Physical Therapy Guide to Ankylosing Spondylitis
Ankylosing spondylitis is an inflammatory disease. It causes pain and stiffness in the spine, pelvis, and other joints (hips, shoulders, knees, and ankles). AS is a chronic (lifelong) disease. Researchers believe that it is genetic (passed on through one’s parents). A majority of people who have AS carry a gene called HLA-B27. Around 80% of people who carry the HLA-B27 gene do not develop the disease. AS typically develops in people between ages 17 and 45, with an average age of 24. Males are more likely to have AS than females. They also tend to have more severe symptoms than females.
Physical therapists help people with AS keep their physical function and manage symptoms. They work with patients to maximize their strength, muscle flexibility, joint mobility, posture, movement habits, and physical conditioning. Physical therapy and exercise are considered key elements in treating AS.
Physical therapists are movement experts. They improve quality of life through hands-on care, patient education, and prescribed movement. You can contact a physical therapist directly for an evaluation. To find a physical therapist in your area, visit Find a PT.
What Is Ankylosing Spondylitis?
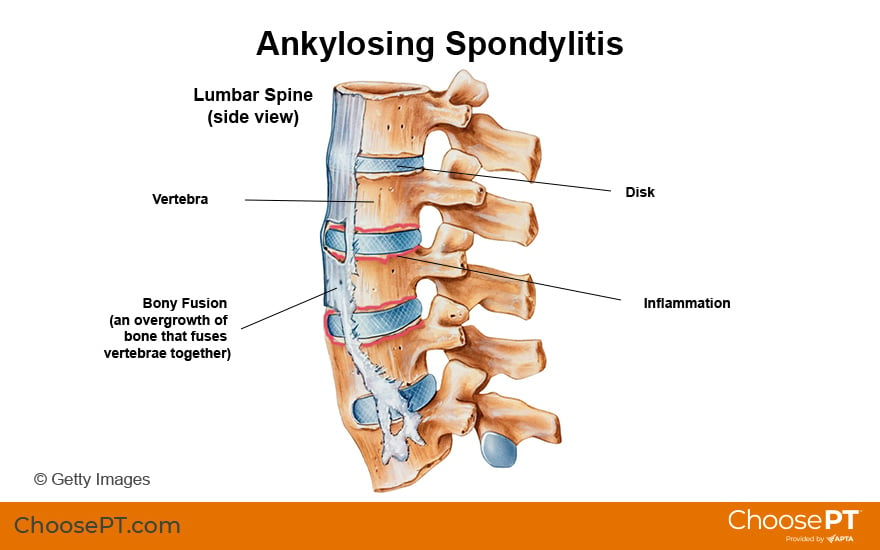
Ankylosing spondylitis is an inflammatory disease. It affects the spine, pelvis, and joints throughout the body. AS causes inflammation in the part of the bone where ligaments and tendons attach. This inflammation can lead to fusion (growing together) of the joints in the pelvis (sacroiliac) and spine. AS affects both the muscles and joints. People with AS also can have problems with their:
- Eyes (uveitis).
- Skin (psoriasis).
- Gastrointestinal system (inflammatory bowel disease or IBD).
- Heart, lungs, and kidneys, though involvement with these is not common.
There is no cure for AS. But proper treatment can greatly help to improve quality of life for people living with the disease by improving:
- Pain.
- Stiffness.
- Physical function.
Medicines help manage the inflammation that causes symptoms. In some cases, total hip replacement and other surgeries can be performed if needed. Doctors may consider surgery if the joints become too stiff and painful to manage with medicine and physical therapy.
How Does It Feel?
The most common symptom that occurs with AS is pain and stiffness in the sacroiliac joints (at the base of the spine) and low back. Pain is especially worse in the middle of the night. People with AS may also experience hip and shoulder pain. The pain linked to AS often occurs along with morning stiffness that lasts more than one hour and/or stiffness after long periods of being inactive. Both of these kinds of stiffness often improve with exercise or physical activity. People with AS also can experience general fatigue and poor sleep.
If left unchecked, bony fusion (where bones grow together), or ankylosis, due to AS in the neck, spine, and hip joints can cause:
- Stiffness that gets worse over time and reduces your ability to turn your head, stand upright, or bend.
- Trouble keeping good posture. People with AS may stoop forward, which can make it harder to walk and increases the risk of falling. This “stooped” posture may also increase stress and pain in the spine.
