Physical Therapy Guide to Knee Osteoarthritis
Knee osteoarthritis is a condition that results from degenerative changes to the cartilage, or cushion, between the bones of the knee joint. Knee OA can make everyday activities more difficult due to general knee discomfort and pain. In the United States, nearly 12.4 million people ages 65 or older have symptomatic knee OA. This condition often affects women more than men. Even though knee OA is more common in older adults, people as young as age 45 can show symptoms. Physical therapists treat people with knee OA to help reduce pain and improve movement (mobility). They design personalized treatment programs to help people of all ages and abilities with the condition. And, according to a new study, choosing physical therapy for osteoarthritis of the knee outperforms steroid injections and is cost-effective.
Physical therapists are movement experts. They improve quality of life through hands-on care, patient education, and prescribed movement. You can contact a physical therapist directly for an evaluation. To find a physical therapist in your area, visit Find a PT.
What Is Knee Osteoarthritis?
Knee OA results from inflammation and wear and tear of the cartilage between the bones of the knee joint. It can affect the entire joint, including its bones, surrounding ligaments, and muscles.
Knee OA may worsen over time and make it challenging to do everyday activities due to pain and discomfort. The following factors can affect how quickly symptoms worsen:
- Age.
- Body structure.
- Body mass index.
- Sex (male or female).
- Ethnicity.
- Strength.
- Activity level.
Knee OA may develop over time after a ligament or cartilage injury in the knee. Physical therapy has been proven to successfully manage knee OA. Seeing a physical therapist early can help slow the progression of the condition, or even prevent it from becoming worse. Proper treatment also can help people delay or avoid surgery. Although physical therapy is successful in many cases, some patients may still require surgery based on the severity of their condition.
How Does It Feel?
Knee OA has a wide range of symptoms. The most common symptom is pain around the knee joint. Knee mobility also may decrease. When knee cartilage wears down, it can expose the underlying bone in certain spots. This causes increased stress on and compression of the remaining cartilage. As cartilage wears down, the bones in your knee joint rub together causing friction that makes your knee hurt and become stiff or swollen. You also may feel grinding or hear popping sounds while bending your knee.
Your activity level as well as the amount and types of activities you do can impact your symptoms. For example, symptoms may worsen with activities such as walking without supportive shoes or using the stairs.
Symptoms of knee OA may include:
- Morning stiffness lasting less than 30 minutes.
- Pain during or after activity. Examples include walking, climbing or going down stairs, or rising from a chair to stand.
- Pain or stiffness after sitting with the knee bent or straight for a long time.
- A feeling or sound of popping, cracking, or grinding when moving the knee.
- Swelling after activity.
- Tenderness to touch along the knee joint.
Typically, these symptoms develop slowly over time rather than suddenly. Some people do not know they have knee OA, due to a lack of symptoms. Or they may not remember a specific injury that caused their symptoms to begin. If you have worsening knee pain that lasts several months and does not improve with rest, see your doctor or physical therapist.
How Is It Diagnosed?
There are two methods for diagnosing knee OA:
- Self-reporting of symptoms and a physical exam.
- Diagnostic imaging (X-ray or MRI).
Physical therapists identify, diagnose, and treat movement problems, such as those common with knee OA. Your physical therapist will ask you questions about your medical history and activity. They will perform a physical exam to get measurements that include your knee’s:
- Range of motion.
- Strength.
- Mobility.
- Flexibility.
Your physical therapist may recommend that you get imaging such as X-rays of your knee to gain more information on the condition of your knee joint. X-rays are good at detecting OA in the knee. If your doctor suspects more severe joint or tissue damage, they may order an MRI to get a more detailed view of the joint and surrounding tissues. They also may order blood tests to rule out other conditions or other types of arthritis that can cause symptoms similar to knee OA.
How Can a Physical Therapist Help?
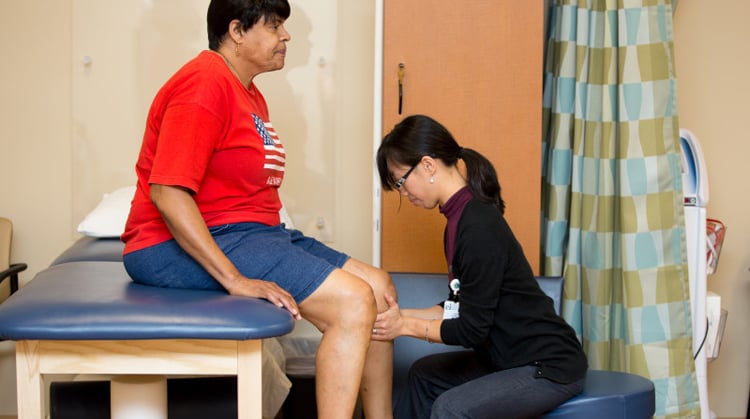
Your physical therapist will design a personalized treatment program specific to your condition and goals. Your program may include:
Range-of-motion exercises. Your physical therapist will assess your range of motion. They will compare the motion of your affected knee with that of your healthy knee. They will select specific flexibility exercises to help improve your ability to bend and straighten your knee.
