Physical Therapy Guide to Shoulder Impingement Syndrome
Shoulder impingement syndrome occurs as the result of chronic, repeated compression of the rotator cuff tendons. The condition is also called subacromial pain syndrome (which identifies where the pain is felt in the shoulder below the acromion). These include the long head of the biceps tendon, the bursa, or the ligaments in the shoulder. This impingement causes pain and movement problems. An injury to the shoulder also can cause this condition. People who do repeated overhead arm movements are most at risk for developing a shoulder impingement. It occurs more often among manual laborers and athletes (such as weightlifters, volleyball players, or baseball pitchers). Poor posture also can contribute to its development. If left untreated, a shoulder impingement can lead to more serious conditions, such as a rotator cuff tear. Physical therapists help decrease pain and improve shoulder motion and strength in people with shoulder impingement syndrome.
Physical therapists are movement experts who improve quality of life through:
- Hands-on care.
- Patient education.
- Prescribed movement.
You can contact a physical therapist directly for an evaluation. To locate a physical therapist in your area, visit Find a PT.
What Is Shoulder Impingement Syndrome?
iShoulder impingement syndrome develops when tendons, ligaments, or bursa in the shoulder are repeatedly compressed or “impinged.” This causes pain and movement problems. The shoulder is made up of three bones, called the:
- Humerus (the long bone of the upper arm).
- Scapula (shoulder blade).
- Clavicle.
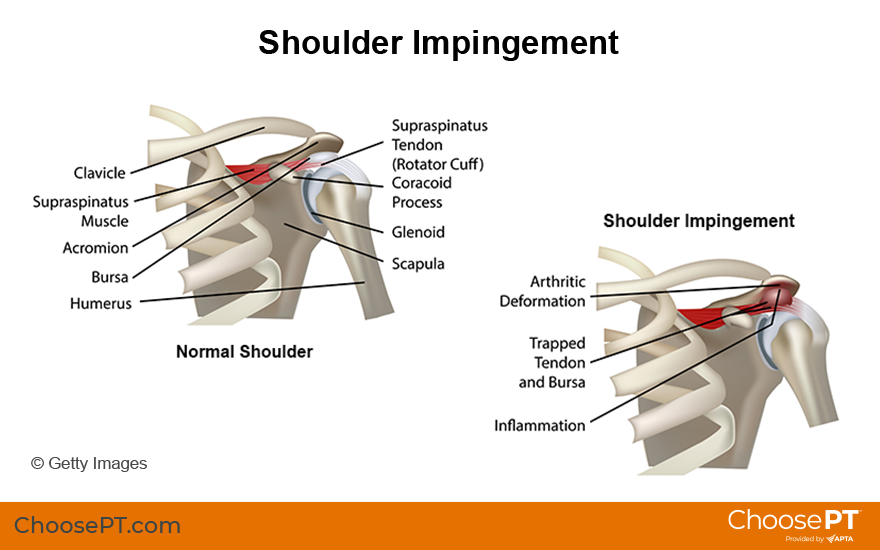
Shoulder impingement syndrome also may be called "subacromial" impingement syndrome. The rotator cuff tendon and the bursa sit beneath the acromion (a bony, bump-like prominence at the tip of the shoulder). Over time, these tissues can become compressed or pinched under the acromion:
- Rotator cuff tendons. These tendons are often the most affected by this condition.
- Long head of the biceps tendon.
- Ligaments.
- Bursa (a fluid-filled sac that provides a cushion between the bony acromion and the rotator cuff tendon.
Impingement symptoms also can occur when compression and microtrauma harm the tendon.
How Does It Feel?
People with shoulder impingement syndrome may experience:
- Restricted shoulder motion with weakness in movements such as reaching overhead, behind the body, or out to the side.
- Shoulder pain when moving the arm overhead, out to the side, and beside the body.
- Pain and discomfort when attempting to sleep on the involved side.
- Pain with throwing motions and other dynamic overhead movements.
How Is It Diagnosed?