- Osteopenia or osteoporosis (low bone mass). This can increase the risk of fractures (broken bones), especially in the spine and hips.
- Breathing problems. Joints where the ribs and spine attach can become stiff, which may limit chest and lung expansion. This stiffness can lead to shortness of breath and increased risk of lung infections.
In about 40% of cases, AS can affect the soft tissues of the eye (uveitis). If the eye is affected, a person may have eye pain, blurred vision, and increased sensitivity to light. People with AS also can have skin conditions (psoriasis) and inflammatory bowel disease, which may cause abdominal pain, diarrhea, and/or weight loss.
How Is It Diagnosed?
If you see a physical therapist first for symptoms, such as chronic back pain, they will perform a thorough evaluation. The goal is to determine all the factors that may be contributing to your condition. If AS is suspected, the physical therapist will consult with your doctor for further tests. These may include an X-ray or MRI of the spine and sacroiliac joints. Your doctor also may order blood and genetic tests. If you test positive for the HLA-B27 gene, it might mean you are at higher risk for developing AS. A qualified doctor must interpret these results before a diagnosis.
Your physical therapist will begin with an interview to gather information. They will ask about your health history, condition, and activities. They also may ask questions about your experience, such as:
- What are your current symptoms? When did symptoms first begin?
- Do your symptoms get worse, stay the same, or improve with activity?
- Do you have pain, and if so, what is the location and intensity of your pain? Does pain vary during the day? Is it waking you up at night?
- Do you have trouble doing any activities? What activities are you unable to do?
This information helps your physical therapist understand what you are experiencing. It also will help to determine the course of the physical exam and treatment.
The physical exam often begins by your physical therapist observing any movements or positions that cause pain. It also may include:
- Watching you walk with and without shoes on. Your physical therapist may watch you go up and down stairs. They also may ask you to show them how you pick up an object from the floor.
- Assessing posture and the range of motion (movement) of the spine, hips, knees, and shoulders.
- Checking for any tender spots around the spine, hips, and sacroiliac joints.
- Assessing your ability to bend down (squat), and balance on each leg.
- If the physical therapist suspects AS, they will perform other tests such as measuring your chest expansion after asking you to take a deep breath and exhale. This will help them assess how AS may be affecting your rib joints and breathing function.
How Can a Physical Therapist Help?
A physical therapist can help people with AS:
- Improve posture, strength, muscle flexibility, joint mobility, conditioning, and efficiency of movement.
- Manage symptoms such as pain and stiffness.
- Perform everyday activities more easily.
Your physical therapist will develop a treatment plan specific to your condition and goals. It may include:
Patient education. Your physical therapist will educate you about ankylosing spondylitis. This knowledge will help you make decisions about your physical activities. They will work with you to identify any problems around the type and amount of activities and exercises you do and your everyday activities. Your physical therapist will recommend changes to your exercise routine and daily activities as needed. They also will develop a personalized exercise program to help you maximize your physical function.
Posture training. Improving posture to avoid slouching or forward bending can reduce pain in the spine and other joints. It also can reduce the risk of falling.
Strengthening exercises. Improving the strength in your back and abdominal muscles can reduce pain and improve your posture. It also can improve your ability to walk and do normal daily activities.
Flexibility exercises. Range-of-motion and stretching exercises help keep the spine and other joints from getting stiff. They also help you maintain more flexible muscles and joints. Your physical therapist will teach you exercises that can help improve pain and physical function. These exercises also may decrease the risk of bony fusion.
Aerobic exercise. Low-impact exercise such as walking, swimming, or bike riding can reduce the risk of heart disease. It also can reduce the risk for pain, stiffness, and fatigue in people with AS. Your physical therapist can help you figure out the best way to get aerobic exercise.
Deep-breathing exercises. Your physical therapist may teach you exercises to improve chest expansion. This will allow you to breathe more easily. The goal of these exercises is to increase oxygen and blood flow in the body. Getting enough blood flow and oxygen throughout the body can help decrease stiffness, pain, and fatigue.
Movement retraining. Physical therapists teach people with AS how to move more efficiently. Movement retraining can improve your energy levels and ability to function. It also can help reduce pain and fatigue. Your physical therapist also may recommend equipment to:
- Improve walking.
- Lessen pain.
- Reduce your risk of falling.
Your physical therapist will work with other members of your health care team as needed to ensure the best possible care.
