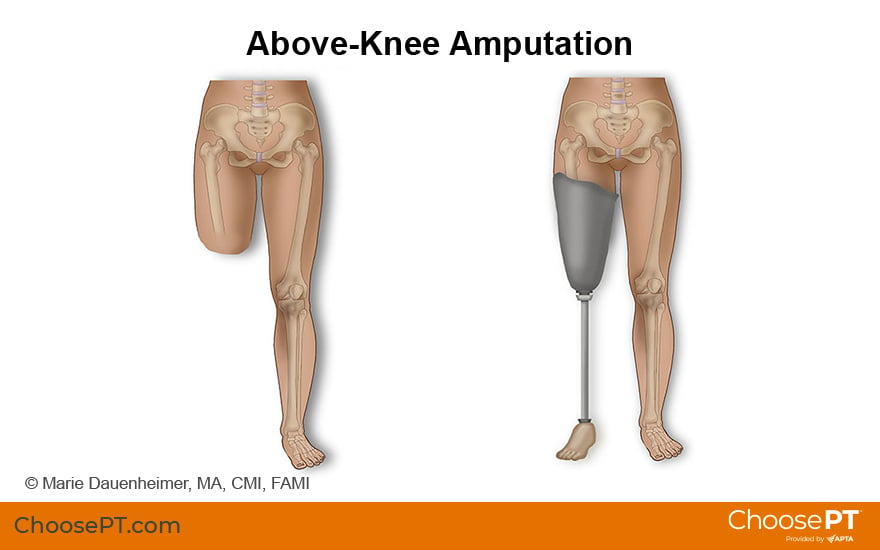
Physical Therapy Guide to Above-Knee Amputation (Transfemoral Amputation)
Above-knee amputation is the surgical removal of part of the leg above the knee. The procedure is also called transfemoral amputation, which refers to the femur, the large bone in the upper leg. Above-knee amputation may be performed on people of any age group. It is most common in those aged 65 and older. Major causes leading to this type of surgery are damage to the lower leg by trauma, infection, or disease.
Physical therapists are experts in human anatomy and movement. They help people increase mobility, manage pain, and improve quality of life through hands-on care, patient education, and prescribed movement. You can contact a physical therapist directly for an evaluation. To find a physical therapist in your area, visit Find a PT.
What Is Above-Knee Amputation?
The majority (70%–85%) of above-knee amputations are due to peripheral vascular disease, also known as peripheral arterial disease. PVD (or PAD) is a condition where blood vessels outside the heart become narrowed or blocked, leading to poor circulation. Reduced blood flow can damage the muscles, nerves, and skin. This can result in wounds that are difficult to heal, and infection.<.p>
When wounds worsen, infection can spread to the bone and become life-threatening. Amputation removes the diseased part of the limb and prevents the spread of infection. Surgeons perform above-knee amputation instead of below-knee amputation when:
- There is no longer enough blood flow in the entire lower leg.
- Infection is so severe it prohibits a lower-level amputation.
Above-knee amputation also may be needed after a catastrophic injury (trauma) or when a cancerous tumor damages the leg beyond repair.
A vascular or orthopedic surgeon typically performs the procedure. The goal is always to leave as much of the healthy limb as possible. The surgeon will also shape the remaining part of the limb (stump) to prepare for the use of a prosthesis.
How Can a Physical Therapist Help?
Your physical therapist can help you prepare for above-knee amputation surgery. They also can help you regain strength, movement, and function after surgery.
Prior to Surgery
Before your surgery, your physical therapist may:
- Prescribe exercises for conditioning and to improve the strength and flexibility of your hip and trunk.
- Teach you how to walk with a walker or crutches.
- Explain to you and your caregivers what to expect after the procedure.
Immediately After Surgery
Your hospital stay after amputation surgery will be about five to 14 days. Your wound will be bandaged. You also may have a drain (tube that is inserted into the area to help remove excess fluid). Your physician will help you manage your pain with proper medication.
Physical therapy will begin soon after surgery once your physician clears you for it. A physical therapist will review your medical and surgical history and visit you at your bedside. Your first two to three days of treatment may include:
- Learning to roll in bed, sit on the edge of the bed, and move safely to a chair.
- Gentle stretching and range-of-motion exercises.