Muscle strengthening. Research shows that people with knee OA who follow a program to improve their muscle strength have less pain and improved quality of life. Improving the strength of the muscles in the leg can help minimize the wear and tear of cartilage in the knee, control knee movement, and reduce the amount of force on the joint when moving.
Strengthening the hip and "core" muscles can help balance the amount of force on the knee joint during walking, running, and other repetitive movements. The core refers to the muscles of the stomach, low back, and pelvis. A strong core increases stability throughout your body. Your physical therapist will assess these different muscle groups, compare the strength in each leg, and design an exercise program to target your areas of weakness.
Manual therapy. Physical therapists are trained in manual (hands-on) therapy. Your physical therapist will gently move your muscles, loosening them to gain more range of motion in your knee joint and increase your flexibility. In many cases, manual therapy can be used along with stretching to produce lasting benefits. These techniques can target areas that are difficult to treat on your own. Research shows that adding manual therapy to an exercise program can decrease pain and increase functional mobility.
Bracing. Compression sleeves around the knee may help reduce pain and control swelling. Devices such as braces can help modify the forces placed on the knee. Different braces can help reduce stress on specific areas of your knee. By distributing pressure to less painful areas of the joint they may allow you to do weight-bearing activities with less pain. Depending on your symptoms and knee condition, your physical therapist will determine the best brace, if any, for you.
Activity recommendations. Since knee OA could worsen over time, it is important to do the right types of activities, while avoiding too much stress on the knee. Your physical therapist can guide you in modifying your activities, and changing how often you do them, if needed. In some cases, aquatic therapy (provided in a pool) can produce great benefits by enabling knee strengthening while minimizing the pressure on the knee. Your physical therapist will prescribe and monitor exercises based on your specific condition and abilities. Sometimes, using an assistive device such as a cane may help as well.
Other treatments. Your physical therapist may recommend how and when to use therapeutic methods such as ice and heat to aid in pain management. Physical therapists are experts at using movement, positioning, and other methods to help reduce pain and avoid the use of medications, including opioids.
Numerous studies have shown that physical therapy is very effective in helping manage osteoarthritis of the knee. In a recent study, researchers calculated the economic impact of choosing physical therapy for OA of the knee over steroid injections, and found that doing so saves $13,981, including all the hidden costs of your time, pain, missed life events, and the dollars paid for services.
If Surgery Is Required
In some cases of knee OA, the cartilage (also called the meniscus) may have a tear and is not able to absorb shock. Surgery to repair or remove parts of this cartilage may be needed if physical therapy, injections, and anti-inflammatory medications are unsuccessful. However, research shows that 70% of patients with a meniscus tear who were deemed candidates for surgery did not need surgery if physical therapy was received first. Physical therapy is an effective alternative for many people with knee OA who would prefer to avoid or delay surgery.
If, after consulting with professionals, you choose to have a recommended surgery, physical therapy will be an integral part of your preparation and recovery. It is important to note that in severe cases of osteoarthritis, a total knee replacement can provide 90% to 95% of pain relief. Factors to consider with your doctor and physical therapist before choosing surgery include:
- The severity of wear and tear in the knee joint.
- Age.
- Body mass index.
- Strength.
- Activity level.
- Overall health.
If needed, your physical therapist can refer you to an orthopedic surgeon to discuss your options. Should you choose surgery, your physical therapist can assist you beforehand with "prehab." Prehab is a shorter stint of physical therapy with surgery-specific exercises to improve your knee strength and flexibility before surgery. Following surgery, your physical therapist will design a program based on your condition and goals, which will include some or all of the treatments listed above. Your specific program will depend on:
- The type of surgery you received.
- Your overall level of function.
- Your fitness prior to surgery.
Can This Injury or Condition Be Prevented?
Regular physical activity can benefit your physical, mental, and social health. It also can prevent or improve osteoarthritis. Activity also may reduce your risk for many chronic conditions, such as heart disease, diabetes, obesity, depression, and some cancers. Physical therapists are experts in movement. Some ways that a physical therapist can help you prevent knee OA include:
Developing an appropriate exercise program. Lack of physical activity is a major contributor to many health problems, including knee OA. By strengthening the muscles around the knee and surrounding joints, you can help decrease stress on your knee. Exercises to improve flexibility can help you maintain knee movement and healthy knee cartilage. Your physical therapist can design a personalized treatment program to improve your strength and flexibility.
Weight loss. Research has shown that people who are overweight have higher rates of knee OA than those who are not. Being overweight can increase stress on your knee joint. This contributes to the wearing away of the protective cartilage and leads to knee OA. Your physical therapist can determine your fitness level, design an exercise program for you, and recommend possible lifestyle changes. They also can refer you to another health care provider, such as a dietician, for further guidance.
Modifying activities. Often, people can unknowingly do activities in inefficient ways. This puts added stress on the body, including the knee joint. Your physical therapist can teach you better ways to move that reduce stress on your body and your knees.
Taking a "whole body" approach to movement. Lack of strength, mobility, and flexibility in areas such as the ankle, hip, and spine also can affect the knee. Taking care of these areas is important to help prevent knee OA. Your physical therapist will work with you to help ensure your whole body moves correctly.