After Surgery
If your hip joints have developed severe arthritis, your doctor may recommend a total joint replacement. Physical therapists help people recover after surgery. They will work with you to help you:
- Regain strength, flexibility, and endurance.
- Improve your walking ability and balance.
- Help you safely return to your usual daily activities.
Can This Injury or Condition Be Prevented?
AS is a genetic disease. There is no way to prevent it yet. However, a physical therapist can help you improve your physical function and manage your symptoms. Physical therapists teach you the best way to move and hold your body (posture correction). They design and prescribe exercise programs specific to your condition for stretching, strengthening, and conditioning. Your physical therapist will work with you to help you function at your highest level.
What Kind of Physical Therapist Do I Need?
All physical therapists are prepared through education and clinical experience to treat problems of the spine. However, you may want to consider:
- A physical therapist who has experience treating people with ankylosing spondylitis. Some physical therapists have a practice with an orthopedic focus.
- A physical therapist who is a board-certified clinical specialist in orthopedic physical therapy, or who has completed a residency or fellowship in orthopedic physical therapy. This physical therapist has advanced knowledge, experience, and skills that may apply to your condition.
You can find physical therapists in your area with these credentials and clinical expertise on Find a PT, a tool built by the American Physical Therapy Association.
General tips when you are looking for a physical therapist (or other health care provider):
- Ask family, friends, and other health care providers to recommend a physical therapist.
- Ask about the physical therapist’s experience treating ankylosing spondylitis or other orthopedic conditions before you make an appointment.
- Be prepared to describe your symptoms in as much detail as possible on your first visit, including what makes your symptoms better or worse.
The American Physical Therapy Association believes that consumers should have access to information to help them make informed health care decisions and prepare them for their visit with a health care provider.
The following resources offer some of the best scientific evidence related to physical therapy treatment for ankylosing spondylitis. They report recent research and give an overview of the standards of practice both in the United States and internationally. They link to a PubMed* abstract, which may also offer free access to the full text, or to other resources. You can read them or print out a copy to bring with you to your health care provider.
Gianotti E, Trainito S, Arioli G, Rucco V, Masiero S. Effects of physical therapy for the management of patients with ankylosing spondylitis in the biological era. Clin Rheumatol. 2014;33(9):1217-1230. : Article Summary in PubMed.
National Institute of Arthritis and Musculoskeletal and Skin Disease. : What is ankylosing spondylitis? Fast facts: an easy-to-read series of publications for the public. Published April 2011.
Ince G, Sarpel T, Durgun B, Erdogan S. Effects of a multimodal exercise program for people with ankylosing spondylitis [erratum in: Phys Ther. 2006;86(10):1452]. Phys Ther. 2006;86(7):924-935. : Article Summary in PubMed.
Spondylitis Association of America: About ankylosing spondylitis.
Martey C and Sengupta R. Physical therapy in axial spondyloarthritis: guidelines, evidence and clinical practice. Curr Opin Rheumatology. 2020;32:365-70. : Article Summary in PubMed.
Millner JR, et al. Exercise for ankylosing spondylitis: an evidence-based consensus statement. Sem Arth Rheum. 2016; 45:411-27. : Article Summary in PubMed.
O’Dwyer T, O’Shea, Wilson F. Physical activity in spondyloarthritis: a systematic review. Rheumatol Int. 2015;35:393-404. : Article Summary in PubMed.
Perotta FM, Musto A, Lubrano E. New insights in Physical Therapy and Rehabilitation in axial spondyloarthritis: a review. Rheumatol Ther. 2019;6:479-86. : Article Summary in PubMed.
Regnaux JP, Davergne T, Palazzo C, Roren A, Rannou F, Boutron I, Lefevre-Colau MM. Exercise programs for ankylosing spondylitis. Cochrane Database of Systematic Reviews 2019, Issue 10. : Article Summary in PubMed.
*PubMed is a free online resource developed by the National Center for Biotechnology Information. PubMed contains millions of citations to biomedical literature, including citations in the National Library of Medicine's MEDLINE database.
Expert Review:
Jun 17, 2021
Revised:
Nov 15, 2021
Content Type: Guide
Ankylosing Spondylitis
PT, DPT, board-certified clinical specialist in orthopaedic physical therapy
Andrew Lui
PT, DPT
Stephen F. Reischl
PT, DPT, board-certified clinical specialist in orthopaedic physical therapy, on behalf of the APTA Academy of Orthopaedic Physical Therapy