Physical Therapy Guide to Lymphedema
Lymphedema is swelling in the arms or legs due to a disruption of lymph fluid flow through the lymphatic system. This disruption causes fluid to accumulate under the skin. The most common cause of lymphedema is the removal of lymph nodes. It also can be caused by an obstruction that blocks lymph fluid movement. About one in five women who are living with or beyond breast cancer and who have had the lymph nodes in their underarm removed during breast cancer treatment will develop lymphedema. Lymphedema generally develops three months to 20 years after cancer treatment. Identifying and treating lymphedema early helps to ensure more rapid and improved outcomes. Still, treatment provided later during the chronic stages of the disease can help. Physical therapists work closely with you and other members of your health care team to help control swelling caused by lymphedema and meet your goals for returning to your activities.
Physical therapists are movement experts. They improve quality of life through hands-on care, patient education, and prescribed movement. You can contact a physical therapist directly for an evaluation. To find a physical therapist in your area, visit Find a PT.
Check with your doctor or physical therapist immediately if you have swelling in one of your limbs and:
- Have cancer.
- Received treatment for cancer.
- Have a heart, kidney, or liver condition or develop any unexplained swelling.
What Is Lymphedema?
The lymphatic system collects lymph fluid (excess fluid, proteins, and other substances) from the body tissues and carries it back to the bloodstream. Lymph fluid moves slowly through lymphatic vessels and passes through lymph nodes as it returns to the bloodstream. Swelling occurs when the normal drainage of fluid is disrupted, and lymph fluid accumulates in the body tissues. This can be due to a blockage or surgical removal of lymph nodes. This results in large amounts of lymph fluid collecting in the tissue.
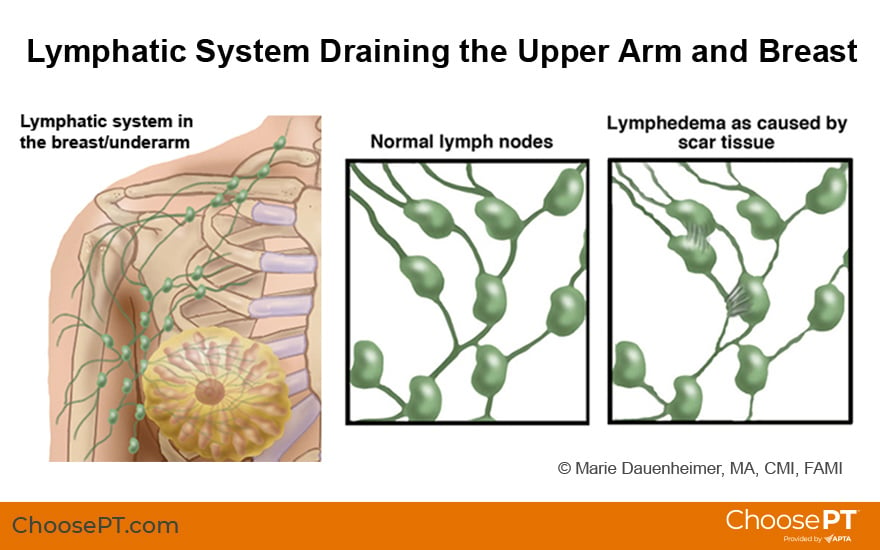
Lymphedema can be a hereditary condition. Most often, however, it results from blockages in lymph vessels caused by infection, cancer, and scar tissue due to radiation therapy or the surgical removal of lymph nodes.
You are at greater risk for lymphedema if you:
- Had surgery to remove your lymph nodes in the underarm, groin, or pelvic area.
- Received radiation therapy to your underarm, groin, pelvic region, or neck.
- Have scar tissue in the lymphatic ducts, veins, or under the collarbones, caused by surgery or radiation therapy.
- Received taxane chemotherapy.
- Have cancer that has spread to the lymph nodes in the neck, chest, underarm, pelvis, or abdomen.
- Have tumors in the pelvis, abdomen, or chest that put pressure on your lymphatic vessels and/or lymphatic duct and block fluid drainage.
- Have inflammation of the arm or leg after surgery.
- Are older.
- Have a poor diet or are overweight. These conditions may delay recovery from surgery and radiation therapy and increase the risk of lymphedema.
Signs and Symptoms
With lymphedema, you may have:
- Swelling in your arms, legs, shoulders, hands, fingers, chest, or neck.
- Skin that feels tighter, harder, or thicker than normal in the affected area.
