you determine which types of shoes may work best for you, especially as you work to improve your foot strength.
Strengthening the small muscles inside your foot, known as the intrinsic foot muscles, can also help with prevention. One common exercise for this is often called toe Yoga. To perform this exercise, keep your heel and midfoot on the ground while lifting your big toe and keeping your smaller toes down. Hold for 1–2 seconds and repeat 10 times. Then switch by lifting your smaller toes while keeping your big toe down. This exercise can be challenging at first, and it’s okay to use your hands to assist as you learn the movement. You can do toe Yoga multiple times a day to build better control of your toes. This can help to support foot stability and how your foot interacts with the ground.
Strength in the rest of the leg and core can also help reduce stress on the foot during daily activities. Maintaining flexibility in the calf and foot muscles allows for easier movement when standing and walking. A physical therapist can design a personalized program to help you care for your feet and support long‑term foot health.
What Kind of Physical Therapist Do I Need?
All physical therapists are prepared through education and experience to treat people with bunions or bunionettes. However, you may want to consider:
- A physical therapist with experience treating foot, ankle, and orthopedic conditions. Some physical therapists focus on this area of care.
- A physical therapist who is a board-certified clinical specialist or who completed a residency or fellowship in orthopedic physical therapy. This therapist has advanced knowledge, experience, and skills that may apply to your condition.
You can find physical therapists who have these and other credentials by using Find a PT, an online tool built by the American Physical Therapy Association. Search for physical therapists by location and expertise.
General tips when you're looking for a physical therapist (or any other health care provider):
- Ask family, friends, and other health care providers to recommend a physical therapist.
- Ask about the physical therapists' experience in helping people who have bunions before you make an appointment.
- Be prepared to describe your symptoms in as much detail as possible, and say what makes them worse.
Davis DD, Taqi M, Kane SM. Fifth-Toe Deformities. [Updated 2022 Nov 19]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Article Summary in PubMed.
Wei Z, Zeng Z, Liu M, Wang L. Effect of intrinsic foot muscles training on foot function and dynamic postural balance: A systematic review and meta-analysis. PLoS One. 2022;17(4):e0266525. Published 2022 Apr 20. Article Summary in PubMed.
Cooper, M.T, Granadillw, V., and Coughlin, M. J. The bunionette deformity: Evaluation and management. Annals of Joint. Jan., 2020. Vol 5. Accessed on May, 11, 2026
Ceccarini P, Rinonapoli G, Nardi A, Bisaccia M, Di Giacomo LM, Caraffa A. Bunionette. Foot Ankle Spec. 2017;10(2):157-161. Article Summary in PubMed.
*PubMed is a free public website run by the National Library of Medicine. It allows people to access summaries and references from health research articles published in scientific journals, including those indexed in the MEDLINE database.
Expert Review:
May 13, 2026
Revised:
May 14, 2026
Content Type: Guide
Bunionette
PT, DScPT
Makenzie Mazin
PT, DScPT