- Learning how to position your limb to prevent muscle tightness and keep your ability to straighten the hip joint fully.
When you are medically stable, the physical therapist will help you learn to move about safely. They will work with you to help you prevent falls, use a wheelchair, and stand or walk with an assistive device.
Rehabilitation
Prevention of contractures. A contracture is the development of soft-tissue tightness that limits joint motion. The condition occurs when muscles and other soft tissues become stiff from lack of movement. The most common contracture following an above-knee amputation occurs at the hip. If the hip stays flexed (bent), you may be unable to straighten it. Sitting in the same position for long periods can contribute to contractures. Using a pillow under the thigh of the affected limb can also do so.
It is essential to prevent contractures early. They can become permanent if not addressed throughout the rehab process. Contractures can make it hard to wear your prosthesis. They also can make it difficult to walk.
Your physical therapist will help you maintain normal posture and range of motion at your hip. They will teach you how to position your leg and show you stretching exercises to maintain a normal range of motion. Following your physical therapist’s advice can help prevent a contracture.
Compression to address swelling. It is normal to swell after surgery. Your physical therapist will help you maintain compression on your limb. This will help to protect it, reduce and control swelling, and help it heal. Your physical therapist may:
- Wrap the limb with elastic bandages.
- Apply and have you wear an elastic shrinker sock.
These methods also help shape the limb to prepare it for fitting the prosthetic leg.
In some cases, a rigid dressing, or plaster cast, may be used instead of elastic bandages. An immediate post-surgery prosthesis may be applied. The method chosen depends on each person’s situation. Your physical therapist will help monitor the fit of these devices and teach you how to safely use them. The main goal of your care during this time is to protect the limb and reduce swelling.
Pain management. Your physical therapist will help with pain management in a variety of ways, including:
- Manual therapy, or “hands-on” treatments. These may include soft tissue (muscle, tendon) mobilization, joint manipulation, or gentle range-of-motion exercises.
- Limb management. This can include skin care and the use of a prosthetic shrinker.
- Desensitization. This technique includes methods to gently reduce the limb’s sensitivity to clothing, pressure, or touch.
- Mirror therapy or graded motor imagery. Your physical therapist may work with you to help reduce any ‘phantom’ sensation or pain below the amputation.
See the Physical Therapy Guide to Phantom Limb Pain for more information about amputation pain.
Prosthetic fitting. Your physical therapist will work with a specialist to choose the best prosthesis for your unique condition, situation, and goals. You may receive a temporary prosthesis while your limb continues to heal. The prosthesis will be modified to fit as needed over this time.
Physicians use the following criteria to determine when you are ready for a temporary prosthesis, or your first artificial limb:
- Your incision is almost healed or completely healed.
- Your swelling has decreased to an acceptable amount.
- You have regained sufficient strength to be able to walk safely.
After the limb has reached a stable shape and your physician approves it, you will be fitted for a permanent prosthesis. Walking with a transfemoral prosthesis can be a challenge. Physical therapy for gait training (learning to walk safely) is crucial at this stage.
Prosthetic and functional training. You will learn to function more independently once you receive a prosthesis. Your physical therapist will help you master movements, daily activities, and walking with an assistive device. You will learn a daily skin care routine and how to check for redness or blisters. It’s also important to continue exercise and positioning to prevent contractures.
Your physical therapist will teach you how to manage your new prosthesis. This can include putting it on and taking it off. You also can learn how to manage a good prosthetic socket fit. Your physical therapist will help you gradually build up tolerance for the prosthesis while protecting your skin. You may continue to use a wheelchair for getting around, even after you get your permanent prosthesis. Some people choose to use a wheelchair if their limb feels sore, or when waiting on a new or repaired prosthesis.
Guided rehabilitation. Full healing and a return to regular activity may take a full year or more. Amputation rehabilitation is a long journey. You may experience some setbacks, which are a normal part of the process. Managing your limb and the new prosthesis will require practice to learn and master. Talk to your physical therapist about your goals. Communicate your family responsibilities, work activities, and favorite hobbies. This will help your physical therapist design a treatment plan to reach or exceed your goals. Your recovery is a team effort.
Return to Recreational and Sports Activities
If you are active or have a favorite sport, you may want to consult with a recreational physical therapist. Some physical therapists have a practice focusing on adaptive sports. They can help you choose the right adaptive recreation equipment. See our article, Adaptive Sports: Staying Active While Living With a Disability for more information. Visit our Health Center for People with Disabilities. The Amputee-Coalition also offers many resources.