An X-ray or MRI help to identify shoulder impingement syndrome. They also help to rule out other conditions that could be causing your discomfort. Before seeing a physical therapist, your doctor may refer you to have one of these tests.
Your physical therapist will perform a thorough evaluation. They will assess the degree of your condition or injury and determine any factors that may be contributing to it. Shoulder impingement syndrome can be the result of a single injury. However, it is much more likely that it develops over time due to repeated irritation in the shoulder region.
Your physical therapist will begin by gathering information about your condition. This will include your health history. They may be assisted by forms you fill out before your first session. Your physical therapist may ask questions such as:
- How did your injury occur?
- How have you taken care of the condition? Have you seen other health care providers or had imaging or other tests done, with results?
- What are your current symptoms? Do they change within a typical day?
- If there is pain, what is the location and intensity of your pain? Does your pain vary during the day?
- Are there any activities you are unable to do or have difficulties completing since the injury?
They will note any activities that make your symptoms worse or better.
This information helps your physical therapist to better understand your condition and determines the course of your physical examination. The physical exam will vary, but most often will begin with observing movements discussed during the interview. It will include the region of your symptoms and other neighboring areas that may have changed since your symptoms began. For example, your physical therapist may examine your lower arm, neck, and posture.
During your physical exam, your physical therapist will:
- Watch you move your arm and shoulder overhead and do other reaching tasks.
- Assess the mobility and strength of your shoulder and other regions of the body.
- Gently but skillfully palpate (feel) your shoulder and surrounding area to determine exactly where it is most painful.
The physical exam will help determine the areas that require treatment to improve your condition.
Your physical therapist will discuss their findings with you. They will work together with you to develop a program that begins your recovery.
How Can a Physical Therapist Help?
It is important to get proper treatment for shoulder impingement syndrome as soon as it occurs. If left untreated, secondary conditions can result from it, including:
- Irritation of the bursa.
- Rotator-cuff tendinitis or tears.
Physical therapy can successfully treat shoulder impingement syndrome. Your physical therapist will work with you to devise a treatment plan that is specific to your condition and goals. Your personalized treatment program may include:
- Patient education. Your physical therapist will educate you about your condition. They will work with you to identify any external factors causing your pain. They may recommend changes to the type and amount of exercises you perform, your athletic activities, and your home or work activities. They will develop a personalized exercise program to help ensure a pain-free return to your desired activities.
- Pain management. Your physical therapist will design a program to address your pain that includes applying ice to the affected area. They also may recommend changing some activities that cause pain. Physical therapists are experts in prescribing pain-management techniques that reduce or eliminate the need for medicines, including opioids.
- Range-of-motion exercise. The mobility of the shoulder joint and scapula can be limited. This causes increased stress to various structures. Your condition may be forcing the shoulder to work at a disadvantage. Your physical therapist may teach you self-stretching techniques to decrease tension and help restore normal motion of the shoulder region and arm function.
- Manual therapy. Your physical therapist may treat your condition using “hands-on” treatments (manual therapy) to gently move your muscles and joints. These techniques help improve motion. They also may be used to guide the region into a less stressful movement pattern.
- Muscle strengthening. Muscle weaknesses or imbalances can contribute to impingement of the shoulder joint as the scapula deviates due to weakness. Based on the level of your injury, your physical therapist will design a safe, personalized, progressive resistance program for you. It may include your core (midsection). You may begin by performing strengthening exercises lying on a treatment table or at home on the bed or floor. You then may advance to exercises in a standing position. Your physical therapist will choose what exercises are right for you, based on your age and physical condition. Your plan may include using resistance machines at the clinic. Your physical therapist also will determine if going to a gym is appropriate.
- Functional training. Once your pain, strength, and motion improve, you will need to safely transition back into more demanding activities. To minimize the stress to the shoulder joint, it is important to teach your body safe, controlled movements. Based on your movement assessment and goals, your physical therapist will create a series of activities to help you learn how to use and move your body correctly and safely. These may include retraining of activities such as throwing, swinging a racket, or a work activity.
Can This Injury or Condition Be Prevented?