- Aching, tingling, or a feeling that your arm or leg is heavy.
- Weakness in your arm or leg.
- Inability to move certain joints, such as your wrist or ankle, as freely as usual.
- Pitting (indentation) in the tissues of your limb (made by pressing a finger on the skin that takes time to “fill in” after removing the pressure).
- Clothing, rings, bracelets, or shoes that fit tighter than before.
- Repeated infections in your arm or leg.
- Joint pain.
- Difficulty doing your daily activities.
If you have fever and chills, and your limb with lymphedema is red, swollen, or painful and feels warm to the touch, you may have an infection. Contact your doctor.
How Is It Diagnosed?
Your physical therapist will review your medical history and medicines and perform a thorough physical examination. They also will gather the following information:
- Your actual weight compared with your ideal weight.
- Circumference measurements of your arms, legs, chest, and neck.
- How well you’re able to do activities of daily living. These include bathing and grooming, dressing and undressing, or walking, eating, and drinking.
- Whether you have a history of edema, radiation therapy, chemotherapy treatments, or surgery.
- The amount of time between surgery and when you first noticed the swelling in a limb.
- A history of other chronic health conditions such as diabetes, high blood pressure, kidney disease, heart disease, or phlebitis (inflammation of the veins).
How Can a Physical Therapist Help?
Your physical therapist will serve as an important member of your health care team. They will work closely with you to design a treatment program to help control the swelling and meet your goals for returning to your activities.
In the early stages of lymphedema, when the swelling is mild, it often can be managed by techniques that encourage lymph flow such as:
- Compression garments.
- Exercise.
- Elevation of the affected limb.
For more severe swelling, your physical therapist may use a treatment plan called complete decongestive therapy to help improve the flow of lymph fluid. This includes:
- Manual lymphatic drainage, which feels like a light form of massage.
- A personalized exercise program.
- Compression bandaging to help reduce your swelling.
- Providing you with information on skin and nail hygiene to reduce the risk of infection.
Your physical therapist will carefully monitor the size of your affected limb throughout your treatment sessions. Once the size of your limb has decreased to the desired measurements, your physical therapist will help you begin to take over your own care and will:
- Develop a safe and sensible personalized exercise program for you to do on your own. This program will help you increase your physical fitness without overly straining your affected arm or leg.
- Update your compression garments to ensure they fit properly and best meet your needs.
- Educate you about how proper nutrition and diet, and skin and nail care can help reduce your risk of infection.
Can This Injury or Condition Be Prevented?
Some risk factors for lymphedema, such as treatment for cancer, cannot be avoided. If you have had your lymph nodes removed, or received radiation or certain chemotherapies, but you don’t have lymphedema, you might still be at risk for developing it. Your physical therapist will help you identify factors that may increase your risk for lymphedema. They will provide you with suggestions for managing these risks so that you can reduce the likelihood of developing it.
Your physical therapist will:
- Design a safe and sensible individualized home exercise program to improve your overall fitness and help you avoid a weight gain that can increase your risk of lymphedema.
- Develop a safe and sensible exercise program that will avoid straining the affected limb and help you reduce the risk of developing lymphedema following surgery or infection.
- Periodically assess the size of your limb and, if there is an increase in limb size, provide conservative, early intervention to help prevent further swelling.
- Help you maintain good skin/nail care and hygiene.
Poor drainage of the lymphatic system might make infection of your arm or leg more likely. Even a small infection could lead to serious lymphedema. You can help prevent infections from occurring by avoiding cuts and abrasions, burns, punctures, and insect bites on your affected limb.
What Kind of Physical Therapist Do I Need?
Although all physical therapists are prepared by their education and experience to treat a variety of conditions, including lymphedema, you may want to consider:
- A physical therapist who is experienced in treating lymphedema.
- A physical therapist who has completed specific training in lymphedema management and has advanced knowledge, experience, and skills that apply to your condition.
You can find physical therapists who have these and other credentials by using Find a PT , the online tool built by the American Physical Therapy Association to help you search for physical therapists with specific clinical expertise in your geographic area.
General tips when you’re looking for a physical therapist (or any other health care provider):
- Get recommendations from family, friends, or other health care providers for physical therapists trained in managing lymphedema.
- When you contact a physical therapist for an appointment, ask about their experience in helping people with lymphedema.
- Be prepared to describe your symptoms in as much detail as possible, and say what makes your symptoms worse.
