Physical Therapy Guide to Medial Collateral Ligament Injury
The medial collateral ligament is the most commonly damaged ligament in the knee. The MCL can be sprained or torn as a result of a blow to the outer side of the knee. An MCL injury also can occur when twisting the knee, or by quickly changing directions while walking or running. MCL injury most often occurs in athletes, although nonathletes can also be affected. Physical therapists treat people with an MCL sprain or tear to reduce pain, swelling, stiffness, and any related weakness.
Physical therapists are movement experts. They improve quality of life through hands-on care, patient education, and prescribed movement. You can contact a physical therapist directly for an evaluation. To find a physical therapist in your area, visit Find a PT.
What Is an MCL Injury?
The medial collateral ligament is a small, thick band of tissue on the inner side of the knee joint. It connects two bones — the thighbone and the shin bone — preventing the knee from bending inward toward the other knee. When the knee is hit on the outer side of the leg, or if the knee is twisted violently, the MCL can overstretch, causing a partial or complete tear. MCL injuries commonly occur in football players who get "clipped" or hit on the outer side of the knee. Other causes may include twisting and turning while skiing, blows received on the soccer field, trauma from a car accident, or turning the knee sharply while the foot is planted on the ground. Healing times vary depending on each person and on the severity of the injury.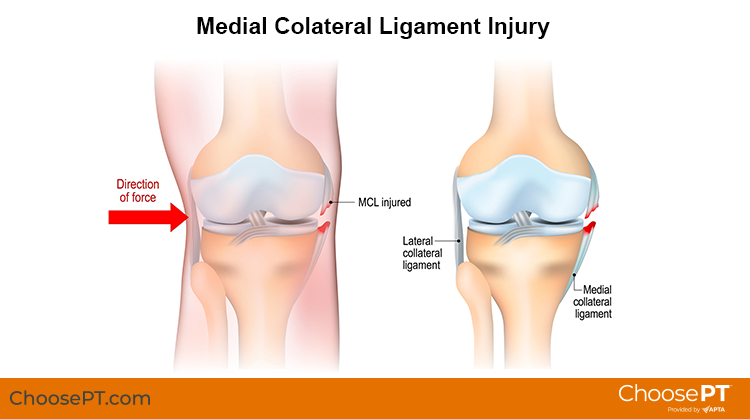
How Does It Feel?
When you experience an MCL injury, you may have:
- Pain on the inner side of the knee.
- Swelling and bruising at the inner side of the knee.
- Swelling that spreads to the rest of the knee joint in one or two days following injury.
- Stiffness in the knee.
- Difficulty or pain when trying to bend or straighten the knee.
- An unstable feeling, as though the knee may give out or buckle.
- Pain or difficulty walking, sitting down, rising from a chair, or climbing stairs.
Signs and Symptoms
With an MCL injury, you may experience:
- A "popping" sound as the injury occurs.
- Pain and swelling in your knee.
- Difficulty moving your knee.
- Difficulty bearing weight on your leg to get up from a chair or walk.
How Is It Diagnosed?
If you see your physical therapist first, they will conduct a thorough evaluation that includes taking your health history. Your physical therapist will also ask you detailed questions about your injury, such as:
- Did you feel pain or hear a "pop" when you injured your leg?
- Did you turn your leg with your foot planted on the ground?
- Did you change direction quickly while running?
- Did you receive a direct hit to the leg while your foot was planted on the ground?
- Did you see swelling around the knee in the first two to three hours following the injury?
- Does your knee feel like it’s buckling or giving way when you try to use it?
Your physical therapist also will perform special tests to help determine if you have an MCL injury. They will gently press on the outside of your knee while it is slightly bent and fully straight to test the strength of your MCL. Your physical therapist also will check the inner side of your knee for tenderness. They will measure the area for any swelling and may use more tests to see if other parts of your knee are injured. They also will observe how you walk.