What Kind of Physical Therapist Do I Need?
All physical therapists are prepared through education and experience to treat conditions such as knee OA. However, when choosing your physical therapist you may want to consider:
- A physical therapist who is experienced in working with people who have knee OA or have had knee replacement surgery. Some physical therapists have a practice with an orthopedic or geriatric focus.
- A physical therapist who is a board-certified clinical specialist or who completed a residency or fellowship in orthopedic or geriatric physical therapy. This physical therapist has advanced knowledge, experience, and skills that may apply to your condition.
- If the physical therapist's clinic accepts your health care plan. You have the right to choose any physical therapist in your state who participates in your health care plan.
You can search for physical therapists in your area who have these and other credentials by using Find a PT, an online tool built by the American Physical Therapy Association.
General tips when looking for a physical therapist (or any other health care provider) include:
- Get recommendations from family, friends, or other health care providers.
- Ask about the physical therapists' experience in helping people with knee OA.
- Be prepared to describe your symptoms in as much detail as possible. Bring a list and description of any activities that make your symptoms worse.
Other Arthritis Resources
- Arthritis: Find a Community-Based Physical Activity Program.
- Online health center for people with arthritis.
- Physical Therapy Guide to Rheumatoid Arthritis.
- Community-based physical activity programs or people with arthritis.
Additionally, the American Physical Therapy Association launched a national campaign to raise awareness about the risks of opioids and the safer alternative of physical therapy for long-term pain management. Learn more at our Safe Pain Management page.
Physical therapists use the latest evidence to design treatment plans for each person's needs, challenges, and goals to improve mobility, manage pain and other chronic conditions, and recover from and prevent injury and chronic disease. Patients also should have access to the latest evidence to improve their understanding of their disease and the importance of self-management.
The American Physical Therapy Association believes that consumers should have access to information that can:
- Help them make health care decisions.
- Prepare them for a visit with their health care provider.
The following articles provide some of the best scientific evidence for the treatment of knee OA. The articles report recent research and give an overview of the standards of practice both in the United States and internationally. They link either to a PubMed* abstract or to the free full text, so that you can read it or print out a copy to bring with you to your health care provider.
American Academy of Orthopaedic Surgeons. "Management of Osteoarthritis of the Knee (Non-Arthroplasty)." Accessed January 18, 2023. https://www.aaos.org/globalassets/quality-and-practice-resources/osteoarthritis-of-the-knee/oak3cpg.pdf. Free Article
Van Doormaal MC, Meerhoff GA, Vliet Vlieland TP, Peter WF. A clinical practice guideline for physical therapy in patients with hip or knee osteoarthritis. Musculoskeletal Care. 2020;18(4):575–595. Article Summary in PubMed
Brosseau L, Taki J, Desjardins B, et al. The Ottawa panel clinical practice guidelines for the management of knee osteoarthritis; part two: strengthening exercise programs. Clin Rehabil. 2017;31:596–611. Article Summary in PubMed
Lespasio MJ, Piuzzi NS, Husni ME, et al. Knee osteoarthritis: a primer. Perm J. 2017;21:16–183. Article Summary in PubMed
McMurray M, Bruneau M, Feldman K, et al. Knee osteoarthritis. American Physical Therapy Association website. Accessed January 18, 2023. Article from APTA
Deshpande BR, Katz JN, Solomon DH, et al. Number of persons with symptomatic knee osteoarthritis in the US: impact of race and ethnicity, age, sex, and obesity. Arthritis Care Res (Hoboken). 2016;68:1743–1750. Article Summary in PubMed
Bhatia D, Bejarano T, Novo M. Current interventions in the management of knee osteoarthritis. J Pharm Bioallied Sci. 2013;5(1):30–38. Article Summary in PubMed.
*PubMed is a free online resource developed by the National Center for Biotechnology Information. PubMed contains millions of citations to biomedical literature, including citations in the National Library of Medicine's MEDLINE database.
Expert Review:
Sep 18, 2022
Revised:
Sep 18, 2022
Content Type: Guide
Osteoarthritis of the Knee
PT, DPT, board-certified clinical specialist in sports physical therapy
Sierra Downum-Meyers
PT, DPT
Kenneth Miller
PT, DPT, board-certified clinical specialist in geriatric physical therapy, on behalf of APTA Geriatrics, an academy of the American Physical Therapy Association
You Might Also Like...
Health Tips
5 Exercises to Reduce Knee PainJun 14, 2024
Knee pain is one of the most common reasons people seek medical treatment. Without proper treatment, it can linger for years. Physical therapy is e
Health Tips
Arthritis: Find a Community-based Physical Activity ProgramJan 16, 2024
Regular physical activity can benefit your physical, mental, and social health, and prevent or improve many chronic conditions. These community-based physical
Health Tips
5 Ways to Help Manage OsteoarthritisOct 17, 2023
Osteoarthritis, or OA, is a degenerative joint disease that causes pain and stiffness and can lead to limited function. Knee OA is the most common type.