Depending on your personal goals, your physical therapist can help you return to sports such as golf, hiking, running, swimming, or cycling. A prosthetist can help you choose the best prosthetic device for taking part in these types of activities. You also may gain valuable advice from other people with amputations. Your physical therapist can help you find support groups in your area.
Can This Injury or Condition Be Prevented?
More than half of all amputations may be preventable. The leading causes of above-knee amputation are related to PVD (poor circulation), complicated by diabetes.
- Diligent diabetes management and foot care can greatly reduce the risk of developing problems that lead to leg amputations.
- Protect your feet by wearing shoes that fit correctly and maintain adequate space for your toes. Diabetic or orthopedic shoes are specially designed to protect your feet.
- It is also important to examine your legs and feet daily for signs of skin problems. These can include a change in color, swelling, blisters, scratches, or open wounds. See our article Feet First: Six Tips to Maintain Healthy Feet and the Freedom to Move for more tips.
- Consult your health care provider right away if you notice a problem. Address problems early to prevent them from getting worse.
- It is also important to stop smoking. Smoking cigarettes can greatly interfere with and delay wound healing in the feet and legs. Smokers with a prior amputation have a 25-times greater risk of reamputation (further removal) of the same limb than nonsmokers.
What Kind of Physical Therapist Do I Need?
All physical therapists are prepared through education and training to treat people with amputations. However, you may want to consider a physical therapist who has experience treating people with lower limb amputations.
You can find physical therapists with these and other credentials in your area by using Find a PT , the online tool built by the American Physical Therapy Association to help you search for physical therapists with specific clinical expertise.
General tips when you're looking for a physical therapist (or any other health care provider):
- Get recommendations from family, friends, or other health care providers.
- Ask your physician or prosthetist if they work closely with a physical therapist.
- Ask about the physical therapists' experience in helping people with a below-knee amputation before making an appointment.
The American Physical Therapy Association believes that consumers should have access to information that could help them make health care decisions and prepare them for a visit with their health care provider.
The following articles provide some of the best scientific evidence related to physical therapy treatment of transtibial amputation. The articles report recent research and give an overview of the standards of practice for treatment of it both in the United States and internationally. The article titles are linked either to a PubMed* abstract of the article or to free full text, so that you can read it or print out a copy to bring with you to your health care provider.
US Department of Veterans Affairs website. VA/DoD clinical practice guidelines for rehabilitation of lower limb amputation. Published 2017. Accessed May 15, 2024.
Amputee Coalition Organization website. Accessed May 15, 2024.
Cancer Treatment Centers of America. Accessed May 15, 2024.
American Diabetes Association. Accessed May 15, 2024.
Digital Resource Foundation for the Orthotics & Prosthetics Community. Accessed May 15, 2024.
The O&P Edge. Accessed May 15, 2024.
Health.mil. Accessed May 15, 2024.
*PubMed is a free online resource developed by the National Center for Biotechnology Information. PubMed contains millions of citations to biomedical literature, including citations in the National Library of Medicine's MEDLINE database.
Expert Review:
May 15, 2024
Revised:
Dec 13, 2024
Content Type: Guide
Above-Knee Amputation
PT, board-certified clinical specialist in orthopaedic physical therapy
Chris Doerger
PT
Michael Verbsky
PT
Toran D. MacLeod
PT, MPT, PhD
Dawn Drumm
PT, DPT, on behalf of the Academy of Acute Care Physical Therapy
You Might Also Like...
Article
Wound Management in Physical TherapyJul 8, 2024
Physical therapists who are wound management specialists have additional skills and expertise to provide wound healing treatments. Learn more about wound
Video
Physical Therapy Allowed Adaptive Surfing Champion to Regain IndependenceOct 25, 2018
After a motorcycle accident led to the above-knee amputation of her right leg, Dani Burt was determined to maintain and promote an active lifestyle. As
Podcast
Young Woman Overcomes Amputation Challenges, Becomes Adaptive Surfing ChampionJul 5, 2018
Dani Burt sustained devastating injuries in a motorcycle accident and awoke to learn that her right leg had been amputated above the knee.