To reach a diagnosis, your physical therapist may team with an orthopedic doctor or other health care provider. The doctor may order further tests, such as an MRI, to confirm the diagnosis and to rule out other damage. An MRI is not needed in all cases but may be ordered to see if surgery is required. Your physical therapist or doctor may recommend devices such as a knee brace to keep your knee from bending. They also may have you use crutches to reduce pain.
How Can a Physical Therapist Help?
Your physical therapist will work with you to design a treatment program that will speed your safe recovery. This program will include exercises and treatments that you can do at home. Physical therapy will help you return to your normal lifestyle and activities.
First 24 to 48 Hours
Your physical therapist may advise you to:
- Rest your knee and avoid walking or any activity that causes pain. They may recommend using crutches and a knee brace to reduce further strain on your MCL when walking.
- Apply ice packs to the area for 15 to 20 minutes every two hours.
- Wrap the area with an elastic bandage for compression.
- Consult with a doctor for further services, such as medication or diagnostic tests.
Your physical therapist can also help you:
Reduce Pain
Your physical therapist may use different treatments and technologies to control and reduce your pain. These may include:
- Ice.
- Heat.
- Ultrasound.
- Electrical stimulation.
- Taping.
- Prescribed exercises.
- Hands-on therapy, such as massage.
Improve Motion
Your physical therapist will choose activities and treatments to help restore normal movement in your knee and leg. These might begin with passive motions that your physical therapist performs for you to gently move your leg and knee joint. Later you will progress to active exercises and stretches that you do yourself.
Improve Strength
Certain exercises will aid healing at each stage of recovery. Your physical therapist will teach you the correct exercises to steadily restore your strength and agility. They will select the right equipment and teach you how to use it to safely to improve your knee strength. Equipment may include:
- Cuff weights.
- Elastic bands.
- Weight-lifting equipment.
- Cardio-exercise equipment, such as treadmills or stationary bicycles.
Improve Balance
Regaining your sense of balance is important after an injury. Your physical therapist will teach you exercises to improve your balance skills.
Speed Recovery Time
Your physical therapist is trained and experienced in the right treatments and exercises to help you safely heal. They will help you return to your normal lifestyle and reach your goals faster than you are likely to do on your own. Healing time will depend on how severe your injury is and which tissues are injured.
Return To Activities
Your physical therapist will discuss your specific goals with you. They will use your goals to create a plan and treatment program for your return to work, sport, and home life. Your treatment program will help you reach your goals in the safest, fastest, and most effective way possible. Your physical therapist will apply hands-on therapy, such as massage. They also will teach you exercises, work-retraining activities, and sport-specific techniques and drills to help you achieve your goals.
Prevent Future Injury
Your physical therapist can recommend a home-exercise program to continue on your own. This program will help you strengthen and stretch the muscles around your knee, upper leg, and core muscles to help prevent future injury.
If Surgery Is Necessary
Surgery is rarely needed for an MCL injury. If you do have surgery, your physical therapist will guide you through a recovery program over several weeks such as described above. They will help you minimize pain, regain motion and strength, and return to normal activities as safely and quickly as possible.
Can This Injury or Condition Be Prevented?
To help prevent a recurrence of your MCL injury, your physical therapist may advise you to:
- Avoid letting your knees collapse in toward each other when jumping, running, or turning quickly.
- Practice balance and agility exercises and drills.
- Always warm up before starting a sport or heavy physical activity.
- Follow a consistent strength and flexibility program to maintain good physical conditioning, even in a sport's off-season.
- Wear shoes that are in good condition and fit well.
What Kind of Physical Therapist Do I Need?
All physical therapists are prepared through education and experience to treat MCL injury. However, you may want to consider:
- A physical therapist who is experienced in treating people with orthopedic injuries. Some physical therapists have a practice with an orthopedic focus.