Shoulder impingement syndrome can be prevented by:
- Maintaining proper strength in the shoulder and shoulder-blade muscles. A healthy shoulder relies on the proper balance of muscle strength in the shoulder region. If there is an imbalance in muscle strength, over time, there is an increased risk for impingement and injury.
- Maintaining proper shoulder, neck, and middle-back range of motion and mobility. The shoulder relies on the mobility of neighboring joints to maintain healthy, proper function.
- Keeping proper posture and using proper shoulder mechanics when reaching and throwing. This reduces the likelihood of shoulder impingement and reduces excessive stress on the shoulder.
- Avoiding forward-head and rounded-shoulder postures (such as spending a lot of time hunched over, sitting at a computer). Poor posture habits put the shoulder in positions that increase the chances for an impingement.
What Kind of Physical Therapist Do I Need?
All physical therapists are prepared, through education and experience, to treat shoulder impingement syndrome. You may want to consider the following when selecting a physical therapist:
- A physical therapist who is experienced in treating people with shoulder impingement syndrome. Some physical therapists have a practice with an orthopaedic or musculoskeletal focus.
- A physical therapist who is a board-certified clinical specialist, or who completed a residency or fellowship in orthopaedic or sports physical therapy. This physical therapist has advanced knowledge, experience, and skills that may apply to your condition.
You can find physical therapists who have these and other credentials by using Find a PT , the online tool built by the American Physical Therapy Association to help you search for physical therapists with specific clinical expertise in your geographic area.
General tips when you are looking for a physical therapist (or any other health care provider):
- Get recommendations from family, friends, or other health care providers.
- When you contact a physical therapy clinic for an appointment, ask about the physical therapists' experience in helping people who have shoulder impingement syndrome.
- During your first visit with the physical therapist, be prepared to describe your symptoms in as much detail as possible and say what makes your symptoms worse.
The American Physical Therapy Association believes that consumers should have access to information to help them make informed health care decisions and prepare them for a visit with their health care provider.
The American Physical Therapy Association believes that consumers should have access to information to help them make informed health care decisions and prepare them for their visit with a health care provider.
The following resources offer some of the best scientific evidence related to physical therapy treatment for shoulder impingement syndrome. They report recent research and give an overview of the standards of practice both in the United States and internationally. They link to a PubMed* abstract which may also offer free access to the full text, or to other resources. You can read them or print out a copy to bring with you to your health care provider.
Camargo PR, Alburquerque F, Avila MA, et al. Effects of stretching and strengthening exercises, with and without manual therapy, on scapular kinematics, function, and pain in individuals with shoulder impingement: a randomized controlled trial. J Orthop Sports Phys Ther. 2015;45(12):984–997. Article Summary in PubMed.
Khan Y, Nagy MT, Malal J, Waseem M. The painful shoulder: shoulder impingement syndrome. Open Orthop J. 2013;347–351. Article Summary in PubMed.
Struyf F, Nijs J, Baeyens JP, Mottram S, Meeusen R. Scapular positioning and movement in unimpaired shoulders, shoulder impingement syndrome, and glenohumeral instability. Scand J Med Sci Sports. 2011;21(3):352–358. Article Summary on PubMed .
*PubMed is a free online resource developed by the National Center for Biotechnology Information. PubMed contains millions of citations to biomedical literature, including citations in the National Library of Medicine’s MEDLINE database.
Expert Review:
Jan 3, 2021
Revised:
Jan 3, 2021
Content Type: Guide
Shoulder Impingement Syndrome
PT, MPT
Wilfred Diaz
PT, DPT, board-certified clinical specialist in orthopaedic physical therapy
Stephen F. Reischl
PT, DPT, board-certified clinical specialist in orthopaedic physical therapy, on behalf of the Academy of Orthopaedic Physical Therapy
You Might Also Like...
Patient Stories
'Famous Amos' Founder Relies On His Physical TherapistJul 29, 2021
Amos is convinced that his success is a result of the individual attention he received from a physical therapist who understood his body and cared about