The American Physical Therapy Association believes that consumers should have access to information that could help them make health care decisions and also prepare them for a visit with their health care provider.
APTA has determined that the following articles provide some of the best scientific evidence on treating lymphedema. The articles report recent research and give an overview of the standards of practice for treatment both in the United States and internationally. The article titles are linked either to a PubMed* abstract of the article or to free access of the full article, so that you can read it or print out a copy to bring with you to your health care provider.
Davies CC, Levenhagen K, Ryans K, Perdomo M, Gilchrist L. Interventions for breast cancer-related lymphedema: clinical practice guideline from the Academy of Oncologic Physical Therapy of the APTA. Phys Ther. 2020;100(7):1163–1179. Article Summary on PubMed.
Thompson B, Gaitatzis K, Janse de Jonge X, Blackwell R, Koelmeyer LA. Manual lymphatic drainage treatment for lymphedema: a systematic review of the literature. J Cancer Surviv. 2020 Aug 15 [Epub ahead of print]. Article Summary on PubMed.
Michelotti A, Invernizzi M, Lopez G, et al. Tackling the diversity of breast cancer related lymphedema: perspectives on diagnosis, risk assessment, and clinical management. Breast. 2019;44:15–23. Article Summary on PubMed.
Bernas M, Thiadens SR, Smoot B, Armer JM, Stewart P, Granzow J. Lymphedema following cancer therapy: overview and options. Clin Exp Metastasis. 2018;35(5-6):547–551. Article Summary on PubMed.
Kilgore LJ, Korentager SS, Hangge AN, et al. Reducing breast cancer-related lymphedema (BCRL) through prospective surveillance monitoring using bioimpedance spectroscopy (BIS) and patient directed self-interventions. Ann Surg Oncol. 2018;25:2948-2952. Article Summary in PubMed.
Kaufman DI, Shah C, Vicini FA, Rizzi M. Utilization of bioimpedance spectroscopy in the prevention of chronic breast cancer-related lymphedema [correction published in Breast Cancer Res Treat. 2017;166(3):817]. Breast Cancer Res Treat. 2017;166:809-815. Article Summary in PubMed.
Levenhagen K, Davies CC, Perdomo M, Ryans K, Gilchrist L. Diagnosis of upper quadrant lymphedema secondary to cancer: clinical practice guideline from the Oncology Section of the American Physical Therapy Association. Phys Ther. 2017;97(7):729–745. Article Summary on PubMed.
Shaitelman SF, Cromwell KD, Rasmussen JC, et al. Recent progress in the treatment and prevention of cancer-related lymphedema. CA Cancer J Clin. 2015;65(1):55–81. Article Summary on PubMed.
Bevilacqua JL, Kattan MW, Changhong Y, et al. Nomograms for predicting the risk of arm lymphedema after axillary dissection in breast cancer. Ann Surg Oncol. 2012;19(8):2580–2589. Article Summary on PubMed.
Quirion E. Recognizing and treating upper extremity lymphedema in postmastectomy/lumpectomy patients: a guide for primary care providers. J Am Acad Nurse Pract. 2010;22:450–459. Article Summary on PubMed.
Gilchrist LS, Galantino ML, Wampler M, et al. A framework for assessment in oncology rehabilitation. Phys Ther. 2009;89:286–306. Article Summary in PubMed.
*PubMed is a free online resource developed by the National Center for Biotechnology Information. PubMed contains millions of citations to biomedical literature, including citations in the National Library of Medicine’s MEDLINE database.
Expert Review:
Sep 17, 2020
Revised:
Sep 17, 2020
Content Type: Guide
Lymphedema
an academy of the American Physical Therapy Association
an academy of the American Physical Therapy Association
PT, PhD
G. Stephen Morris
PT, PhD, fellow of the American College of Sports Medicine, on behalf of the Academy of Oncologic Physical Therapy
Claire C. Davies
PT, PhD
You Might Also Like...
Article
Pelvic and Women's Health Physical TherapyJul 9, 2024
Pelvic and women's health physical therapy focuses on treating the many abdominal and pelvic health concerns of adults and children with pelvic health
Article
Oncologic Physical TherapyJul 9, 2024
Oncologic physical therapists focus on or specialize in providing physical therapist services for persons affected by cancer and cancer survivors of all
Health Tips
10 Ways Physical Activity and Exercise Help During Cancer TreatmentApr 15, 2024
Physical activity and exercise provide short- and long-term benefits for people undergoing cancer treatment. Here's why it's recommended and how it can