- A physical therapist who is a board-certified clinical specialist or who has completed a residency or fellowship in orthopaedic or sports physical therapy. This physical therapist has advanced knowledge, experience, and skills that may apply to your condition.
You can find physical therapists who have these and other credentials by using Find a PT, the online tool developed by the American Physical Therapy Association to help you search for physical therapists with specific clinical expertise in your geographic area.
General tips when you're looking for a physical therapist (or any other health care provider):
- Get recommendations from family, friends, or other health care providers.
- When you contact a physical therapy clinic for an appointment, ask about the physical therapists' experience in helping people who have your type of injury.
- Be prepared to describe your symptoms in as much detail as possible, and say what makes your symptoms worse.
The American Physical Therapy Association believes that consumers should have access to information that could help them make health care decisions and also prepare them for their visit with their health care provider.
The following articles provide some of the best scientific evidence related to physical therapy treatment of MCL injury. The articles report recent research and give an overview of the standards of practice both in the United States and internationally. The article titles are linked either to a PubMed* abstract of the article or to free full text, so that you can read it or print out a copy to bring with you to your health care provider.
Kim C, Chasse PM, Taylor DC. Return to play after medial collateral ligament injury. Clin Sports Med. 2016;35(4):679–696. Article Summary in PubMed.
Loghmani MT, Warden SJ. Instrument-assisted cross fiber massage increases tissue perfusion and alters microvascular morphology in the vicinity of healing knee ligaments. BMC Complement Altern Med. 2013;13:240. Article Summary in PubMed.
Frommer C, Masaracchio M. The use of patellar taping in the treatment of a patient with a medial collateral ligament sprain. N Am J Sports Phys Ther. 2009;4(2):60–69. Article Summary in PubMed.
Hunt SE, Herrera C, Cicerale S, et al. Rehabilitation of an elite olympic class sailor with MCL injury. N Am J Sports Phys Ther. 2009;4(3):123–131. Article Summary in PubMed.
Edson CJ. Conservative and postoperative rehabilitation of isolated and combined injuries of the medial collateral ligament. Sports Med Arthrosc. 2006;14(2):105–110. Article Summary in PubMed.
Azar FM. Evaluation and treatment of chronic medial collateral ligament injuries of the knee. Sports Med Arthrosc. 2006;14(2):84–90. Article Summary in PubMed.
Fung DT, Ng GY, Leung MC, Tay DK. Effects of a therapeutic laser on the ultrastructural morphology of repairing medial collateral ligament in a rat model. Lasers Surg Med. 2003;32(4):286–293. Article Summary in PubMed.
Reider B. Medial collateral ligament injuries in athletes. Sports Med. 1996;21(2):147–156. Article Summary in PubMed.
Paletta GA, Warren RF. Knee injuries and Alpine skiing: treatment and rehabilitation. Sports Med. 1994;17(6):411–423. Article Summary in PubMed.
*PubMed is a free online resource developed by the National Center for Biotechnology Information. PubMed contains millions of citations to biomedical literature, including citations in the National Library of Medicine’s MEDLINE database.
Expert Review:
Jul 19, 2020
Revised:
Jul 19, 2020
Content Type: Guide
Medial Collateral Ligament Injury
PT, DPT
Andrea Avruskin
PT, DPT
James E. Zachazewski
PT, DPT, board-certified clinical specialist in sports physical therapy, on behalf of the Academy of Sports Physical Therapy
You Might Also Like...
Health Tips
Tips to Prevent Skiing-Related Knee InjuriesSep 30, 2018
The most common skiing injuries happen to the lower limb, most commonly the knee. These tips from physical therapist can reduce your risk of being
Video
Preventing Injuries in Youth Soccer PlayersOct 13, 2016
Skye Donovan, PT, PhD, discusses common injuries that affect youth soccer players and how to prevent them.
Patient Stories
Physical Therapist 'Helped To Put Me Back Together Again'Dec 7, 2015
"Without her encouragement, and my support at home, I could not have done this."


